To test his research question, Dr. Mason and his team conducted a retrospective chart review of all patients treated with RC for UC at their center from 1980 to 2017. Patients were screened if they were without neoadjuvant chemotherapy and who had a preoperative serum creatinine measurement available. Using the CKD-EPI formula, estimated glomerular filtration rate (eGFR) was calculated preoperatively and analyzed as a binary variable ≥ or < 60 mL/min/1.73m2. Cox proportional hazard regression models were calculated and risk analysis were utilized to evaluate the association between preoperative eGRF and recurrence-free survival, cancer-specific survival, and overall survival.
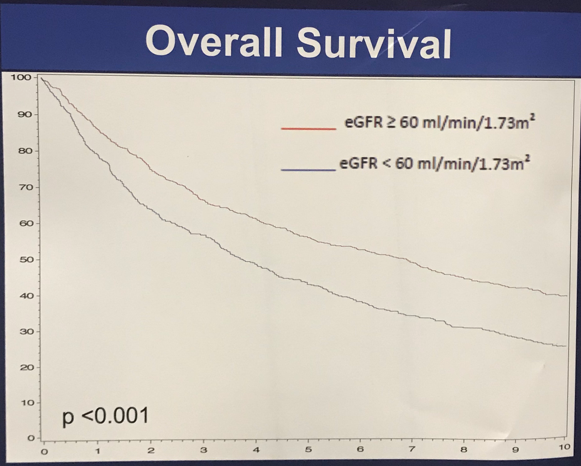
Following completion of the study, an impressive 1,232 patients were identified for inclusion in the study: 683 patients had an eGFR ≥ 60 mL/min/1.73m2 while 549 had an eGFR < 60 mL/min/1.73m2. Median age was significantly higher in the eGFR group that was < 60 mL/min/1.73m2. Median follow up was 10.7 years; 487 patients were diagnosed with recurrence, 455 died of UC, and 1,004 patients died overall. Having an eGFR < 60 mL/min/1.73m2 seemed to not be significantly associated with cancer-specific survival and recurrence-free survival. However, this cohort was associated with a significantly lower overall survival as compared to the eGFR ≥ 60 mL/min/1.73m2. The Kaplan-Meier curve illustrating this is included in the image below.
Presented by: Ross Mason, MD, Urology, Mayo Clinic, Rochester, MN, United States
Co-Authors: Bimal Bhindi1, Igor Frank1, Prabin Thapa2, Matthew K Tollefson1, Houston Thompson1, Jeffrey Karnes1, Stephen A Boorjian1
1Urology, Mayo Clinic, Rochester, MN, United States; 2Health Sciences Research, Mayo Clinic, Rochester, MN, United States
Written by: Zachary Valley, Twitter: @ZacharyAValley, Department of Urology, University of California-Irvine at the 73rd Canadian Urological Association Annual Meeting - June 23 - 26, 2018 - Halifax, Nova Scotia

