He first started by setting the stage for the study. Upper tract urothelial carcinoma (UTUC) is rare when compared to bladder cancer. However, unlike bladder cancer, 60% of UTUC patients present with invasive disease. At this time, the standard of care for these patients is radical nephroureterectomy (RNU) and observation. While management of advanced UTUC has often been extrapolated from the bladder cancer literature, due to the rarity of the disease, there is little evidence for UTUC itself. Yet, as some UTUC patients are included in the metastatic bladder cancer studies, retrospective analyses suggest that patients with metastatic UTUC are similar to those patients with metastatic bladder cancer. Therefore, the rationale for the POUT trial was laid by the strong level 1 evidence for perioperative chemotherapy for MIBC. However, they chose to pursue adjuvant therapy, and pre-operative grading and clinical staging for UTUC is notoriously difficult – therefore, it would be easier to justify systemic therapy for patients with known pathology from an RNU.
Given that the role of post nephroureterectomy treatment for upper tract urothelial carcinoma (UTUC) is unclear, the UK led POUT trial (CRUK/11/027; NCT01993979) addressed whether adjuvant chemotherapy improves disease-free survival (DFS) for patients with histologically confirmed pT2-T4 N0-3 M0 UTUC.
For this trial, patients (maximum n=345) that had a WHO performance status 0-1, and were ≤90 days post nephroureterectomy were randomized (1:1) to 4 cycles of gemcitabine-cisplatin (gemcitabine-carboplatin if GFR 30-49ml/min) or surveillance with chemotherapy given on recurrence, if required. The primary endpoint was DFS, and patients had cross-sectional imaging and cystoscopy every 6 months for the first 2 years, then annually to 5 years. Toxicity was assessed by CTCAE v4. The trial was powered to detect a hazard ratio (HR) of 0.65 (i.e. improvement in 3-year DFS from 40% to 55%; 2-sided alpha=5%, 80% power) with Peto-Haybittle (p<0.001) early stopping rules for efficacy and inefficacy. Secondary endpoints included metastasis-free survival, overall survival, toxicity (CTCAE v4) and patient-reported quality of life, assessed by EORTC QLQ-C30 and EQ5D.
There were 261 patients included in the trial between May 31, 2015, and November 2017, including 129 patients randomized to surveillance and 131 to chemotherapy at 57 UK centers. In November 2017, the independent trial oversight committees recommended POUT close to recruitment as data collected to date met the early stopping rule for efficacy. At the time of interim analysis, the median follow-up was 17.6 months (IQR 7.5-33.6).
Baseline characteristics are summarized below:
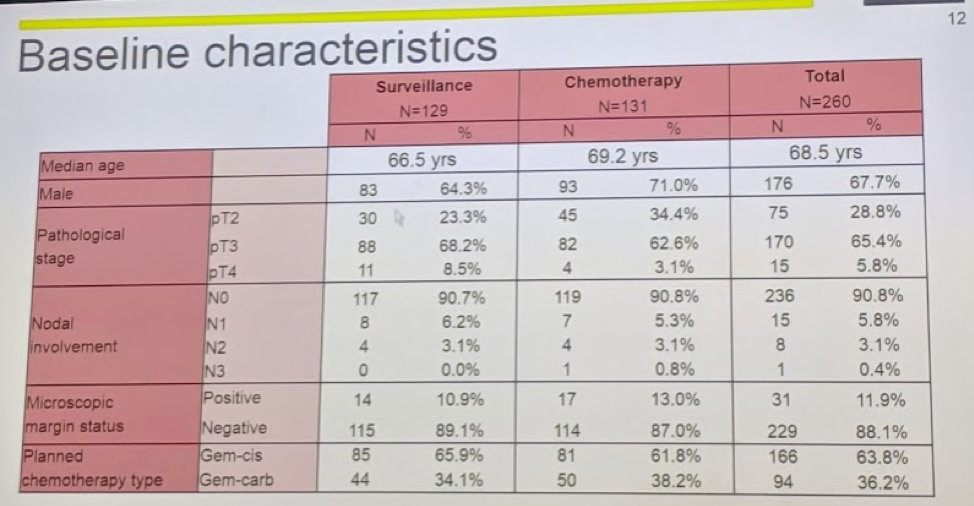
He did specifically point out that most patients were pT3 (~60-70% in each arm), were pN0 (90% in both arms) and margin negatively. Approximately 2/3 received Gem-Cis, while 1/3 received carbo.
Treatment compliance was pretty good – 72% of patients received all 4 cycles.
Grade ≥3 toxicities were reported in 62.1% of chemotherapy patients and 24.8% surveillance patients. During the treatment period, the most common grade ≥3 [≥4] toxicities in chemotherapy patients were hematologic (as expected) and some nausea/vomiting (1.4-2.9%).
In terms of quality of life, as expected, the chemotherapy patients took a hit within the first 12 months – primarily driven by nausea/vomiting. However, by 12 months, there were no differences between the 2 arms.
After a median follow-up of 17.6 months, a significant difference in DFS (HR 0.49, CI 0.31-0.76, p=0.001) favoring the chemotherapy arm was observed. Following adjustment for nodal involvement, microscopic margin status and planned chemotherapy type, the difference was even more pronounced with an HR 0.47, CI 0.30-0.74, p=0.001). At 2-years, this translated to a difference of 17% absolute difference in recurrence-free survival.
When analyzing the secondary end-points, adjuvant chemotherapy was also associated with an improved RFS (HR 0.49, CI 0.30-0.78, p=0.02). Unfortunately, the overall survival is not mature enough, and the although the results demonstrate a separation in the overall survival curves, no significant difference can be discerned at this time point.
Dr. Jones concluded that adjuvant chemotherapy is tolerable, and improved metastasis-free survival in UTUC. Recruitment to the POUT trial was terminated early because of efficacy favoring the chemotherapy arm, however, follow-up for overall survival continues. POUT is the largest randomized trial in UTUC and its results support the use of adjuvant chemotherapy as a new standard of care.
He did note that POUT2 is a new study being developed in which patients are randomized to chemotherapy vs. chemotherapy/immunotherapy – and this does allow for some neoadjuvant treatment.
Presented by: Robert Jones, MD, Professor of Clinical Cancer Research, The University of Glasgow, United Kingdom
Written by: Thenappan Chandrasekar, MD. Clinical Instructor, Thomas Jefferson University, Twitter: @tchandra_uromd, @TjuUrology, at the 16th Meeting of the European Section of Oncological Urology, #ESOU19, January 18-20, 2019, Prague, Czech Republic
Related Content:
Read: ASCO GU 2018: Results of POUT: A Phase III Randomized Trial of Perioperative Chemotherapy versus Surveillance in Upper Tract Urothelial Carcinoma (UTUC)

