Pts who did not undergo nephrectomy had shorter overall survival (OS) than patients who had nephrectomy.1 Dr. Tannir presented a study demonstrating the outcomes for cabozanitinib (CABO), a cMET inhibitor vs. Everloimus (EVE), an mTOR inhibitor, in patients with advanced RCC with or without prior nephrectomy in the phase 3 METEOR trial (NCT01865747).
658 pts with clear cell RCC and ≥1 prior VEGFR Tyrosine Kinase Inhibitors (TKI) were randomized 1:1 to receive CABO at 60 mg qd or EV at 10 mg qd. Patient stratification was performed by MSKCC risk group and the number of prior VEGFR TKIs. The study endpoints included progression-free survival (PFS), overall survival (OS), and objective response rate (ORR).
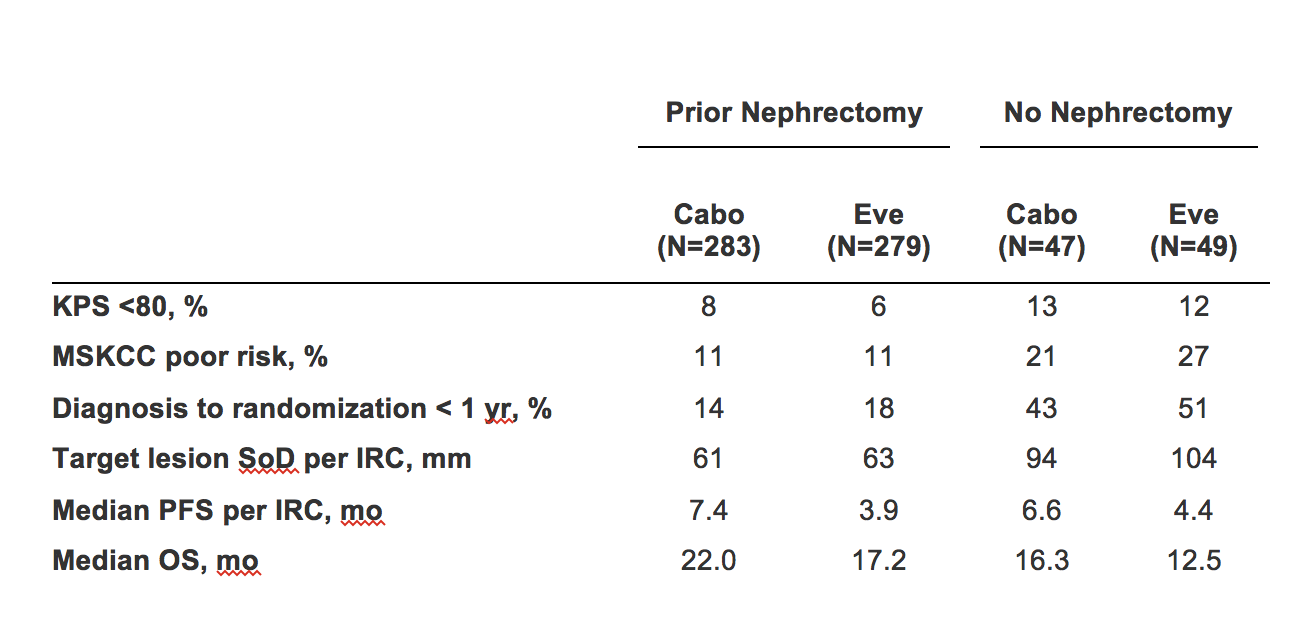
A total of 85% of enrolled pts (562) had prior nephrectomy of which 7% were partial. Baseline characteristics, including Kranofsky performance status (KPS), MSKCC risk group, time from diagnosis to randomization, and median sum of diameters (SoD) for tumor target lesions, were less favorable for the no nephrectomy subgroup, as demonstrated in the table below. Improved PFS and OS with CABO vs EVE were observed regardless of nephrectomy status: for the nephrectomy subgroup, the hazard ratio (HR) was 0.51 (95% CI 0.41-0.64) for PFS and 0.66 (95% CI 0.52-0.84) for OS; and for the no nephrectomy subgroup, the HR was 0.51 (95% CI 0.30-0.86) for PFS and 0.75 (95% CI 0.44-1.27) for OS. Median OS was longer in the nephrectomy subgroup for both treatment arms. ORR per independent radiology committee (IRC) for CABO vs EVE was 17% vs 4% for the nephrectomy patients and 21% vs 2% for the no nephrectomy patients. Grade 3 or 4 adverse events for both subgroups were generally consistent with the safety profiles of CABO and EVE in the overall population. The main limitations of this study include the post-hoc nature of the analyses and the small size of the subgroup without prior nephrectomy.
In summary, CABO improved PFS, ORR, and OS compared with EVE in pts with advanced RCC irrespective of nephrectomy status. All baseline characteristics were less favourable for the patients without nephrectomy. For both treatment arms nephrectomy was associated with longer median OS.
Presented By: Nizar M. Tannir, The University of Texas MD Anderson Cancer Center, Houston, TX
Written By: Hanan Goldberg, MD, Urologic Oncology Fellow (SUO), University of Toronto, Princess Margaret Cancer Centre
Twitter: @GoldbergHanan
REFERENCES:
1. Hanna N, Sun M, Meyer CP, et al. Survival Analyses of Patients With Metastatic Renal Cancer Treated With Targeted Therapy With or Without Cytoreductive Nephrectomy: A National Cancer Data Base Study. Journal of clinical oncology : official journal of the American Society of Clinical Oncology 2016; 34(27): 3267-75.
at the 2017 ASCO Annual Meeting - June 2 - 6, 2017 - Chicago, Illinois, USA

