According to Dr. Novosad, catheter-associated urinary tract infections (CAUTI) are the most common disease linked to healthcare. These conditions increase morbidity and mortality, prolong hospitalization, and elevate medical costs.
National Healthcare Safety Network (NHSN) uses the following surveillance definition of CAUTI (Figure 1):
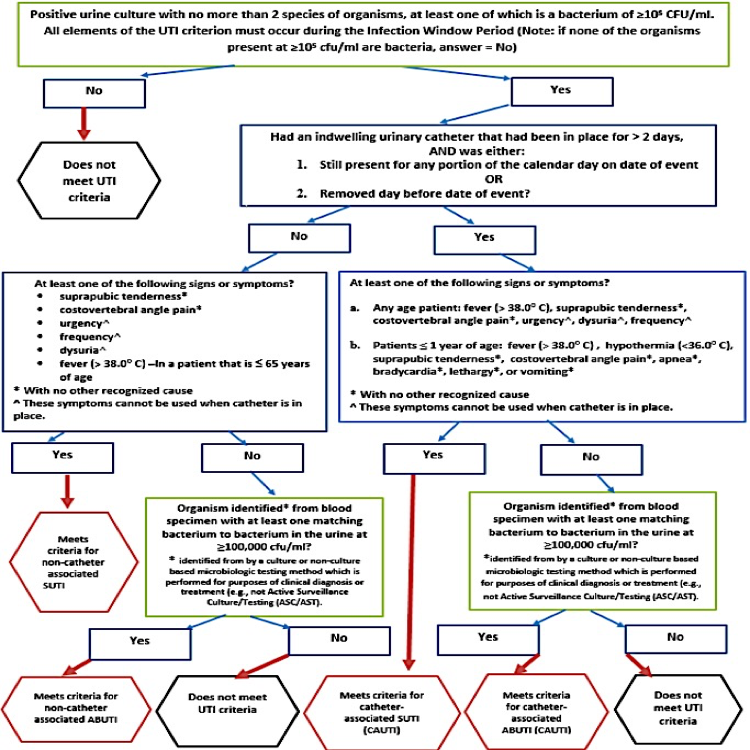
Figure 1
In 2015, UTI definitions were changed to exclude cultures with colony counts less than 100,000 CFU/ml and yeast infections. Figure 2 reflects changes in standardized infection ratio (SIR) of CAUTI in 2009 – 2016. SIR is defined as an actual number of CAUTI/predicted number of CAUTI.
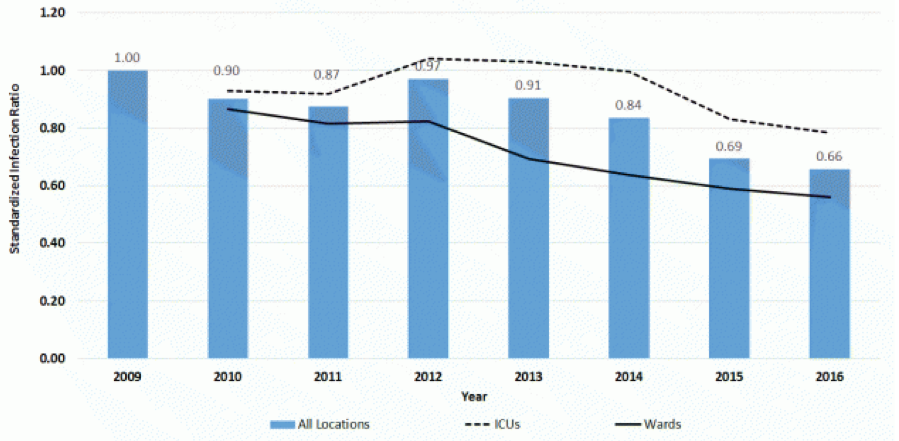
Figure 2
Although there is a decrease in a number of healthcare-associated urinary tract infections, further actions are needed to prevent CAUTI. Dr. Novosad stated that risk of infection increase by 3-7% each day a catheter is in place. Primary risk factors of UTI and bacteriuria include prolonged catheterization, disconnection of the drainage system, lower professional training of inserter, female gender, older age, and patient’s compromised immunity.
Current CAUTI guidelines stress an importance of insertion of urinary catheter only for appropriate indication and only for the appropriate amount of time. Since these practices vary among practices and providers, it would be beneficial to create and implement site-specific policies for utilizing indwelling catheters. For example, quality control checklists can be created to ensure appropriate practices during catheter insertion and maintenance.
It is also crucial to provide guidance in diagnosing urinary tract infections. Dr. Novosad pointed out that 20 to 83% of patients with asymptomatic bacteriuria are treated with antibiotics, which leads to antimicrobial overuse, the emergence of resistant bacteria strains, and adverse health events. New Antimicrobial Stewardship Standard recommends testing for UTI only when clinical symptoms are present.
Urine culture protocol in the intensive care units (ICU) suggests conducting urinalysis on the specimen first. It is recommended to perform urine culture only if pyuria is present in the specimen after urinalysis. These guidelines are not mandated and left to the discretion of each ICU in the US. However, such intervention lead to the decrease in CAUTI rate across practices which decided to participate (Figure 3)
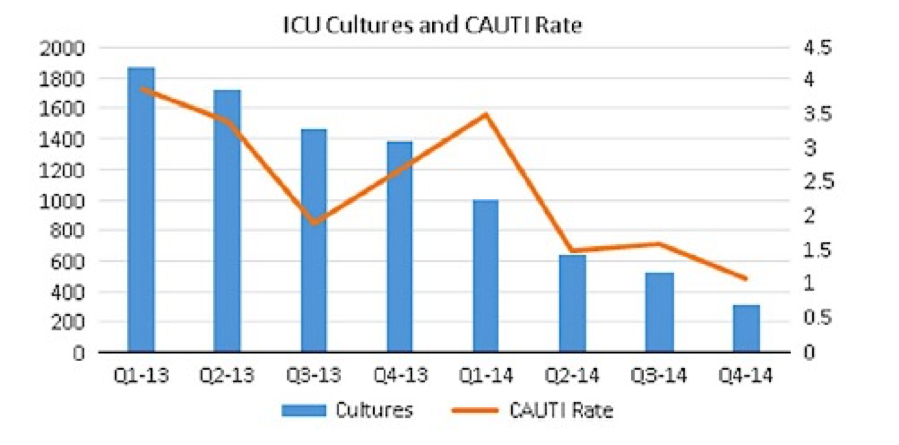
Figure 3
Finally, Dr. Novosad reviewed targeted assessment for prevention (TAP) of healthcare-associated infections (HAI). TAP is a CDC framework for quality improvement that utilizes prevention strategies. TAP is available for the number of HAI including urinary tract infections linked to the catheter use.
TAP reports of the facilities with high infection rates are generated by the NHSN. These practices are offered to participate in the prevention interventions by assessing potential gaps in infection control and calculating scores within the facility. Then practice data are presented using TAP feedback report along with the implementation tools and links to resources.
Presented by: Shannon Novosad, MD, MPH, Medical Officer, Hospital Infection Prevention Team, Division of Healthcare Quality Promotion, National Center for Emerging and Zoonotic Infectious Diseases, Centers for Disease Control and Prevention
Written by: Hanna Stambakio, BS, Clinical Research Coordinator, Division of Urology, University of Pennsylvania, @PennUrology at the 2018 ICS International Continence Society Meeting - August 28 - 31, 2018 – Philadelphia, PA USA


