Genome-wide association studies (GWAS) have aided in the discovery of more than 150 prostate-specific susceptible SNPs in men of European descent, however, significant ethnic and racial disparities in GWAS have limited the use of ethnicity-specific polygenetic risk assessments. Thanks to efforts from Haiman and coauthors discovery of genetic variants conferring African American-specific risk of prostate cancer have provided a strong impetus to evaluate ethnicity-specific polygenetic risk.1,2
The Stockholm3 test is a three-part model that incorporates pre-biopsy clinical information, multiple protein quantification (total PSA, free PSA, human kallikrein2, MSMB, MIC) and a cumulative genetic risk score derived by identifying germline SNPs validated for association with prostate cancer risk. The model was developed in a primarily Caucasian prospective cohort of approximately 60,000 men and was able to reduce the number of benign biopsies by 44% while missing no grade group 2 cancers compared to PSA screening alone.3
We know African American men have been shown to have a higher prostate-specific antigen (PSA), higher likelihood of detectable PC, and higher grade of cancer compared to Caucasian men, therefore we proposed a method of propensity score matching to account for these features of delayed presentation. Here we studied the differences in prostate cancer detection in an American cohort from Chicago and a screening cohort from Stockholm, Sweden.4
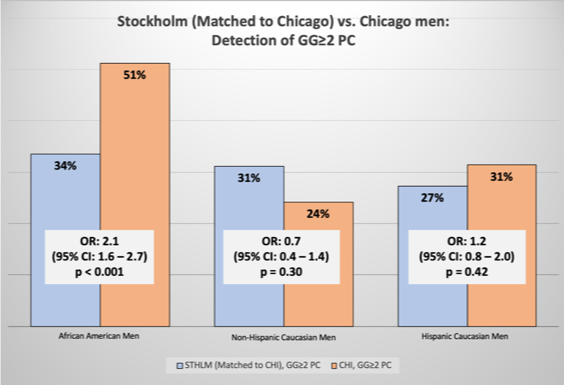
Figure 1 Comparing the odds ratio (OR) of Gleason Grade Group ≥2 prostate cancer (GG≥2 PC) detection in Chicago (CHI) men compared to Stockholm (STHLM) men eligible for propensity score (PS) matching with African American, non-Hispanic Caucasian and Hispanic Caucasian men 95% Confidence intervals (CI) with two-sided p values.
We found that despite appropriately matched PSA, age, prostate volume, prior prostate biopsy, family history of prostate cancer, and the use of 5-alpha reductase inhibitors, there was still an increased risk for prostate cancer in African American men (Figure 1). Using the matched cohorts from Stockholm we performed a secondary analysis of the Stockholm3 test and discrimination for Gleason Grade group 2 prostate cancer was maintained over PSA (Figure 2).
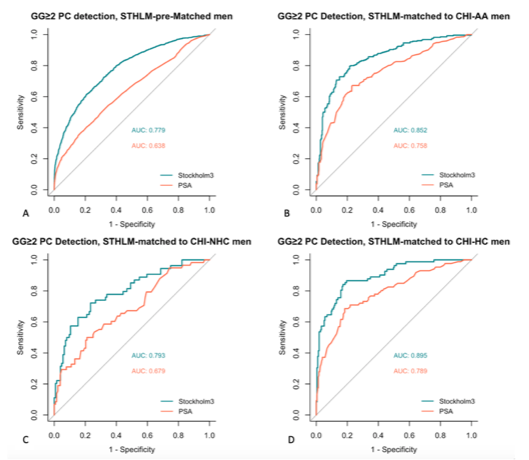
Figure 2: Comparing the area under the receiver operator curve (AUC) using PSA and the Stockholm3 test for the detection of Gleason Grade Group ≥2 prostate cancer (≥GG2 PC) and the Stockholm (STHLM) pre-matched men (A) and propensity score (PS) matched STHLM men to Chicago (CHI) African American (AA) (B), non-Hispanic Caucasian (NHC) (C), and Hispanic Caucasian (HC) men (D)
The results of this study strengthened our hypothesis that the Stockholm3 test may have utility in high-risk cohorts such as African American men. Our ongoing studies using the Stockholm3 test and ethnic-specific genetic variants aim to further elucidate differences in model calibration and prostate cancer prediction for the Stockholm3 test in African American and multiethnic men.
Written by: Hari T. Vigneswaran, Andrea Discacciati, Peter H. Gann, Henrik Grönberg, Martin Eklund, Michael R. Abern
Department of Urology, College of Medicine, University of Illinois at Chicago, Chicago, IL, 60607, USA. ., Department of Medical Epidemiology and Biostatistics, Karolinska Institutet, 171 77, Solna, Sweden., Department of Pathology, College of Medicine, University of Illinois at Chicago, Chicago, IL, 60607, USA., Department of Urology, College of Medicine, University of Illinois at Chicago, Chicago, IL, 60607, USA.
Published Date: August 17th, 2020
Read the Abstract


