The potential benefits of LND include:
- Improved survival?
- Improved staging (prognosis)
- Longer recovery
- Increased complications
There is only one randomized controlled trial (EORTC 30881 – Blom 2009) that assessed the correlation between LND and survival in these patients. There are, however, several systematic reviews that attempted to answer this question as well, and many retrospective studies with limited adjustment for biases and confounding. In the EORTC 30881 prospective randomized controlled study, 772 patients were randomized to either radical nephrectomy + LND or radical nephrectomy alone.5 The results showed no difference in survival between the two arms with a lymph node metastases rate of 4%, and similar complication rates in both arms. Although this is the best quality evidence we have, the trial was limited by a low rate of lymph node metastases, and unknown lymph node template/completion. Additionally, the surgeons were not blinded, and the LND was not standardized. Similarly, in the most recent systematic review, LND was not associated with improved mortality either.6 Lastly, in retrospective propensity score-adjusted data, LND did not improve metastases or survival rates.7 This was consistent in higher risk groups including those with clinical adenopathy.
Dr. Lavallée moved on to discuss the possible reasons for the recurring outcomes, demonstrating no survival benefit in LND. Possible reasons include the fact that the spread of RCC is unpredictable, as opposed to other cancers such as testicular cancer. Additionally, the spread is both lymphatic and hematologic. Lastly, studies of patients with node-positive disease report:
- Hilar lymph nodes skipped in 1/3 of patients
- Only 20% of positive node disease is in an ipsilateral “predictable” location
- 30% are suprahilar (increases morbidity)
- 60-70% with positive node disease have concurrent distant metastases
Figure 1 – Lymph Node-Positive Disease and its Unpredictable Spread in Various RCC Patients:
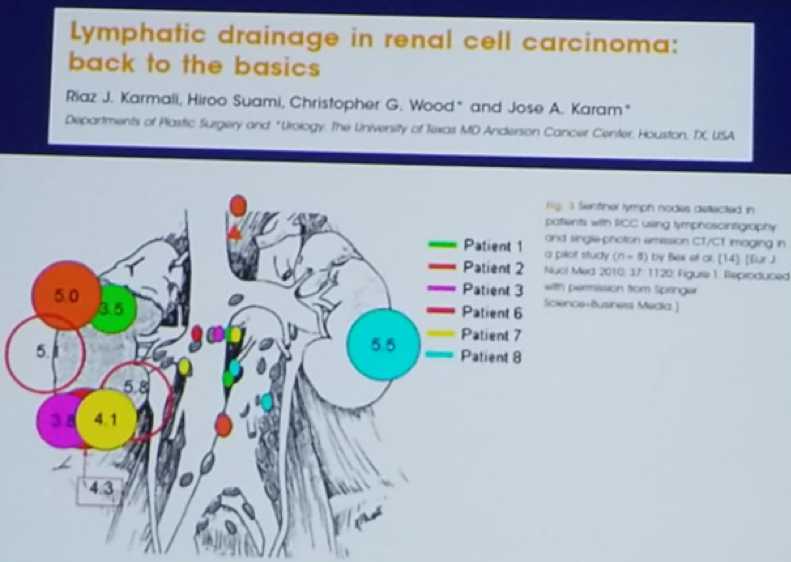
If LND does not improve survival is it still worthwhile doing? That was the next question discussed by Dr. Lavallee. The EORTC 30881 randomized controlled trial demonstrated that LND is not without complication with a significant increase in the rate of bleeding, and a two-fold increase in the rate of embolism (9.4% vs. 6.5%, and 2.2% vs. 1.1%, respectively).5 An increased rate of complications associated with LND was also shown in retrospective data.7 LND was shown to be associated with a 40% increase in complications, especially in LND performed in metastatic patients. Importantly, the reporting of complication is not performed well in most studies with a considerable rate of under-reporting. Furthermore, most studies are published by centers of excellence, with high-volume surgeons. Whether this data could be generalized to all medical centers in the community as well, is not intuitively straight forward.
Dr. Lavallee summarized his talk stating a few take-home messages:
- It is impossible to predict which patient will develop lymph node-positive disease
- It is also impossible to predict the spread of the disease
- More than 50% of patients with positive node disease have distant metastases
- LND has not been shown to improve survival.
Presented by: Luke Thomas Lavallée, Associate Scientist, Clinical, Epidemiology Program, Ottawa Hospital Research Institute
Urologic Oncologist, Division of Urology, Department of Surgery, The Ottawa Hospital, General Campus, Assistant Professor, University of Ottawa
References:
1. Kates et al. Ann Surg Onco 2012
2. Bazzi et al. J Urol 2012
3. Farber et al. Urol Onc 2019
4. Lavalle L et al. EBU 2018
5. Blom JH et al. Eur Urol 2009
6. Bhindi B. et al. BJU Int. 2018
7. Gershman B et al. Eur Urol 2017
Further Related Content:
Lymph Node Dissection at the Time of Nephrectomy - PRO


