In the presented study, all subjects undergoing curative-intent radical cystectomy between 1994-2017 (n=1031 patients) were allocated to one of the various ten surgeons in the authors’ urology department. The endpoints that were looked at included survival outcomes (overall survival, 90-day mortality rate), surrogate cancer control, (positive margins resection rate, and a number of lymph nodes evaluated). Lastly, the blood transfusion rate was analyzed.
The median age was 67 (34-81) with 78% of the patients being males. A total of 47% had T2 disease, and 27% had T3/T4 disease, and 25% had positive node disease. 80% of the patients underwent ileal conduit reconstruction. The results demonstrated varying overall survival rates among the ten different surgeons, ranging from 42% to 78%. There was a considerable difference between the surgeons in the number of lymph nodes removed, R1 resection rates, blood transfusion rates, and 90-day mortality rates. This all demonstrated the variance and considerable differences between the surgeons in this particular institute.
Due to these results, the authors decided to implement a centralization system where the more competent surgeons with the better overall parameters, be the ones that specifically and exclusively treat these patients. The centralization system began in 2013 and is continuing up to the present day. So far, 134 patients have been enrolled in the centralization system. These patients were compared to the ones treated before the centralization system had been implemented to see if patient outcomes had improved.
No significant differences were seen between the groups in their respective age and gender. However, there was a much higher rate of patients with positive node disease in the pre-centralization era (30% vs. 17%, p<0.01). When assessing the 2-year freedom from mortality rate, there was a considerable difference in favor of the post-centralization era (84% vs. 62%, p=0.0007), as seen in figure 1. There was also a significant difference in the 90-day mortality rate (1.5% vs. 6.4%), blood transfusion rate (5% vs. 59%), positive margin rate (1.5% vs. 13%), and median number of lymph nodes removed (13% vs. 8%), all in favor of the patients in the post-centralization era.
Figure 1 – Freedom from Mortality Stratified by Era:
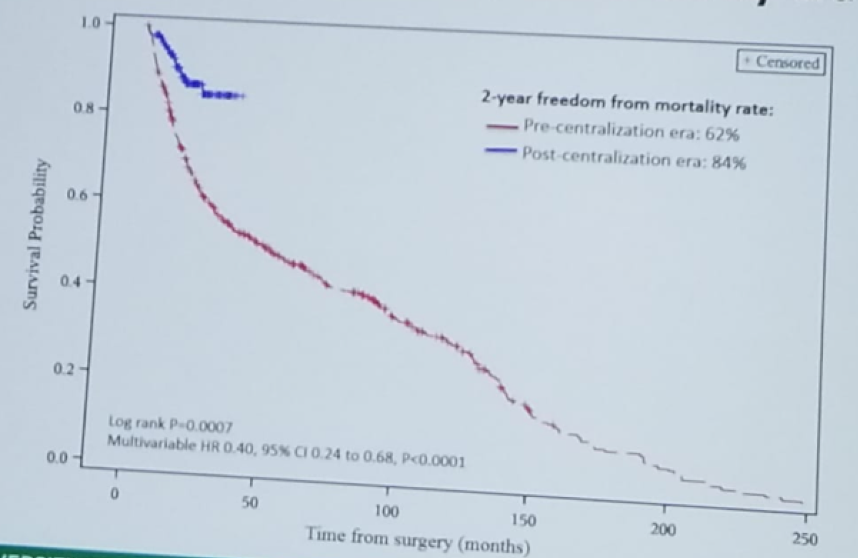
In summary, Dr. Fairey states that the patient’s likelihood of achieving optimal clinical outcomes differed depending on which urologic surgeon performed the radical cystectomy. Active centralization of radical cystectomy at the University of Alberta reduced between surgeon variation and improved clinical outcomes. Lastly, active centralization of radical cystectomy in Canada may represent a mechanism to improve and optimize overall bladder cancer quality of care.
Presented by: Adrian Fairey, MD, MS, Urologic Surgeon, Assistant Professor, Division of Urology, Department of Surgery, University of Alberta, Edmonton, Alberta, Canada
Written by: Hanan Goldberg, MD, Urologic Oncology Fellow (SUO), University of Toronto, Princess Margaret Cancer Centre, Twitter: @GoldbergHanan at the CUOS – Canadian Uro-Oncology Summit 2019, #CUOS19 January 10-12, 2019 Westin Harbour Castle, Toronto, Ontario, Canada

