
The incidence of metastatic prostate cancer at diagnosis ranges from ~5-50%, with significant geographic differences as previously described.2 Such patients are defined as having de novo or synchronous mHSPC. Additionally, there exists a subset of men initially diagnosed with non-metastatic disease, many of whom have received prior definitive local treatment, who will have progression to a metastatic state prior to development of castration resistance. This is known as metachronous mHSPC. This distinction between synchronous (i.e. de novo) and metachronous presentations is of utmost clinical importance given the known differences in underlying genomic mutational profiles and prognoses, influencing the subsequent choice of treatment intensification.3,4 These two cohorts can be further subdivided based on the volume of metastatic disease at presentation: low and high volumes. The CHAARTED high-volume criteria have been widely adopted in clinical practice, with high volume patients defined as follows: presence of visceral metastases or ≥4 bone lesions with ≥1 beyond the vertebral bodies and pelvis.5
As such four distinct subgroups become clinically relevant (median overall survival per CHAARTED and GETUG-15 among men receiving ADT alone, ie. the control groups in these trials):
- Synchronous and high volume: 3 years
- Synchronous and low volume: 4.5 year
- Metachronous and high volume: 4.5 years
- Metachronous and low volume: ~8 years
Index Patient 4: Metachronous Low Volume mHSPC
Case Presentation: A 76-year-old male with an ECOG performance status of 1 has a known history of prostate cancer Gleason Score 7 (4+3) in 5/12 cores and had previously undergone a robotic radical prostatectomy nine years ago with evidence of cT3a disease and positive surgical margins. After the patient had achieved urinary continence 6 months post-operatively, he and his treating physician opted for adjuvant radiation therapy to the prostatic fossa. The patient was free of biochemical recurrence until 5 years ago when his PSA was noted to progressively increase with a PSA doubling time of 18 months. A shared decision between the patient and physician was taken to forgo systemic therapy with androgen deprivation therapy until there was evidence of metastatic disease. At a serum PSA level of 5.2 ng/ml, a staging work up with a Pylarify PSMA PET/CT scan demonstrated evidence of a single metastatic site at the level of the 3rd lumbar vertebra. There was no evidence of any other metastatic sites (bone or visceral) and the patient’s blood work was otherwise unremarkable.Doublet Therapy: Docetaxel + ADT
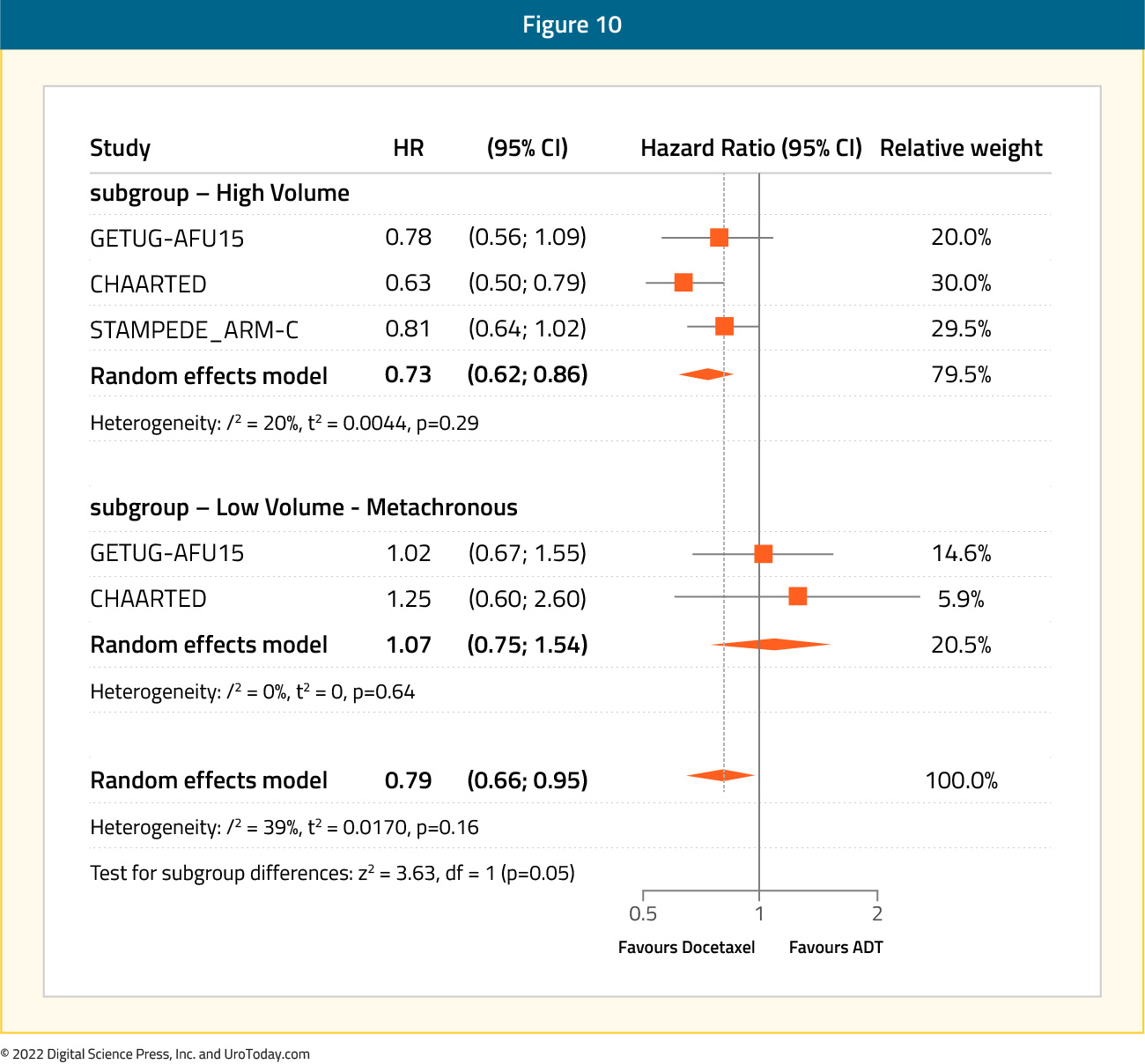
Importantly, there is consistent evidence against the use of docetaxel in this mHSPC subgroup. Results from the CHAARTED trial demonstrated a minimal overall survival in this subgroup (HR: 0.77; 95% CI: 0.51 to 1.18).5 Furthermore, results from the STOPCaP meta-analysis presented at ASCO 2022 using CHAARTED and GETUG-AFU15 data demonstrated no overall survival benefit to docetaxel addition (HR: 1.07; 95% CI: 0.75 to 1.54).
Doublet Therapy: ARAT + ADT
Subgroup analyses have consistently demonstrated an overall survival benefit to ARAT addition in patients with low volume mHSPC. Results from the ARCHES trial demonstrated a 37% improved hazard of overall survival with enzalutamide addition to ADT in patients with metachronous low volume mHSPC (HR: 0.63, 95% CI: 0.26 to 1.54).12 Analysis from the ENZAMET trial presented at ASCO 2022 demonstrated that this benefit is reflected in an improvement in 3-year overall survival from 83% to 92% on interim analysis.
Metastasis-Directed Therapy
In addition to systemic therapy with ADT + ARAT in this subgroup, there is emerging data from both ORIOLE, STOMP, and SABRC-COMET regarding the role of metastasis-directed therapy (MDT) in select patients with metachronous, oligometastatic mHSPC.
The STOMP trial was a multicenter, randomized phase II trial that prospectively evaluated the effects of MDT for patients with evidence of oligometastatic disease on choline PET/CT (up to three extracranial sites) who had received prior treatment with curative intent and had evidence of biochemical recurrence with testosterone >50 ng/ml (i.e. metachronous, oligometastatic mHSPC). Between 2012 and 2015, 62 patients were randomized 1:1 and MDT was either SBRT or metastasectomy. The primary endpoint was time to initiation of ADT (called ADT-free survival). ADT was initiated for symptoms, progression beyond three metastases, or local progression of known metastatic disease. Time to castration resistance was a secondary endpoint (called CRPC-free survival). The updated five-year results were presented at GU ASCO 2020. With a median follow up of 5.3 years, the five-year ADT-free survival was 8% in the surveillance arm compared to 34% for the MDT group (HR 0.57, 95% CI 0.38 to 0.84, log-rank p=0.06). Secondary endpoint of CRPC-free survival at 5 years was 53% in subjects under surveillance and 76% in those receiving MDT (HR 0.62, 80% CI 0.35 to 1.09).15
The ORIOLE trial was a randomized phase II trial of 54 men with metachronous, oligometastatic mHSPC (up to three sites). Metastatic sites were diagnosed via 18F-DCFPyL PET/CT. Between 2016 and 2018, patients were randomized in a 2:1 fashion to receive SABR or observation. The primary outcome was progression at 6 months, defined as serum PSA increase, progression detected by conventional imaging, symptomatic progression, ADT initiation for any reason, or death. Progression at six months occurred in 7 of 36 patients (19%) receiving SABR and 11 of 18 patients (61%) undergoing observation (p = 0.005). Treatment with SABR improved median PFS (not reached vs 5.8 months; HR 0.30, 95% CI 0.11 to 0.81).16
Recently published pooled data from the two trials demonstrates that MDT in these patients improves progression-free survival from 5.9 months (95% CI: 3.2 – 7.1) to 11.9 months (95% CI: 8.0 – 18.3; HR: 0.44, p<0.001), without any significant improvements seen in radiographic progression-free survival, time to castration-resistant disease, or overall survival.17
SABR-COMET was a randomized, open-label phase II study of patients with oligometastatic disease (up to five sites) between February 2012 and August 2016. This trial was not restricted to patients with prostate cancer and also included lung, breast, and colorectal cancer patients. Of the 99 patients in this trial, 18 (18%) had prostate cancer. After stratifying by the number of metastases (1–3 vs 4–5), patients were randomized in a 1:2 fashion to receive either palliative standard of care alone or standard of care plus SABR. In an updated analysis published in 2020 (median follow up 51 months), the five-year OS rate was 17.7% (95% CI 6-34%) in the control arm and 42.3% in the SABR arm (95% CI 28-56%, stratified log-rank p=0.006). The corresponding median OS was 28 months and 50 months, respectively.18
The following table summarizes OS outcomes by CHAARTED disease volume criteria and presentation (synchronous vs metachronous) among men with mHSPC: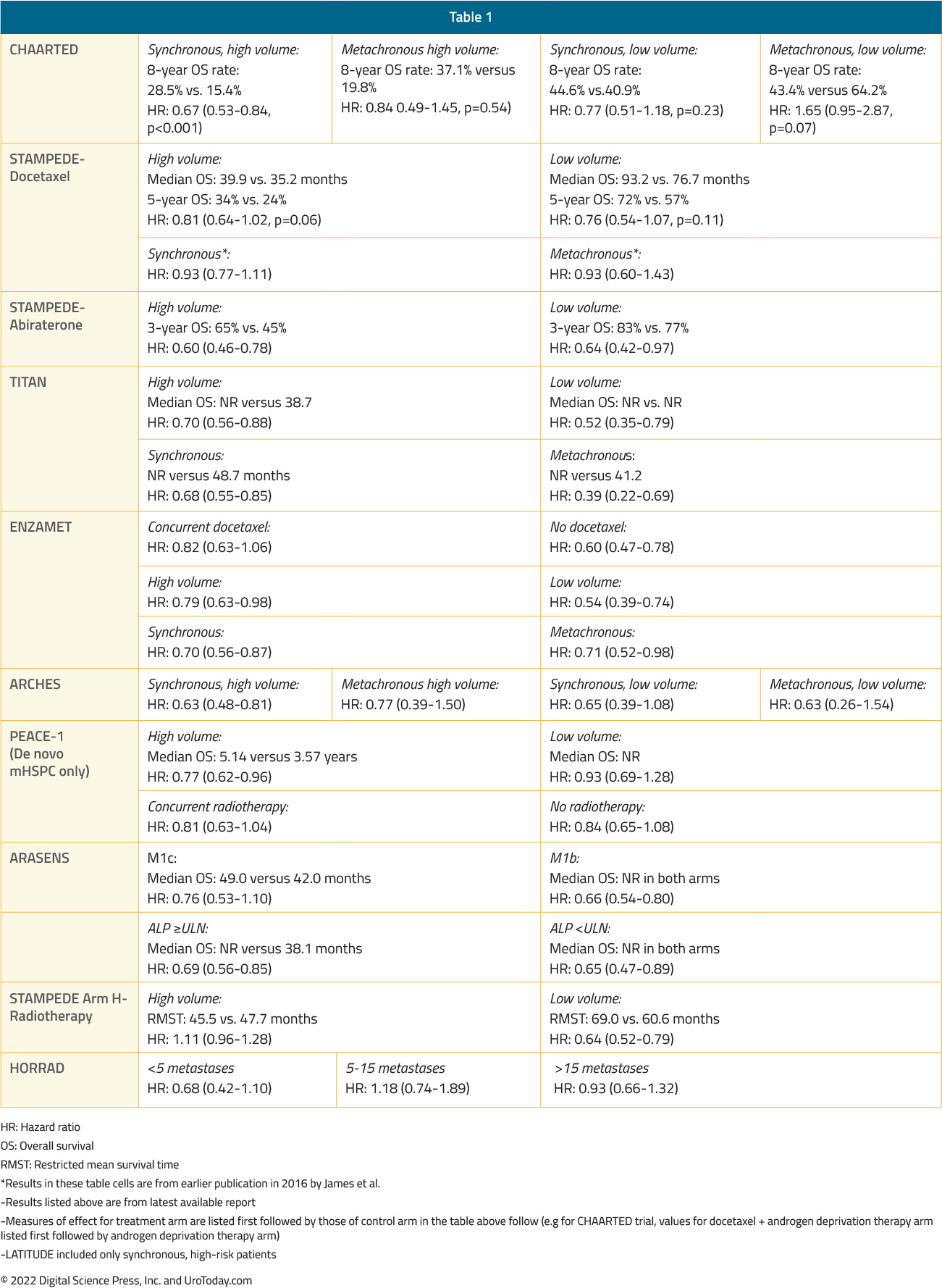
Treatment with ADT alone is no longer an adequate standard of care treatment for patients with mHSPC. Early treatment intensification with an ARAT and/or docetaxel is critical to maximize overall survival outcomes in mHSPC patients. Based on the current evidence, it appears that patients with synchronous, high volume mHSPC benefit from early treatment intensification with triplet therapy in the form of both an ARAT and docetaxel, whereas the remaining mHSPC subgroups benefit most from doublet therapy with ARAT addition to ADT. Radiotherapy to the prostate is associated with improved overall survival in mHSPC patients with synchronous, low-volume disease, whereas metastasis-directed therapy may be associated with improved outcomes in men with metachronous, oligometastatic disease.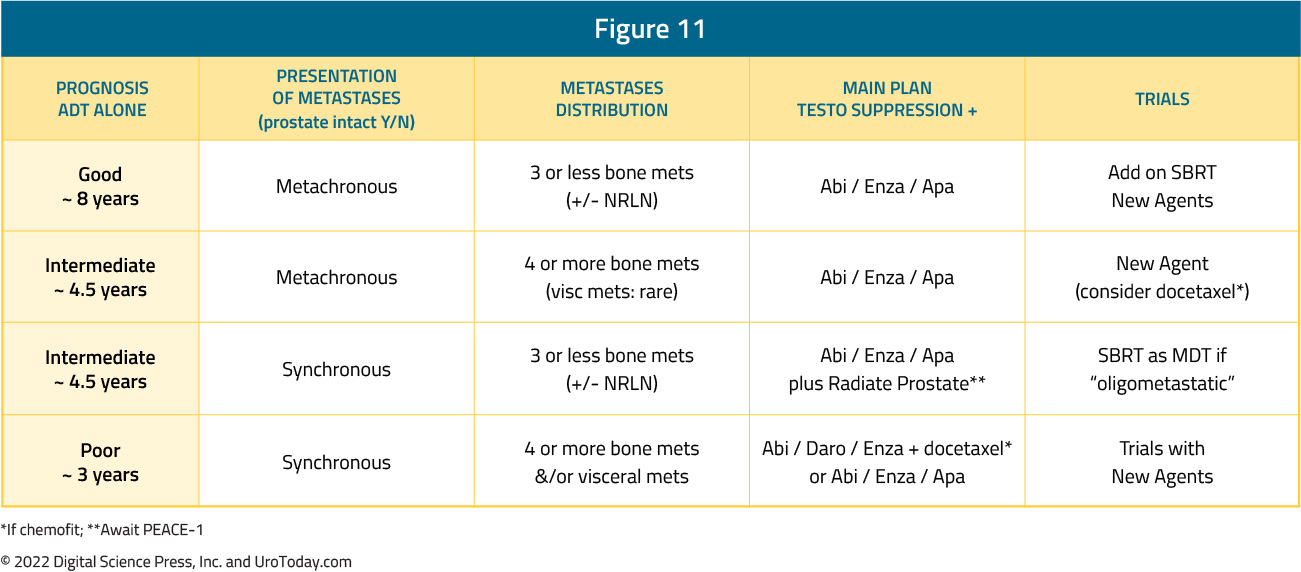
- Rashid K. Sayyid, MD, MSc, University of Toronto, Toronto, Ontario
- Zachary Klaassen, MD, MSc, Medical College of Georgia, Augusta, Georgia, USA

