For this study, the authors used the Canadian Kidney Cancer information system to prospectively identify patients from 16 institutions between 2011 and 2017 with RCC. Baseline patient, tumor, and treatment characteristics between Indigenous Canadians and non-Indigenous Canadians were performed using descriptive statistics:
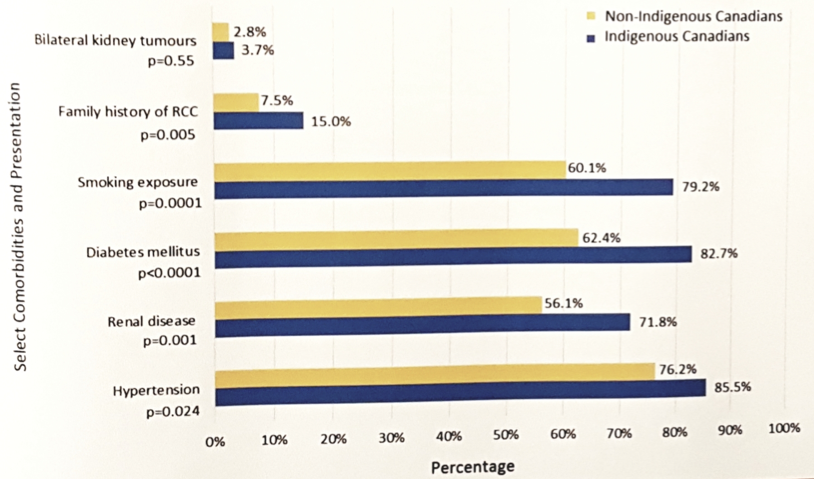
During the study period, there were 5,031 patients with RCC, of which 110 (2.2%) self-identified as Indigenous Canadians. These patients were significantly younger at the time of clinical diagnosis (mean 56.9 vs 61.2 years; p=0.0002) and had a twofold greater prevalence of family history of RCC (15% vs 7.5%; p=0.005). There was no difference in clinical stage at diagnosis between the groups (p=0.98), including those presenting with metastatic disease (10% vs 11%). Indigenous Canadians more commonly had prevalent comorbid conditions that may impact the management of RCC, including higher rates of obesity, hypertension, renal disease, diabetes mellitus, and smoking. Furthermore, Indigenous Canadians received significantly fewer renal tumor biopsies (16.4% vs 28.9%) and a lower rate of active surveillance (4.6% vs 13.1%; both p<0.05). From the time of clinical diagnosis, Indigenous Canadians had a longer median time to biopsy and surgery, however surgical, ablative, and systemic treatment rates were not different between the two groups. Over a median follow-up of >2 years for both groups, interestingly the 5-year overall survival rate was significantly higher among Indigenous Canadians compared to non-Indigenous Canadians: 93.7% vs 83.9% (p=0.025). Time to recurrence and progression between groups was comparable.
The strength of the current study is that this is the first study assessing kidney cancer outcomes among Indigenous populations in Canada. A possible limitation is that this is purely a descriptive study, likely secondary to the small sample size of Indigenous Canadians and thus small event rate precluding multivariable analysis of survival outcomes. Nonetheless, Wong concluded that Indigenous Canadians with RCC are diagnosed at an earlier age and at a similar clinical stage to non-Indigenous Canadians. Despite higher baseline comorbid diseases and longer time to biopsy and surgery, importantly, Indigenous Canadians experienced similar clinical outcomes to non-Indigenous Canadians. These findings are somewhat contradictory to studies assessing NA/AN populations in the United States and deserve further evaluation with long-term follow-up.
References:
1. Batai K, Bergersen A, Price E, et al. Clinical and molecular characteristics and burden of kidney cancer among Hispanics and Native Americans: Steps towards precision medicine. Clin Genitourin Cancer 2018;16(3):e535-e541.
Presented by: Emily Wong, MD, McMaster University, Hamilton, Ontario, Canada
Co-Authors: Anil Kapoor1, Ranjeeta Mallick2, Lori Wood3, Simon Tanguay4, Frédéric Pouliot5, Naveen S. Basappa6, Alan So7, Denis Soulières8, Darrel Drachenberg9, Luke Lavallee10, Rodney Breau10.
Author Information:
1. Urology, McMaster University, Hamilton, ON, Canada
2. Ottawa Hospital Research Institute, University of Ottawa, Ottawa, ON, Canada
3. Medical Oncology, Queen Elizabeth II Health Sciences Centre, Halifax, NS, Canada
4. Urology, McGill University Health Centre, Montreal, QC, Canada
5. Urology, Université Laval, Quebec, QC, Canada
6. Medical Oncology, Cross Cancer Institute, Edmonton, AB, Canada
7. Urology, University of British Columbia, Vancouver, BC, Canada
8. Centre Hospitalier de l'Université de Montréal, Université de Montréal, Montreal, QC, Canada
9. Urology, University of Manitoba, Winnipeg, MB, Canada
10. Urology, The Ottawa Hospital, Ottawa, ON, Canada
Written By: Zachary Klaassen, MD, Urologic Oncology Fellow, University of Toronto, Princess Margaret Cancer Centre Twitter: @zklaassen_md at the 73rd Canadian Urological Association Annual Meeting - June 23 - 26, 2018 - Halifax, Nova Scotia
8. Centre Hospitalier de l'Université de Montréal, Université de Montréal, Montreal, QC, Canada
9. Urology, University of Manitoba, Winnipeg, MB, Canada
10. Urology, The Ottawa Hospital, Ottawa, ON, Canada
Written By: Zachary Klaassen, MD, Urologic Oncology Fellow, University of Toronto, Princess Margaret Cancer Centre Twitter: @zklaassen_md at the 73rd Canadian Urological Association Annual Meeting - June 23 - 26, 2018 - Halifax, Nova Scotia

