Conservative options for the management of nocturia include lifestyle and behavioral modifications such as decrease in fluid intake, bladder training techniques, and oedema management. Compression stockings and leg elevation are recommended to address an issue of extra fluid in the lower limbs, but data on effectiveness are scarce.
The goal of the presented study was to evaluate if leg elevation prior to bedtime can decrease nocturic episodes and estimate the effect of intervention on the first uninterrupted sleep period, nighttime urine volume, and overall quality of life linked to the condition.
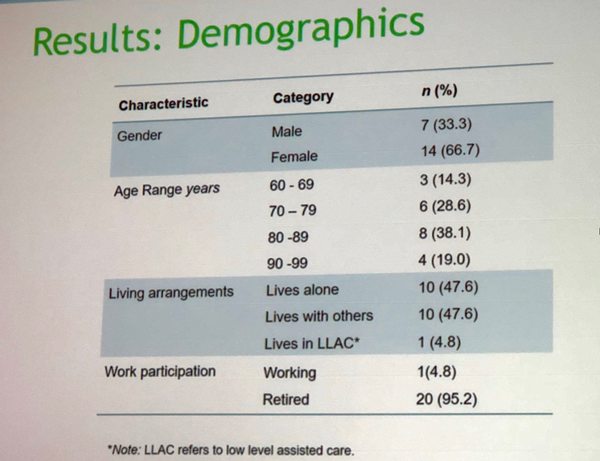
Total number of 21 subjects was enrolled to the prospective, single group, pre-and post group research. Study sample included males and females 60 year of age or older, with diagnosis of cardiovascular disease, peripheral oedema, and nocturia. Sample baseline data is reflected in Table 1.
Subjects were recruited between July 2017 and November 2017 from the outpatient Continence Service clinic and followed for 2 weeks. Researchers utilized 24-hour voiding diary to assess nocturic episodes and voided volumes and actigraphy to document sleep patterns. Subjects were prescribed leg elevation in a supine position before bedtime for 2 weeks. In addition, they had to complete Nocturia Quality of Life Questionnaires and measure ankle circumference every morning and evening.
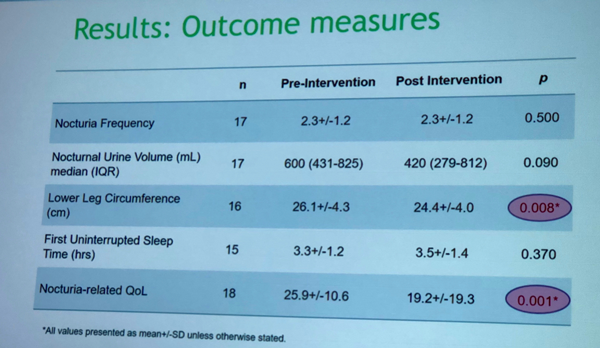
Data show that peripheral edema has significantly decreased in study participants. Subjects reported increase in nocturia-specific quality of life and improvement in nighttime voided volume. However, no statistically significant changes were found in a number of nocturic voids and first uninterrupted sleep period (Figure 2).
Study outcomes can possibly be affected by the small sample size, lack of adherence to the protocol by the participants, and short prescription term. Data suggest that active leg elevation can potentially improve oedema and overall quality of life, but further research in essential in evaluating program’s sustainability and subject’s adherence to the protocol.
Presented by Claire F Ervin, RN, Royal Melbourne Hospital, Australia
Coauthors: Murphy M, Rose G E, Ong T, Whishaw D M, Bower W F
Written by: Hanna Stambakio, BS, Clinical Research Coordinator, Division of Urology, University of Pennsylvania, Twitter: @PennUrology at the 2018 ICS International Continence Society Meeting - August 28 - 31, 2018 – Philadelphia, PA USA


