(UroToday.com) The game changing session of the European Association of Urology (EAU)’s 2021 annual meeting included a presentation by Dr. Michael Hofman from the Peter MacCallum Cancer Centre discussing the phase 2 trial of 177Lu-PSMA-617, TheraP, as well as important contrasts/differences between TheraP and VISION. TheraP was an ANZUP/PCFA sponsored trial that began in 2016 and represents a world-first study, being a phase III randomized controlled trial of a direct targeted radioligand.
TheraP enrolled patients with mCRPC who had previously received docetaxel and were eligible to receive cabazitaxel. Patients were required to have progressive disease with a rising PSA with absolute PSA of 20 ng/mL or higher. All patients underwent both Ga-68-PSMA-PET/CT and F-18-FDG-PET/CT prior to randomization. To be eligible for inclusion, patients must have had a high avidity lesion on PSMA PET/CT (SUV max >20 at any site) with measurable disease with SUV max of 10 or greater. Further, there could be no sites of disease which were FDG positive but PSMA negative. Among 200 men at 11 sites in Australia who were eligible, randomization was performed in a 1:1 fashion to 177Lu-PSMA-617 or cabazitaxel. Randomization was stratified according to disease burden, prior use of enzalutamide or abiraterone, and study site.
The primary study outcome was PSA response and these data were initially reported at ASCO 2020. PSA response was operationalized looking at a response of at least 50% from baseline. Compared to those receiving cabazitaxel (37%, 95% CI 27 to 46%), responses were significant higher among those who received Lu-PSMA (66%, 95% CI 56 to 75%) with an absolute difference of 29% (95% CI 16 to 42%, p<0.0001):
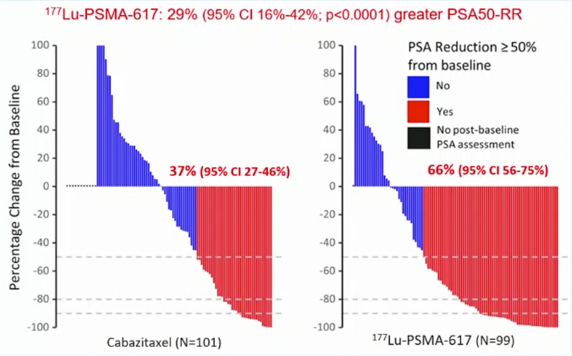
More recent data were presented at ASCO-GU 2021 examining secondary endpoints including PSA/radiologic PFS (PCWG3), pain response (≥2 point reduction on McGill-Melzack Present Pain Intensity scale, objective response rate (RECIST 1.1), adverse events (CTCAE), and PROs (EORTC QLQ-C30). Over a median follow-up of 18.4 months, PFS was significantly longer in those assigned 177Lu-PSMA-617 rather than cabazitaxel (rates at 1 year 19% [95% CI 12-27%] versus 3% [1-9%], HR 0.63, 95%CI 0.46-0.86; p = 0.0028) based on 173 events. 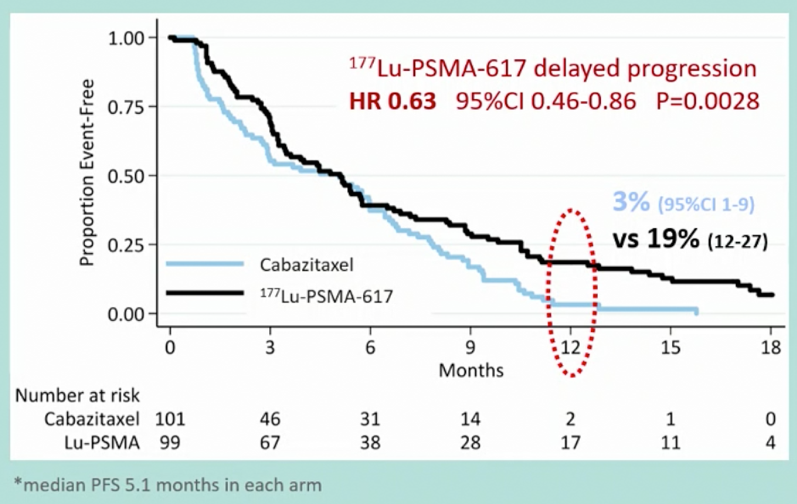
A similar benefit was seen whether PFS was examined radiographically (rPFS, HR 0.64, 95% CI 0.46-0.88; p = 0.007; 160 events) or based on PSA (PSA-PFS, HR 0.60 95% CI 0.44-0.83; p = 0.002; 172 events). Among men with measurable disease (n=78), objective response rates were significantly greater in the 177Lu-PSMA-617arm (49% versus 24%, RR 2.1, 95% CI 1.1-4.1; p = 0.019):
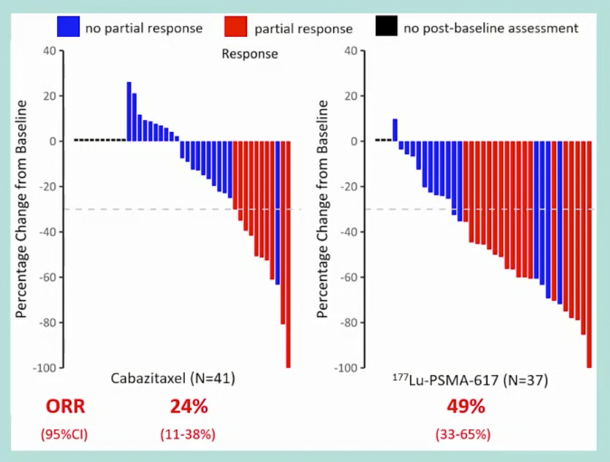
With regards to Grade 3-4 adverse events, the 177Lu-PSMA-617 arm had more thrombocytopenia (11% vs 0%), whereas the cabazitaxel arm had more neutropenia +/- fever (13% vs 4%):

Among those with pain at baseline (n=90), pain responses occurred in 60% in the 177Lu-PSMA-617 arm versus 43% for cabazitaxel (RR 1.42, 95% CI 0.84-4.48; p = 0.10). Overall, patient-reported global health status was similar between arms (177Lu-PSMA-617: 64 [95% CI 61-67] versus cabazitaxel: 60 [57-64]), though significantly better function was noted for patients receiving 177Lu-PSMA-617with respect to fatigue, social functioning, insomnia, and diarrhea domains. No PRO domains were superior for cabazitaxel. The trial also further assessed deterioration free survival, defined as the time to a 10 point or greater decline in EORTC QLQ-C30 global health related quality of life, which also favored the 177Lu-PSMA-617 treated group: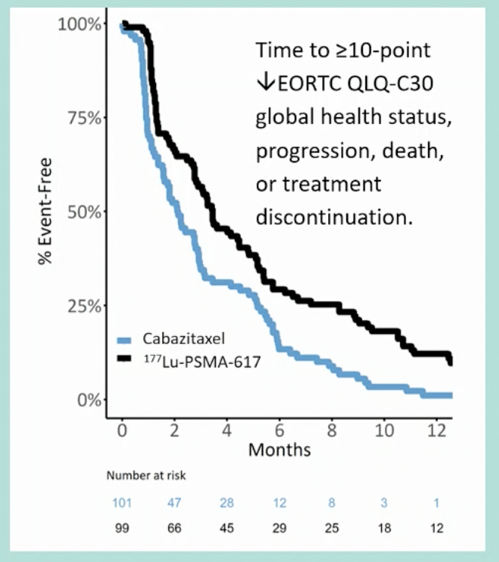
Dr. Hofman then contrasted the TheraP [1] and VISION [2] trials. The following table summarizes these findings, with notable differences in the percentage of patients excluded from the trial (28% for TheraP versus 12% for VISION), and PSA >= 50% (66% for TheraP versus 46% for VISION):
Dr. Hofman then discussed several patient’s noting their eligibility for TheraP versus VISION:
- Patient #1 – “low” PSMA uptake in the retroperitoneal nodes, but avid on FDG-PET. This patient would have been ineligible for TheraP given the FDG-PET activity (and corresponding negative PSMA PET activity), but eligible for VISION.
- Patient #2 – heterogeneous uptake in the bone (negative on PSMA-PET and avid on FDG-PET). This patient also would have been ineligible for TheraP, but eligible for VISION
Dr. Hofman concluded his presentation with the following take home messages, as well as noting that 177Lu-PSMA-617 is a new class of effective therapy:
- 177Lu-PSMA-617 improves patient outcomes in men with mCRPC following docetaxel and androgen receptor directed therapy
- 177Lu-PSMA-617 is more active than cabazitaxel in PSMA-avid disease with fewer Grade 3-4 adverse events and improved quality of life
- Optimal patient selection, sequencing, and monitoring of 177Lu-PSMA-617 will continue to evolve
Presented By: Michael S. Hofman, MBBS (Hons), FRACP, FAANMS, Professor of Molecular Imaging, The University of Melbourne, and Nuclear Medicine Physician in the Centre for Cancer Imaging at the Peter MacCallum Cancer Centre in Melbourne, Australia
Written By: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, @zklaassen_md on Twitter during the 2021 European Association of Urology, EAU 2021- Virtual Meeting, July 8-12, 2021.
References:
- Hofman MS, Emmett L, Sandhu S, et al. [(177)Lu]Lu-PSMA-617 versus cabazitaxel in patients with metastatic castration-resistant prostate cancer (TheraP): A randomized, open-label, phase 2 trial. Lancet. 2021 Feb 27;397(10276):797-804.
- Sartor O, de Bono J, Chi KN et al. Lutetium-177-PSMA-617 for Metastatic Castration-Resistant Prostate Cancer. N Engl J Med. 2021 Jun 23 [Epub ahead of print].


