The NYU group retrospectively reviewed the charts of all PD patients who underwent video urodynamics (VUD) for storage symptoms between 2010 and 2017 at their institution. Only patients with PD who complained of OAB symptoms and underwent VUD were included after a movement disorder specialist had examined them.
Forty-two patients were included in the analysis, with a mean age of 74.5 years. 69% of the subjects were men, and 31% were women, with a mean BMI of 25.9 and a disease duration of an average of 6.6 years. Of these, 70.5% had been on anticholinergic medications, 56.8% had a history of mirabegron use, 31.8% had a history of alpha-adrenergic blockers, 20.5% had a history of surgery for BPH, 4.5% had a history of intradetrusor botulinum toxin, and 7.1% had no prior treatment.
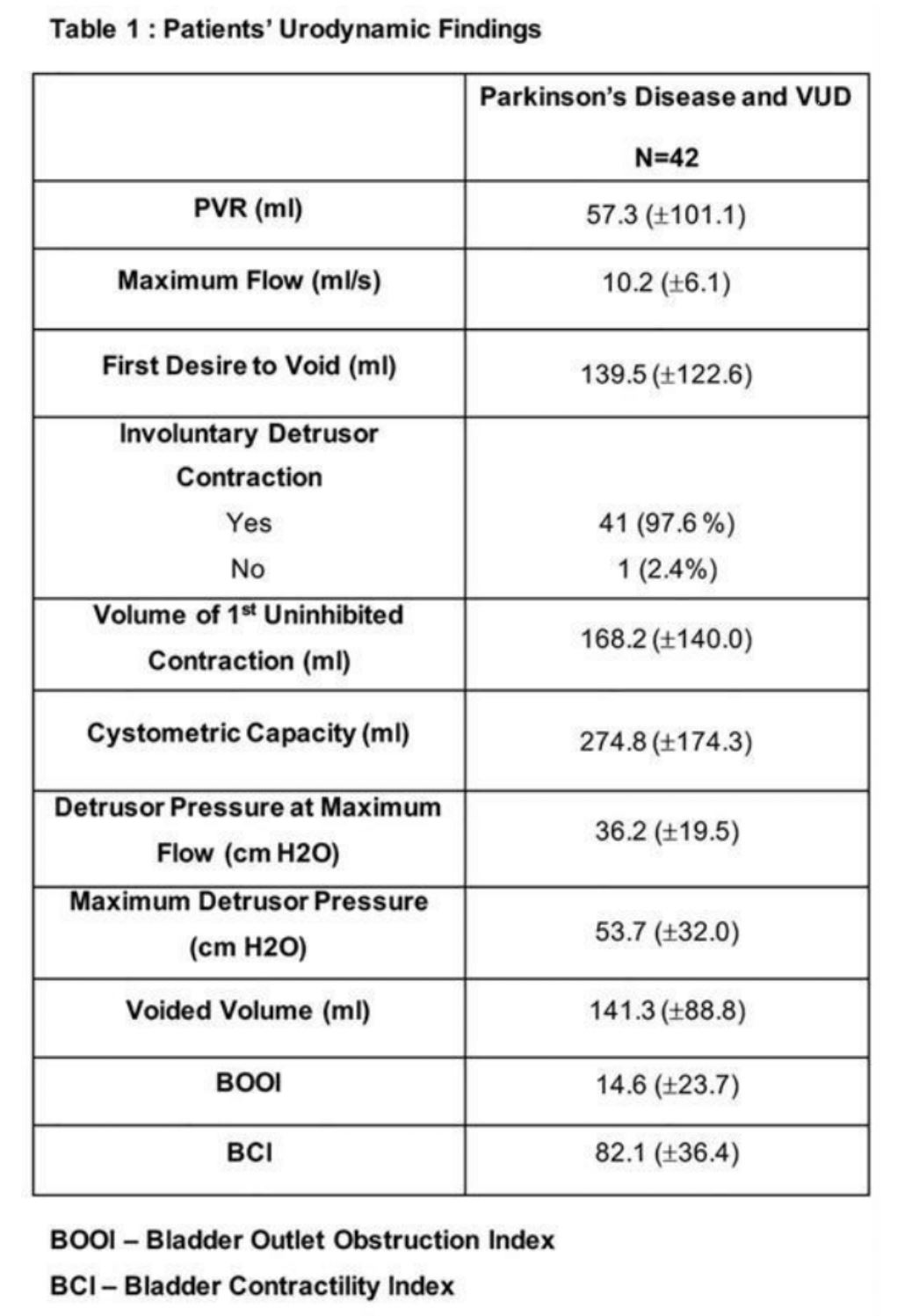
On VUD, the mean post-void residual was 57.3 ±101.1 ml, with a cystometric capacity of 274.8 ± 174.3 ml. 41 of the 42 patients (97.6%) were noted to have an involuntary detrusor contraction (IDC), and the authors noted the one patient who did not demonstrate an IDC was diagnosed just 2 months prior to VUD. The first desire to void occurred on average at 139.5 ± 122.6 ml. The mean volume of the first uninhibited contraction was 168.2 ml. On pressure flow analysis, the patients had an average maximum flow of 10.2 ml/s (9.9 ml/s for males, and 8.4 ml/s for females), with an average detrusor pressure at maximum flow of 36.2 cm H2O. The maximum detrusor pressure was 53.7 cm H2O (41.3 cm H20 for males, 22.6 cm H20 for females). The average voided volume was 141.3 ml.
Of their cohort, 18/42 (42.9%) demonstrated detrusor underactivity on UDS, and 20/42 (47.8%) were found to have normal bladder contractility. When comparing these two group, there was no difference in post-void residuals, first sensation, first IDC, gender, and age, but there was a higher rate of mean age of PD diagnosis (detrusor underactivity group with 69.1 years vs normal contractility group with 63.6 years, p=0.02) in those with detrusor underactivity.
The authors concluded that most PD patients with OAB symptoms exhibit DO on VUD, but that the decision to perform urodynamics in these patients should be prompted by other objectives than diagnosing DO due to the high probability of OAB based on clinical symptoms.
Presented by: Gregory Vurture, MD, New York University School of Medicine, New York, New York
Written by: Judy Choi, MD, Assistant Professor, Department of Urology, University of California, Irvine @judymchoi at the Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction Winter Meeting, SUFU 2019, February 26 - March 2, 2019, Miami, Florida


