What is an Indwelling Catheter?
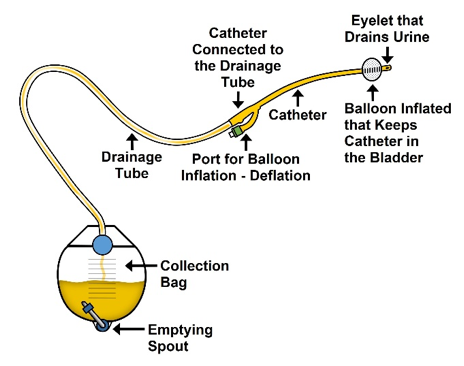
An indwelling urinary catheter (IUC), generally referred to as a “Foley” catheter, is a closed sterile system with a catheter and retention balloon that is inserted either through the urethra or suprapubically to allow for bladder drainage. External collecting devices (e.g. drainage tubing and bag) are connected to the catheter for urine collection
Indwelling urinary catheters are recommended only for short-term use, defined as less than 30 days (EAUN recommends no longer than 14 days.) The catheter is inserted for continuous drainage of the bladder for two common bladder dysfunction: urinary incontinence (UI) and urinary retention.
Two Types of Indwelling Catheters
Indwelling urinary catheters are either inserted:
- Transurethrally
- Suprapubically
Suprapubic catheterization is usually used for bladder drainage following in bladder, urethral or pelvic surgery, or following genitourinary trauma. Both methods of indwelling catheterizations are associated with complications.
In practice, transurethral catheterization is the typical approach because the procedure can be organized and managed by nurses whereas suprapubic catheterization requires a more complex procedure. However, if in place long-term, defined as more than 30 days, the insertion, changing and management are done by nurses (registered nurses, licensed practical nurses).
Transurethral Catheterization
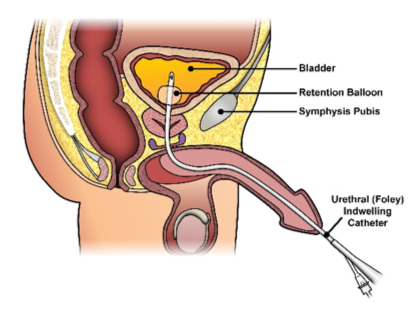
Transurethral indwelling catheterization or urinary catheterization is defined as passage of a catheter into the urinary bladder via the urethra (urethral catheter). Transurethral indwelling catheterization is also called urethral catheterization. In this site, we only use the term urethral catheterization.
Suprapubic Catheterization
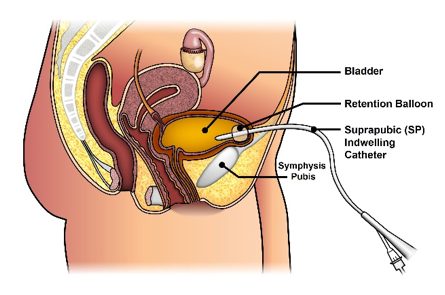
Suprapubic catheterization is the insertion of a catheter into the bladder via the anterior abdominal wall. The catheter is inserted through an incision made above the pubic bone and below the umbilicus. The insertion of this type of catheterization is done by a urologic specialist. Long term catheterization can be associated with many serious problems including urinary tract infections, urethritis, bladder spasms with pain and urinary leakage, and other bladder complications.
Use Patterns
Short Term
Short-term uses include:- Management of acute urinary retention.
- Postoperative bladder decompression following GU surgery or pelvic trauma.
- Monitoring urinary output in acutely ill patients.
Long Term & CAUTI
Long-term use, defined as greater than 30 days, is discouraged because it provides access for bacteria from a contaminated environment into a vulnerable body organ and system.
As a result, catheter-associated urinary tract infection (CAUTI) is the most common type of infection acquired in hospitals and nursing homes. At least 15% to 25% of patients may have an indwelling catheter inserted sometime during their hospital stay, with most only used for the short-term (defined as < 30 days). Prevalence is greater in high acuity patient units, with critical care and intensive care units having the highest prevalence. CAUTIs are associated with multiple complications and side effects, can lead to increased length of stays, mortality rates, and ultimately higher hospital costs.
Closed Drainage System
A closed catheter drainage system is an aseptic system in which the path from the tip of the catheter inserted into the bladder, to the bag which catches urine, is closed and should not be disconnected. This structure is designed to eliminate inoculation of the urinary tract with bacteria via the catheter drainage tubing and from the collection bag. The term ‘closed drainage’ is, however, not entirely accurate as there are often numerous portals of entry of pathogens and the system must be opened to allow emptying and be disconnected when the drainage bag is changed
This resource center provides in-depth information on the indwelling Foley catheter from the indication through the complications and prevention strategies. It also has resources that offer tools and on-demand education webinars on appropriate use of the catheters to understanding CAUTI.
Written by: Diane K. Newman, DNP, Continence Nurse Specialist
References
- Hunter KF, Bharmal A, Moore KN. Long-term bladder drainage: Suprapubic catheter versus other methods: a scoping review. Neurourol Urodyn. 2013 Sep;32(7):944-51. doi: 10.1002/nau.22356
- Newman DK, Cumbee RP, Rovner ES. Indwelling (transurethral and suprapubic) catheters. In: Newman DK, Rovner ES, Wein AJ, editors. Clinical Application of Urologic Catheters and Products. Switzerland: Springer International Publishing; 2018, 47-77.
- Newman DK. Devices, products, catheters, and catheter-associated urinary tract infections. In: Newman DK, Wyman JF, Welch VW, editors. Core Curriculum for Urologic Nursing. 1st ed. Pitman (NJ): Society of Urologic Nurses and Associates, Inc; 2017, 439-66.
- Newman DK. The indwelling urinary catheter: Principles for best practice. JWOCN. 2007;34:655-61 DOI: 10.1097/01.WON.0000299816.82983.4a
- Meddings, J, Rogers, MA, Macy, M, & Saint, S. Systematic review and meta-analysis: reminder systems to reduce catheter-associated urinary tract infections and urinary catheter use in hospitalized patients. Clin Infect Dis. 2010, 51(5), 550-60. doi: 10.1086/655133
- Weber DJ, Sickbert-Bennett EE, Brown V. & Rutala WA. Comparison of hospital wide surveillance and targeted intensive care unit surveillance of healthcare-associated infections. Infect Control Hosp Epidemiol. 2007,28(12), 1361-1366. doi: 10.1086/523868


