The authors of this study attempted to describe the upgrading, upstaging, positive surgical margins rate, and location of recurrences at sRARP after failed HIFU treatment. Additionally, the authors attempted to assess the sensitivity of MRI and biopsy against sRARP in the post HIFU setting.
A total of 34 men who underwent sRARP after failed HIFU therapy were analyzed in this study.
Before HIFU, the median age was 64 years with a median PSA of 7.8 ng/dl. Median time to post-HIFU recurrence was 16 months. The MRI-biopsy demonstrated that 56% had in-field recurrence, while 21% had an out-of-field recurrence, and 23% had both types of recurrences.
When analyzing the pathology results of the sRARP, in 94% of cases, the disease was multifocal. The positive surgical margins rate was 31% in the T2 patients, and 43% in the T3 patients. The MRI sensitivity for post-HIFU in-filed-recurrence, out-of-field -recurrence and pathological stage T3 were 82%, 65%, and 10%, respectively. Table 1 demonstrates the comparison of pathological features in pre-HIFU, pre-sRARP, and at sRARP. Figure 1 demonstrates the adverse reclassification rates at sRARP vs. post-HIFU presurgical biopsy/MRI.
The authors concluded that in patients who have failed HIFU, the sensitivity of MRI was limited, and when they underwent sRARP, upgrading, upstaging and positive surgical margins were quite common.
The limitations of this study include its retrospective nature, and its relatively small sample size, with an obvious inherent selection bias. Studies with larger sample sizes are needed before any recommendation can be made.
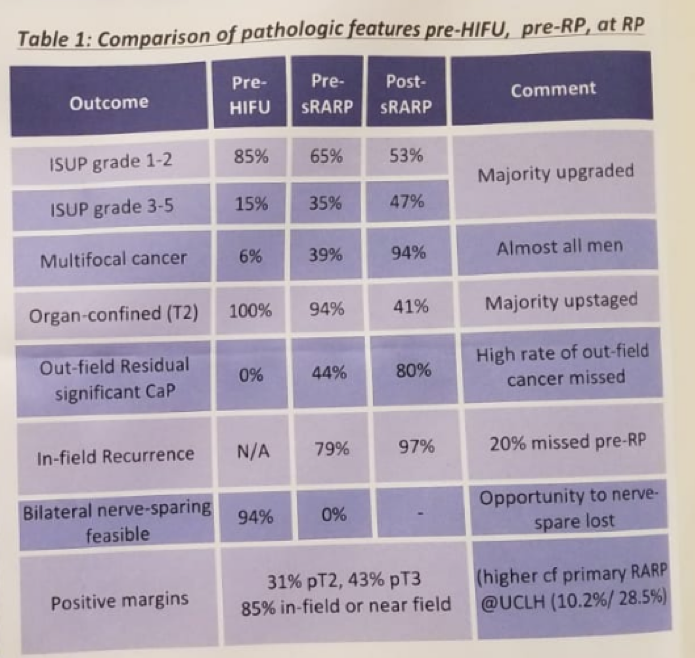
Table 1:
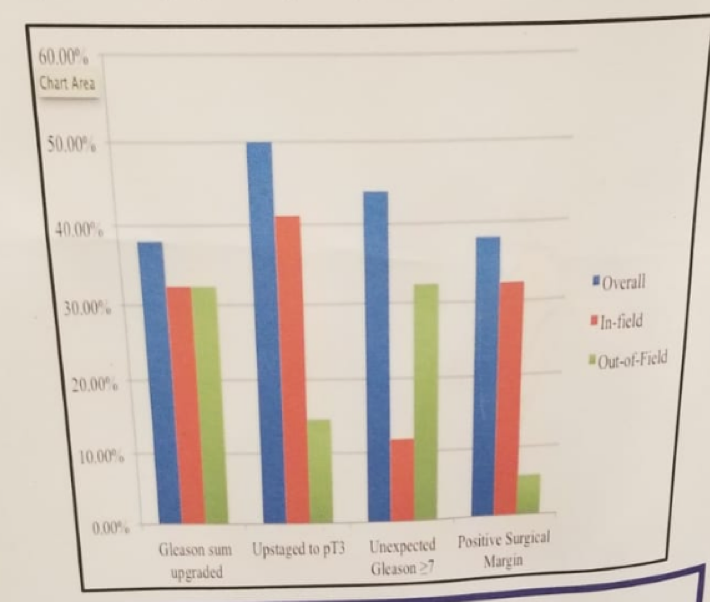
Figure 1 – adverse reclassification rates at sRARP vs post-HIFU presurgical biopsy/MRI:
Presented by: J Thompson, University College London Hospital, London, UK
Written by: Hanan Goldberg, MD, Urologic Oncology Fellow (SUO), University of Toronto, Princess Margaret Cancer Centre, Twitter:@GoldbergHanan at the EAU Robotic Urology Section (ERUS) Meeting - September 5 - 7, 2018 - Marseille, France


