Radical Nephroureterectomy (RNU) is an effective operation for a rate, but potentially very aggressive, upper tract urothelial cancer. Prior studies have put the 10-year CSS at ~67% (Dahl et al. NEJM 2004). However, there is still room for improvement.
1. Is minimally invasive approach appropriate?
a. Laparoscopic approach – he first reviewed the literature of laparoscopic vs open experiences.
- Hanna et al. (EU 2012) – demonstrated that the laparoscopic approach was associated with lower EBL, shorter hospital stays, lower blood transfusions, but slightly longer operative times
- In terms of oncologic outcomes, multiple observational studies have had conflicting results regarding survival outcomes – work by Simone et al (EU 2009) and others suggested worse outcomes (MFS and CSS) for laparoscopic surgery specifically for patients with pT3-4 disease
- Based on this data, current EU recommendations (Roupret et al. EU 2018) suggest both are equivalent for pT1-2N0 cancers
- Similar to laparoscopic surgery, it appears to have benefits with regards to LOS, EBL and transfusion rates
- There does not appear to be any difference between robotic and open surgery
- No specific recommendations were made about this approach on the guidelines
Due to the high rate of ureteral stump recurrence (between 30-75%), bladder cuff excision (BCE) is recommended for all RNU. Lughezzeni et al. (EU) demonstrated a cancer-specific survival benefit to RNU with BCE vs. RNU alone. Hence, this is a Class A recommendation in the guidelines.
But, there are 3 main techniques for removal:
1. Extravesical (open, laparoscopic, robotic)
2. Transvesical (open)
3. Transurethral resection to free the UO through the muscle/fat – and then either “pluck” technique or formal dissection
Xylinas et al. (EU 2010) did a review of the 3 techniques. There was no difference in RFS, CSS, and OS with all three techniques, but an endoscopic approach was associated with a higher intravesical recurrence (IVR) rate with endoscopic management – especially in patients with no prior bladder cancer.
Seisen et al. (EU) in their systematic review found that when comparing extravesical to the transvesical, an extravesical approach favored higher IVR. No similar effect was found when comparing endoscopic to transvesical.
Based on this, his main take home was to be careful with the extravesical approach – specifically the habit of ligating across the distal ureteral stump without making sure to have excised it entirely. The transvesical approach has the strongest evidence.
3. Lymph node dissection (LND)
LND for UTUC is increasing in utilization. Most results support the staging benefit of LND that allows for risk stratification (N0/N+), which has potential implications for subsequent therapy.
From recent data, the best accuracy of staging comes from getting 8+ nodes on the LND – with an associated sensitivity of 75%. Ultimately, it is the number of positive lymph nodes (absolute number and other measures, such as lymph node density) that have prognostic value.
The therapeutic benefit of LND is not yet as clear. Yang et al. (Expert Review Anticancer) completed a systematic review and found that LND did not have therapeutic benefit for all RNU but in a subset of patients with the muscle-invasive disease, it was associated with cancer-specific survival benefit (HR 2.19). Results are seen below:

This same group has done significant work in this field, and also found that:
1. A complete LND is significantly associated with improved CSS, particularly in pT3-4 patients
2. Complete regional LND is more important than the number of nodes obtained
3. The therapeutic benefit appears to be higher for renal tumors than ureteral tumors
For this reason, template-based complete LND in patients with high-risk UTUC is recommended.
Two different anatomic templates are listed below (first is the top panel, the second is bottom panel):
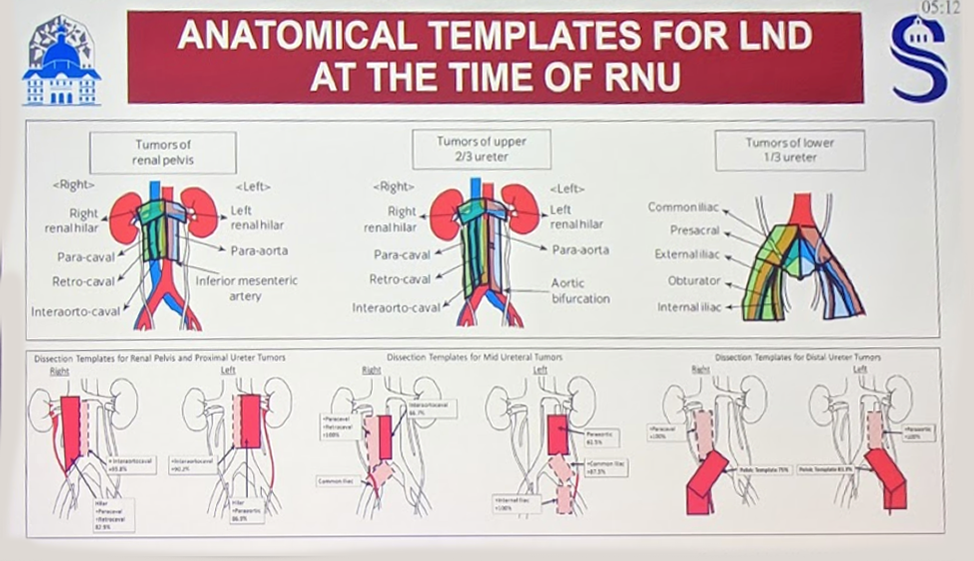
These are stratified by location of the primary tumor – renal pelvis, upper 2/3 of the ureter, distal 1/3 of the ureter.
Presented by: Thomas Seisen, MD, Department of Urology, Pierre and Marie Curie University, Paris, France
Written by: Thenappan Chandrasekar, MD (Clinical Instructor, Thomas Jefferson University) (twitter: @tchandra_uromd, @TjuUrology) at the 34th European Association of Urology (EAU 2019) #EAU19, conference in Barcelona, Spain, March 15-19, 2019.

