
Table 1 – Immune checkpoint inhibitors:
There are currently 1449 ongoing trials of immune checkpoint inhibitors in bladder cancer. This is an astoundingly high number of trials and represents the great interest and hope these drugs have caused.
Two studies that were presented in the ASCO meeting in Chicago in 2018 analyzed the effect of Pembrolizumab and Atezolizumab given as neoadjuvant therapy before radical cystectomy in pT2-T4N0 patients.
These were the PURE-01 trial (NCT 02736266)1 and the ABACUS trial (NCT 02662309)2. The phase two PURE-01 study is the preoperative Pembrolizumab before radical cystectomy for muscle-invasive bladder cancer patients: interim clinical and biomarker finding. The ABACUS study assessed the safety and efficacy of neoadjuvant Atezolizumab. In the PURE-01 study, patients were given three cycles of Pembrolizumab 200 mg and then underwent radical cystectomy. The primary endpoint was a pathological complete response, and overall 60 patients were enrolled. The results demonstrated a 40% pathological complete response rate, with downstaging occurring in 51% of patients. Grade 3 or 4 complications occurred in 5.4% of patients.
In the single-arm phase two ABACUS trial patients who were not fit or were unwilling to receive neoadjuvant cisplatin chemotherapy were given two cycles of 1200 mg of Atezolizumab and then underwent radical cystectomy. The primary endpoint was a pathological complete response. Secondary endpoints included safety and radiological response. Of the 69 patients enrolled in the trial, nine patients (12.1%) had grade 3 or 4 complications induced by Atezolizumab, and ten patients (13.5%) had surgical grade 3 or 4 complications, with one patient (1.3%) enduring treatment-related death. The pathological complete response rate was 23%.
Another similar neoadjuvant study presented at ASCO 2018 was the combination trial of Duvalumab (anti-PD-L1) and Tremelimumab anti-CTLA-4) (NCT 02812420)3. In this trial, the drug combination was given at weeks 1 and 5, and then radical cystectomy was performed at week 9-11. Overall, 12 patients were enrolled, and 6 underwent radical cystectomy. The pathological complete response rate was 50%, with no response in 17% of patients and 33% of the patients demonstrated progression.
Dr. Konety moved on to discuss the association of BCG and PD-L1. High levels pf PD-L1 have been demonstrated in Bacillus Calmette–Guérin (BCG) granulomas.4 High PD-L1 levels have been linked to BCG refractory disease. This occurs in 7% of pTa disease, 16% of pT1 disease, and 45% of carcinoma in situ (CIS) cases. The high levels of PD-L1 are also associated with stage progression. This association brought the idea of administering BCG together with an immune checkpoint inhibitor to patients with bladder cancer. Other drug combinations include two different classes of immune checkpoint inhibitors.
The studies examining the role of immune checkpoint inhibitors as neoadjuvant therapy before radical cystectomy seem promising, but naturally, we need to understand the long-term results, which are still missing. There are currently several ongoing single-arm clinical trials of immune checkpoint inhibitors in bladder cancer, as seen in table 2, and there are also several drug combination trials (Table 3). The results of these trials are eagerly awaited, as hope that the results of these trials will lead to the improvement of the outcomes of muscle-invasive and advanced metastatic bladder cancer are quite high.

Table 2- Single arm ongoing immune checkpoint inhibitor trials:
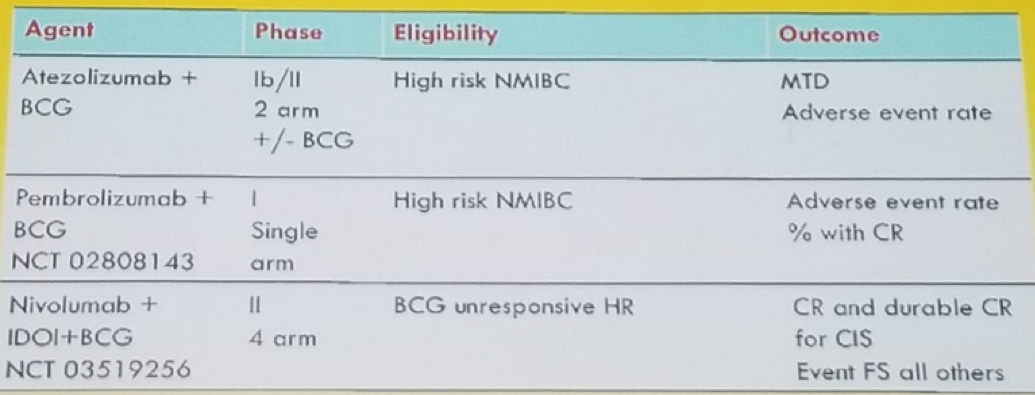
Table 3 – Ongoing trials with combination agents:
Presented by: Badrinath Konety, University of Minnesota, USA
Written By: Hanan Goldberg, MD, Urologic Oncology Fellow (SUO), University of Toronto, Princess Margaret Cancer Centre @GoldbergHanan at the Global Conference on Bladder Cancer 2018 - September 20-21, 2018 Madrid, Spain
References:
1. Necchi A et al. ASCO 2018 abstract 4507
2. Powels T et al ASCO 2018 abstract 4506
3. Gao J et al. ASCO 2018
4. Imman B et al. Cancer 2017

