Introduction
The treatment landscape of advanced prostate cancer continues to evolve, particularly over the last 5+ years. Although there are several treatment options, including both ADT-based doublet and triplet combinations, available for men with metastatic hormone sensitive prostate cancer (mHSPC) that have showed an OS benefit versus ADT alone, there remain several unaddressed questions. First, among the available options, which is to be preferred and for whom: head-to-head trials assessing treatment options are unavailable. There are many reasons for this, including the time involved for these trials to accumulate an appropriate event rate for OS outcomes, and the fact that the majority of these trials are industry-sponsored. As such, investigators have relied on unique statistical methods (such as network meta-analyses) and real-world observations to guide treatment planning in the setting of several efficacious treatment options. Second, real world studies have shown relatively poor uptake of these treatments with proven life-prolonging benefit. Third, despite the improvements seen with these studies, mCSPC remains a life-limiting diagnosis. Thus, there is a need for the development of novel treatment approaches: there are several exciting ongoing/planned clinical trials in the mHSPC disease space that will be reporting outcomes in the coming years.
Comparison of Approved Agents in mHSPC space
Given the multitude of approved agents in this disease space, multiple systematic reviews and network meta-analyses indirectly comparing the available agents have been performed. Because of a lack of head-to-head clinical trials, a network meta-analysis can be employed to perform an indirect comparison among intervention arms for trials that have the same control arm. In 2021, Mori et al. published in BJU International a network meta-analysis, which included 9 trials. The magnitude of OS benefit was greatest in those treated with abiraterone (HR: 0.83, 95% CI: 0.76-0.90), followed by enzalutamide (HR: 0.85, 95% CI: 0.73-0.99), and docetaxel (HR: 0.90, 95% CI: 0.82-0.98).1 These findings are consistent with those published by Wang et al. in JAMA Oncology who also demonstrated that abiraterone had the greatest OS benefit in mHSPC patients (HR:0.61, 95% CI: 0.54-0.70).2 Conversely, in 2020 Sathianathen et al. demonstrated that enzalutamide was the agent with the best OS benefit in this disease space, particularly in patients with low-volume disease.3 Irrespective of the analysis performed, it appears that 2nd generation anti-androgens have superior OS benefits compared to docetaxel and have a more favorable safety profile, particularly with apalutamide.1The addition of 2nd generation anti-androgens to a standard of care regimen of ADT and docetaxel has shown OS benefits in both PEACE-1 and ARASENS. Conversely, does docetaxel addition to a regimen of ADT and a 2nd generation anti-androgen improve OS? Given the lack of primary evidence evaluating this, Roy et al. recently conducted an updated network meta-analysis following the publication of these two trials evaluating triplet therapy, with 11 total trials included. When compared to the combination of ADT and a 2nd generation anti-androgen, triplet therapy with docetaxel had a nonsignificant OS benefit (HR: 0.89, 95% CI: 0.68-1.16), while ADT plus docetaxel (HR: 1.16, 95% CI: 0.94-143) and ADT alone (HR: 1.46, 95% CI: 1.30-1.64) had inferior OS outcomes. In a Bayesian analysis with results presented using P-score ordering, the triplet was the most effective treatment strategy (P score= 0.936) followed by ADT plus novel hormonal therapy (P score= 0.704).4
Real-world Utilization of Novel Agents
With the emergence of multiple combination treatment strategies in the mHSPC disease space, ADT monotherapy +/- a first generation anti-androgen is no longer standard of care in the first line setting for patients presenting with mHSPC, regardless of tumor burden. As one would expect, however, the uptake of such agents in the real world has been less than ideal, with several studies examining utilization of treatment options for men with mHSPC.- Analysis of an IQVIA claims-based dataset of 17 million cancer patients and 10,000 providers across the United States was presented at AUA 2021. This demonstrated that utilization of 2nd generation anti-androgens in 2021 has remained low at 30% of all eligible mHSPC patients. Utilization of chemotherapy amongst medical oncologists has decreased from 33% of eligible patients in 2016 to 12% in 2021. This analysis also demonstrated that uptake of guidelines-recommend treatment for mHSPC patients has been significantly slower amongst urologists, compared to medical oncologists.
- Among 3,556 Canadian men with mHSPC older than 66 years of age, the majority of patients (78.6%) were treated with only a conventional ADT regimen, whereas only 11.2% of men received treatment intensification with docetaxel, and 1.5% received abiraterone acetate + prednisolone. In this study, the median survival amongst the whole population was 18 months (IQR 10-31 months).5
- Presented at the ASCO 2022 annual meeting, Freedland and colleagues assessed reasons behind the lack of treatment intensification for men with mHSPC using data from US academic/community practices. In the first-line setting, most patients received ADT ± NSAA alone (69%), while treatment intensification rates with ADT + novel hormonal therapy (26%) or ADT + chemotherapy (4%) were low. Following the initial treatment course, an additional 166 patients (27%) received subsequent treatment intensification while still castration-sensitive, prior to progression to castration resistant disease.

The top 5 reasons cited why physicians did not provide their patients with initial novel hormonal therapy were concerns regarding drug tolerability (38%), lack of clinical trial evidence of overall survival improvement (31%), lack of reimbursement (26%), patient financial constraints (20%), and questions about sequencing novel hormonal therapies earlier as compared to later in disease (21%).
- Using the Flatiron Health Electronic Health Record database, Swami et al. reported that among men with metastatic newly diagnosed prostate cancer, the majority of patients (54%) received only ADT therapy. Among patients treated with a novel hormonal therapy, an alternate novel hormonal therapy was the most common next therapy and was associated with improved median overall survival over docetaxel: abiraterone followed by docetaxel versus enzalutamide (8.7 versus 15.6 months; adjusted HR 1.32, p = 0.009) and enzalutamide followed by docetaxel versus abiraterone (9.7 versus 13.2 months, adjusted HR 1.40, p = 0.009).6
Upcoming Trials
There continues to be an influx of trials of novel agents in the mHSPC disease space. The combination of darolutamide and ADT is being evaluated in two studies: ARANOTE and ARASEC. ARANOTE is an international, multicenter, randomized, double-blind, placebo-controlled, phase 3 trial of patients with evidence of mHSPC by conventional imaging. Patients will be randomized in a 2:1 fashion to darolutamide 600 mg twice daily or placebo, plus ADT: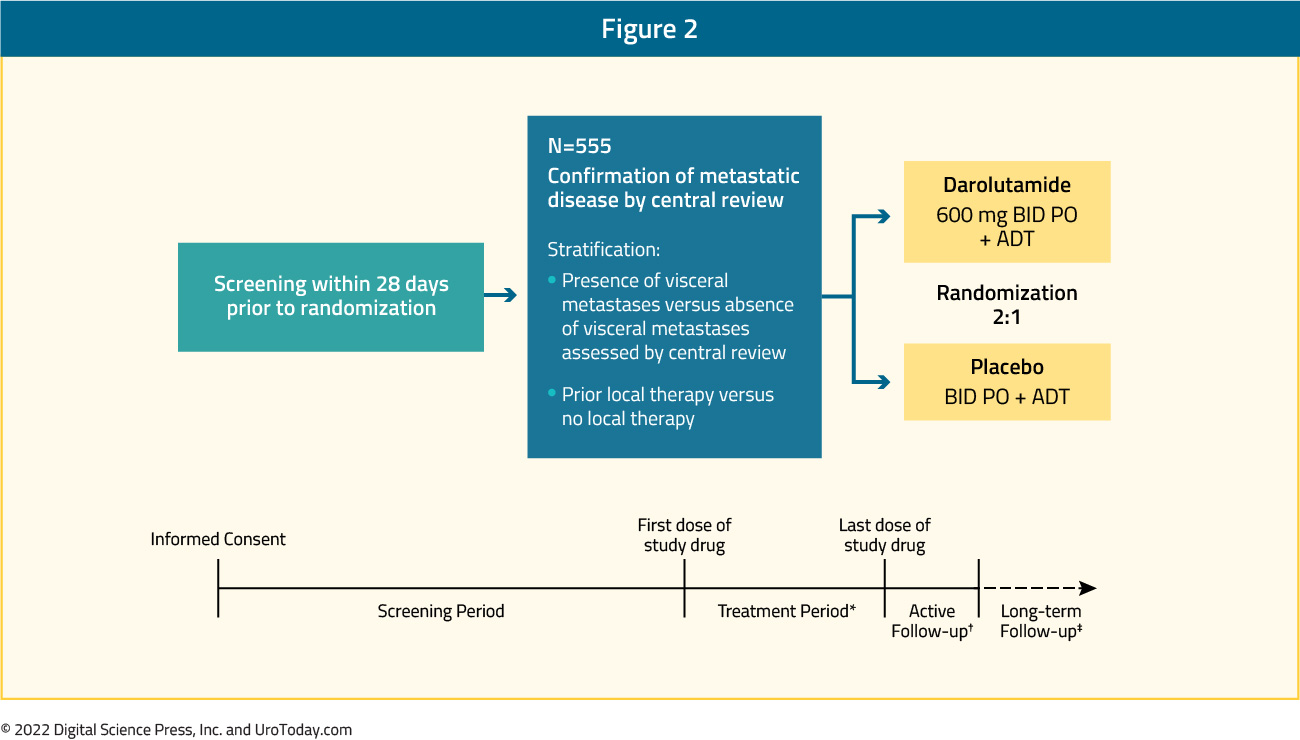
The primary endpoint is rPFS, with secondary endpoints including OS, time to CPRC, time to initiation of subsequent antineoplastic therapy, time to PSA progression, rates of undetectable PSA, time to pain progression, and safety and adverse events. Accrual started February 2021 with an expected final completion date of March 2024.
ARASEC is a US-based, phase 2, open-label, single-arm study with an external control arm. Patients with mHSPC will receive darolutamide 600 mg twice daily plus ADT. The control arm for ARASEC will be derived from the 393 patients with mHSPC treated with ADT alone in the CHAARTED trial. Patients in the active arm will be matched 1:1 to patients in the control arm using important baseline characteristics such as age, ECOG PS, extent of disease defined as low or high volume according to CHAARTED, and presence of bone and visceral metastases.
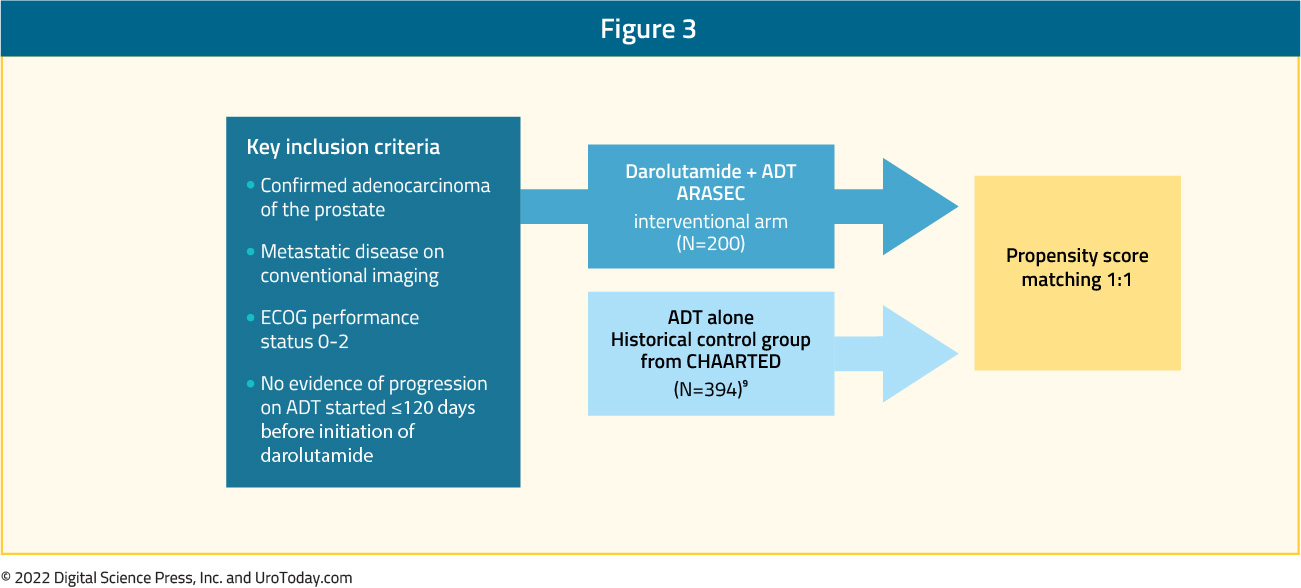
The primary endpoint is PFS, with secondary endpoints of OS, rPFS, time to CPRC, complete PSA response rate at 6 months, and safety. Accrual started November 2021 with an expected final completion date of June 2024.
Following the success of 177Lu-PSMA-617, a high-affinity prostate-specific membrane antigen (PSMA)-targeted radioligand therapy, in the mCRPC space with the VISION7 and TheraP8 trials, attempts have been made to move this drug further forward in the prostate cancer disease spectrum. One such disease space is first line mCSPC. The PSMAddition trial (NCT04720157) is an international, prospective, open label, randomized, phase 3 trial in adults with mHSPC. To be eligible, patients must have PSMA-positive disease (determined by [68Ga]Ga-PSMA-11 PET/CT) and be treatment-naïve or minimally treated candidates for hormonal therapy. A target of approximately 1,126 patients will be randomized in a 1:1 fashion to receive 177Lu-PSMA-617 (7.4 GBq i.v. every 6 weeks, ≤6 cycles) plus standard of care or standard of care alone (control arm). In this context, standard of care is second generation anti-androgen and ADT.
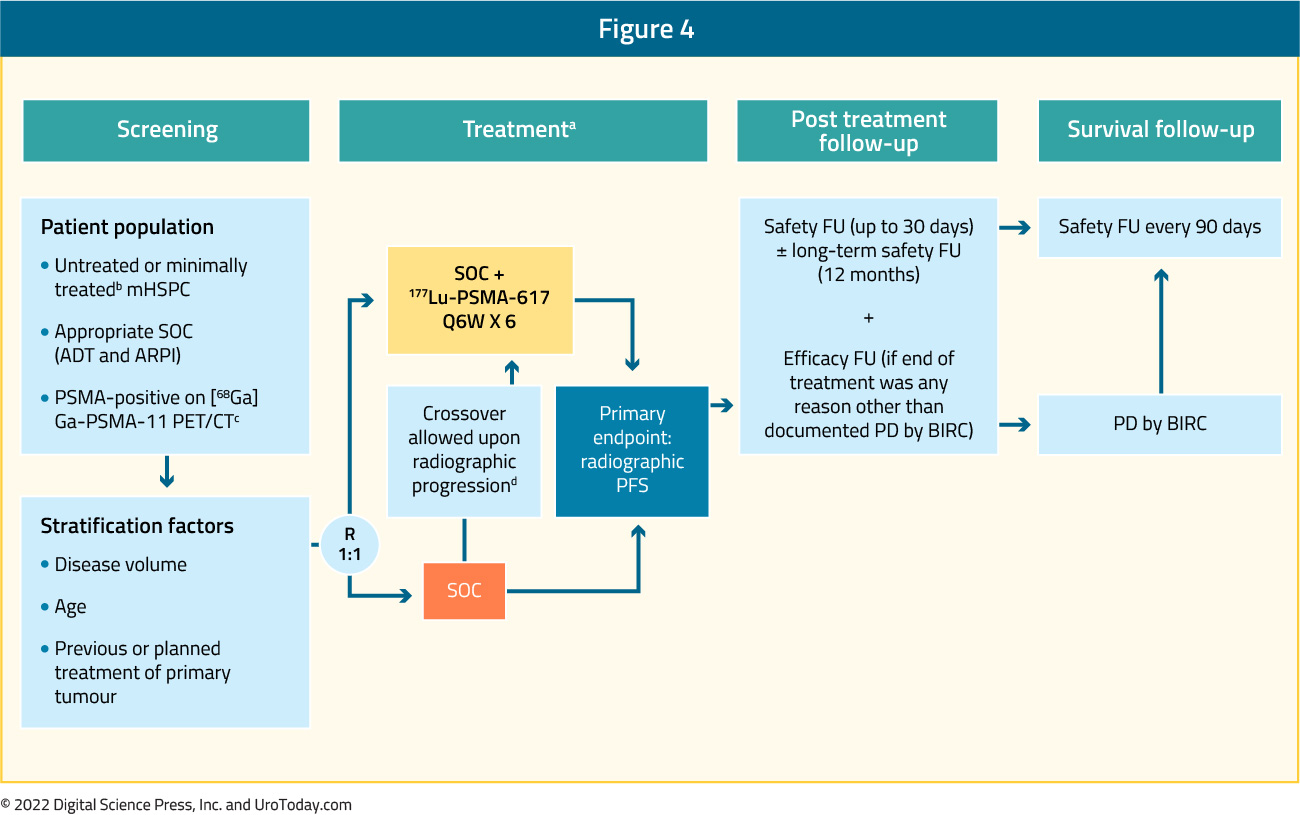
The primary endpoint is rPFS, as assessed by blinded independent centralized review. Upon centrally confirmed radiographic progression, participants in the control arm can cross over to the 177Lu-PSMA-617 arm. The key secondary endpoint is overall survival, for which final analysis will occur at approximately 384 deaths. The first patient was enrolled on trial on June 9, 2021, and currently 19 countries are participating in North America, Europe, and Asia. The estimated study completion date is December 2025.
Similarly, with the success of poly (ADP-ribose) polymerase (PARP) inhibitors in mCRPC patients with altered homologous recombination repair (HRR)/DNA damage response (DDR) genes, studies have been designed to evaluate the efficacy of these agents in the mHSPC disease space. TALAPRO-3 (NCT04821622) is a phase III, double-blind, randomized trial that will compare the combination of talazoparib plus enzalutamide versus placebo plus enzalutamide in men with mHSPC with DDR/HRR alterations.
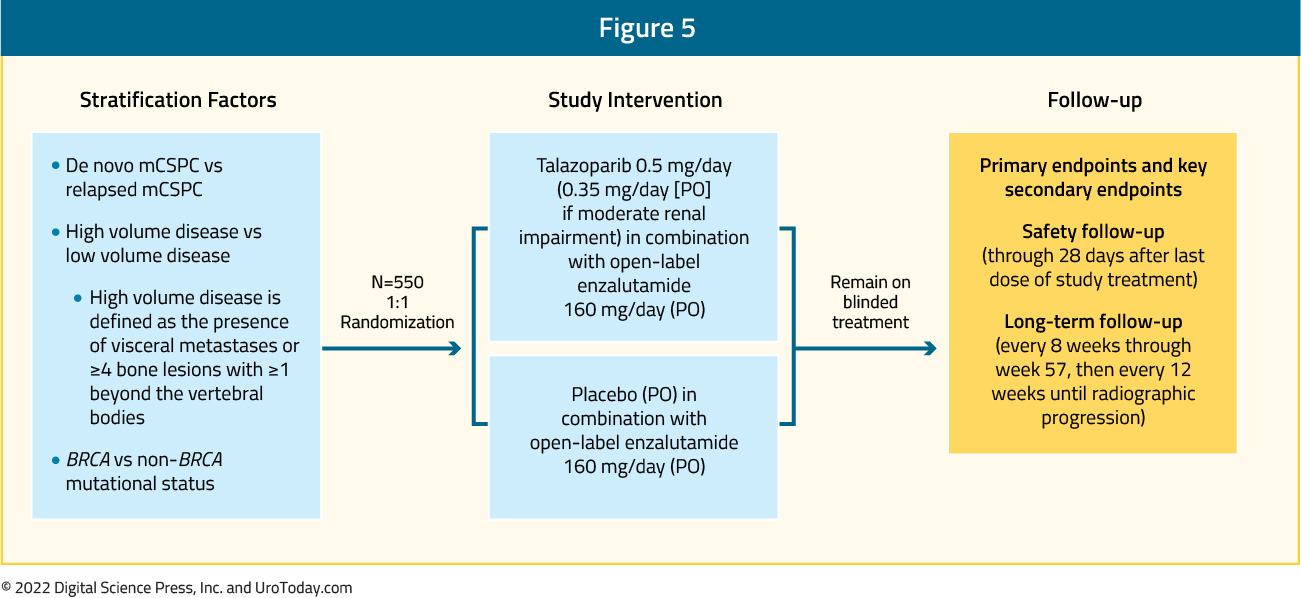
A Phase II study of talazoparib monotherapy (TALAPRO-1) demonstrated robust antitumor activity in men with heavily pretreated, HRR-mutated mCRPC.9 Androgen receptor blockade downregulates HRR gene regulation, which has been hypothesized to induce a “BRCAness” phenotype. PARP inhibition is also expected to increase sensitivity to androgen receptor-directed therapies. Thus, it is hypothesized that the combination of talazoparib and enzalutamide could be synergistic. Approximately 550 patients with mHSPC harboring DDR/HRR alterations will be randomized to talazoparib (0.5 mg once daily) plus enzalutamide (160 mg once daily) or placebo (once daily) plus enzalutamide (160 mg once daily). Patients will have alterations in at least one of 12 DDR/HRR genes known to sensitize to PARP inhibitors (ATM, ATR, BRCA1, BRCA2, CDK12, CHEK2, FANCA, MLH1, MRE11A, NBN, PALB2, RAD51C). The primary endpoint is rPFS. Secondary endpoints include overall survival, safety, and patient-reported outcomes. Study start date was May 2021 with an estimated primary completion date of December 2024.
The ZZFIRST trial, based in Spain, is a multicenter, open-label, randomized, investigator-initiated phase 2 clinical trial of patients with mHSPC. Patients will begin treatment with enzalutamide 160 mg/day for two 28-day cycles in addition to standard ADT. Following this initial lead-in period, patients are then randomized and stratified based on homologous recombination gene alterations on a 1:2 ratio to either continue enzalutamide 160 mg/day or to receive enzalutamide 160 mg/day plus talazoparib 0.5 mg/day. In both arms, patients will continue ADT throughout the trial. Treatment will continue until progressive disease or unacceptable toxicity.
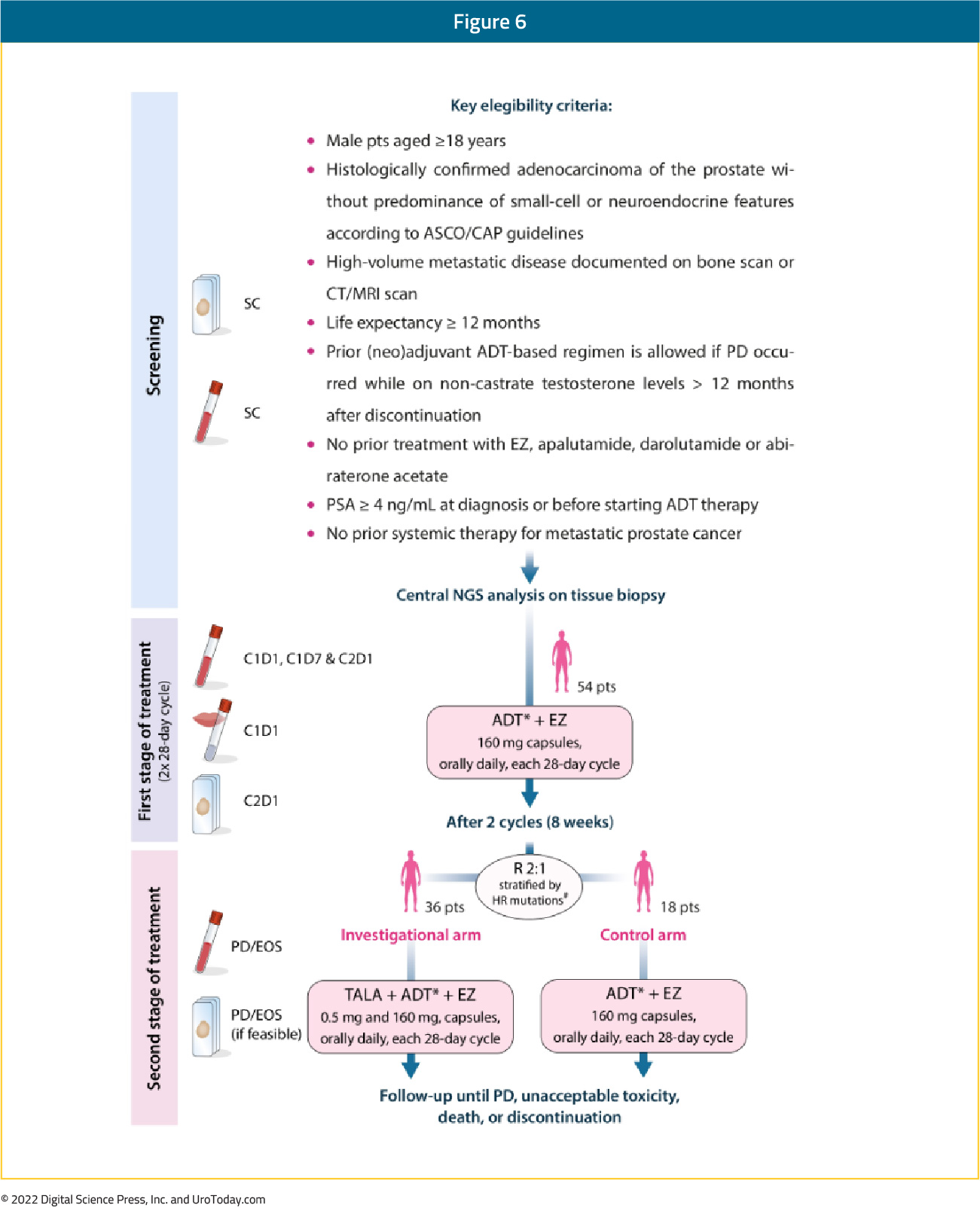
The primary study endpoint is PSA-complete response defined as the percentage of patients with PSA < 0.2 ng/mL at 12 months of therapy. Secondary endpoints include PSA response and time to development of castration resistant disease, the correlation between molecular and transcriptomic signatures with antitumor activity, the effect of enzalutamide and ADT on DNA repair function, and the safety and tolerability of the combination treatment approach. This trial was opened to accrual in July 2020 at 9 sites in Spain. As of December 2021, 48 patients have been enrolled and are receiving study treatment of a targeted 54 participants.
Finally, the SAABR trial is a single arm phase II trial that will evaluate abiraterone + atezolizumab + GnRH analog with SBRT in patients with mHSPC. Preclinical studies have shown that SBRT can induce an immunogenic effect through enhanced expression of the PD-L1 protein on tumor and immune cells. Furthermore, outcomes in subjects with locally advanced disease enrolled on STAMPEDE suggest that prostate radiation therapy may be associated with a reduction in treatment failure. Atezolizumab will be administered to men with newly diagnosed mHSPC by IV infusion (1200 mg IV over 60 minutes every 3 weeks) followed after Cycle 1 by abiraterone acetate (1000 mg PO every day with prednisone 5 mg daily), ADT (GnRH analog), and SBRT (7.25-7.50 Gy x 5 fractions to prostate and seminal vesicles every other day starting at Cycle 5 Day 1 ± 5 days) until unacceptable toxicity, protocol defined progression, or 2 years of treatment. Atezolizumab will be continued for a maximum of 2 years. Continuation of abiraterone acetate and ADT beyond 2 years is at the discretion of the treating physician per local standard of care. The study schema for SAABR is as follows:

The primary objective is failure-free rate at 2 years, with failure defined as biochemical failure, radiographic progression, or death from any cause. Secondary objectives include symptomatic skeletal events defined as a symptomatic fracture (surgery or radiation to the bone or spinal cord compression), prostate cancer specific survival, OS, and safety/tolerability.


