Contents
Introduction
I am very pleased to present you this study in regard the Diagnostic and prognostic value of FDG-PET in recurrent germinal tumor carcinoma.
Testicular cancer represent the 1-5% of all cancer. 25% of patients present with advanced stage disease. After chemotherapy, one of the problem is that the detection of residual masses can occur in 60% of them. Relapse occur in 10-15% of these patients. So, there is a problem in the differential diagnosis between residual disease versus fibrosis.
Long term survival rate is generally favorable but prognosis is variable according to different factors. So, an accurate diagnostic tool capable to predict survival is mandatory to ensure the best strategy treatment.
PET Prognostic Role
Several study have discussed the role of PET and it's potential value at staging and re-staging also with divergent results. At present, FDG-PET is not completely validated in the clinical scenario for testicular cancer, and the prognostic role of PET remains still undefined.
I will show you two article with divergent results because Ambrosini et al. in patients with testicular cancer show low sensitivity for Non-seminoma cancer. Oppositely, Sharma et al. in the same type of patient show the sensitivity of 96%.
FDG-PET Prognostic Evaluation
About the prognostic evaluation of FDG-PET, I did not find a lot of paper about the prognostic evaluation by using PET. This is one example of study in regard the negative Postchemotherapy Positron Emission Tomography evaluation, and the author find that FDG-PET have negative predictive value of 81.7%.
Study Objectives & Design
The aim of this study was to evaluate the performance of FDG-PET during the re-staging process of testicular cancer, to evaluate the effect on treatment decision, and to evaluate the prognostic value of FDG-PET in patient with suspected recurrent germinal tumor cancer.
The type of the studies retrospective involving three Italian departments. 114 patients with germinal tumor carcinoma underwent re-staging FDG-PET for suspicious for recurrent disease. The inclusion criteria was certain diagnosis of testicular cancer after surgery, FDG-PET/CT performed after first-line surgery and/or chemotherapy, and FDG-PET findings were verified by histology and/or other imaging, clinical and instrumental follow-up data was available for at least 24 months from surgery.
PET analysis consider for the accuracy the histology in 17 patients. Contrast-enhanced CT, it was used in 89 patients. MRI was used as a gold standard for accuracy in 15 patients, and clinical follow-up data was available for all patients. In each center, qualitative and semiquantitative evaluation was preformed also by using a semiquantitative like MTV, SUVmax, and SUVmean.
In evaluation of the survival and the risk of progression, we use Kaplan-Meier curves in order to estimate the progression free survival and overall survival. We also use a Cox Regression in order to establish the impact on the risk of progression of better results.
Study Results
Going to the results, 62 patients were negative for PET/CT. 52 patients were positive, and in 46 patients was confirmed a recurrent disease with the gold standard. In 26 patients, the clinical management was changed after PET, and in particular, in 12 patients there was a changing of therapy from surgery or other therapy to second-line chemotherapy. In 6 patients, the therapy changed from second-line chemotherapy to surgery or other therapy. And in 8 patients, there was a change in therapy from surgery or other therapy to watch and wait strategy.
The sensitivity was high, with 88.7%. Specificity was 91.8%. Positive predictive value, negative predictive value and accuracy were all around 90%. No significant difference in accuracy among Seminoma and Non-Seminoma patients was found.
Going to the Kaplan-Meier curves, we can see on the left that after two years of follow up, progression for survival was a significantly longer in patients with a negative scan versus a positive scan. Moreover, on the right we can see that the negative study was associated with a significantly longer overall survival, than a positive one.
By combining PET with TNM staging, progression for survival and overall survival were significantly longer in patients with a negative PET for all stage of disease, in particular for stage three.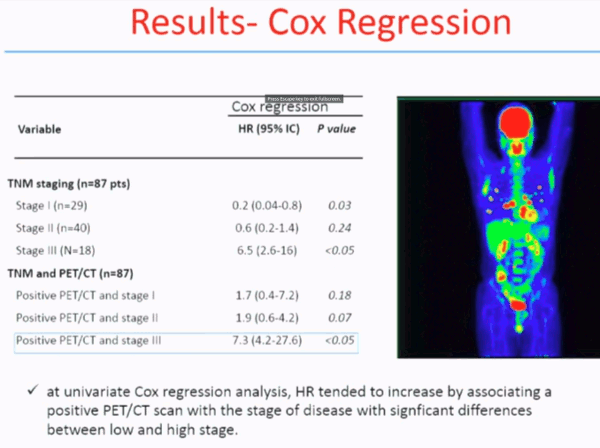
Cox Regression revealed that there is a very high impact of PET/CT in predicting the risk of progression. A positive PET scan was associated with an increased risk of progression with hazard ratio of 24. We found, also, among PET positive patients that the value of SUVmax more than 8 may increase the risk of progression.
Similar results were found if we combine the PET results with the stage. At univariate Cox Regression analysis, hazard ratio tended to increase by associating a PET positive scan with stage of disease, with significant difference between lower and higher stage.
Conclusion & Summary
In conclusion, we can say that FDG-PET/CT has a high diagnostic performance in patients with suspicions of recurrent testicular cancer supporting the use of this method in the clinical scenario. PET may provide crucial information to select the best strategy treatment when recurrent occur after first-line therapy. Although prospective clinical trials are warranted, our results show that FDG-PET has an important prognostic value in the re-staging process of testicular cancer predicting risk of progression and survival rate.


