(UroToday.com) The 2023 American Urological Association (AUA) annual meeting held in Chicago, IL, was host to a moderated poster session focusing on the epidemiology and natural history of prostate cancer. Matthew Davis discussed his group’s study evaluating racial disparities in the future development of lethal prostate cancer based on PSA level measurements in midlife.
Previous analyses in Swedish and US cohorts have demonstrated that PSA levels in midlife strongly predict future rates of lethal prostate cancer.1 However, differences by race/ethnicity have yet to be fully evaluated. The objective of this study was to examine racial disparities in prostate cancer mortality based on initial midlife PSA results in a North American population.
This study included self-identified White and Black men aged 40-59 years, who received their first PSA through the Michigan health system between 1995 and 2019. Patients were assigned into one of four age categories as follows:
- 40 to 44 years
- 45 to 49 years
- 50 to 54 years
- 55 to 59 years
The primary study exposure was the first PSA test performed. This variable was operationalized based on both the median and 90th percentile value for each age group. Competing risks analysis using Fine and Grey’s semiparametric proportional hazards modeling was used to evaluate the association between this first PSA value and prostate cancer-specific mortality, stratified by race, after accounting for potential confounders such as Charlson Comorbidity Index (CCI), among others. Cancer-specific and overall mortalities were obtained via linkage to the Michigan Vital Records registry.
This study included 112,967 men, of whom 73% were White and 27% Black. Median follow-up was 6.7 years and 9.9 years for White and Black men, respectively. Median and 90th percentile PSA by race were as follows:
- White men: 0.7 and 2.0 ng/ml
- Black men: 0.7 and 2.1 ng/ml
Amongst White men, the median and 90th percentile PSA values were:
- Age 40 to 44: 0.6 and 1.3 ng/ml
- Age 45 to 49: 0.7 and 1.6 ng/ml
- Age 50 to 54: 0.7 and 2.0 ng/ml
- Age 55 to 59: 0.9 and 2.8 ng/ml
Among Black men, the median and 90th percentile PSA values were:
- Age 40 to 44: 0.6 and 1.4 ng/ml
- Age 45 to 49: 0.7 and 1.8 ng/ml
- Age 50 to 54: 0.8 and 2.4 ng/ml
- Age 55 to 59: 0.9 and 3.8 ng/ml
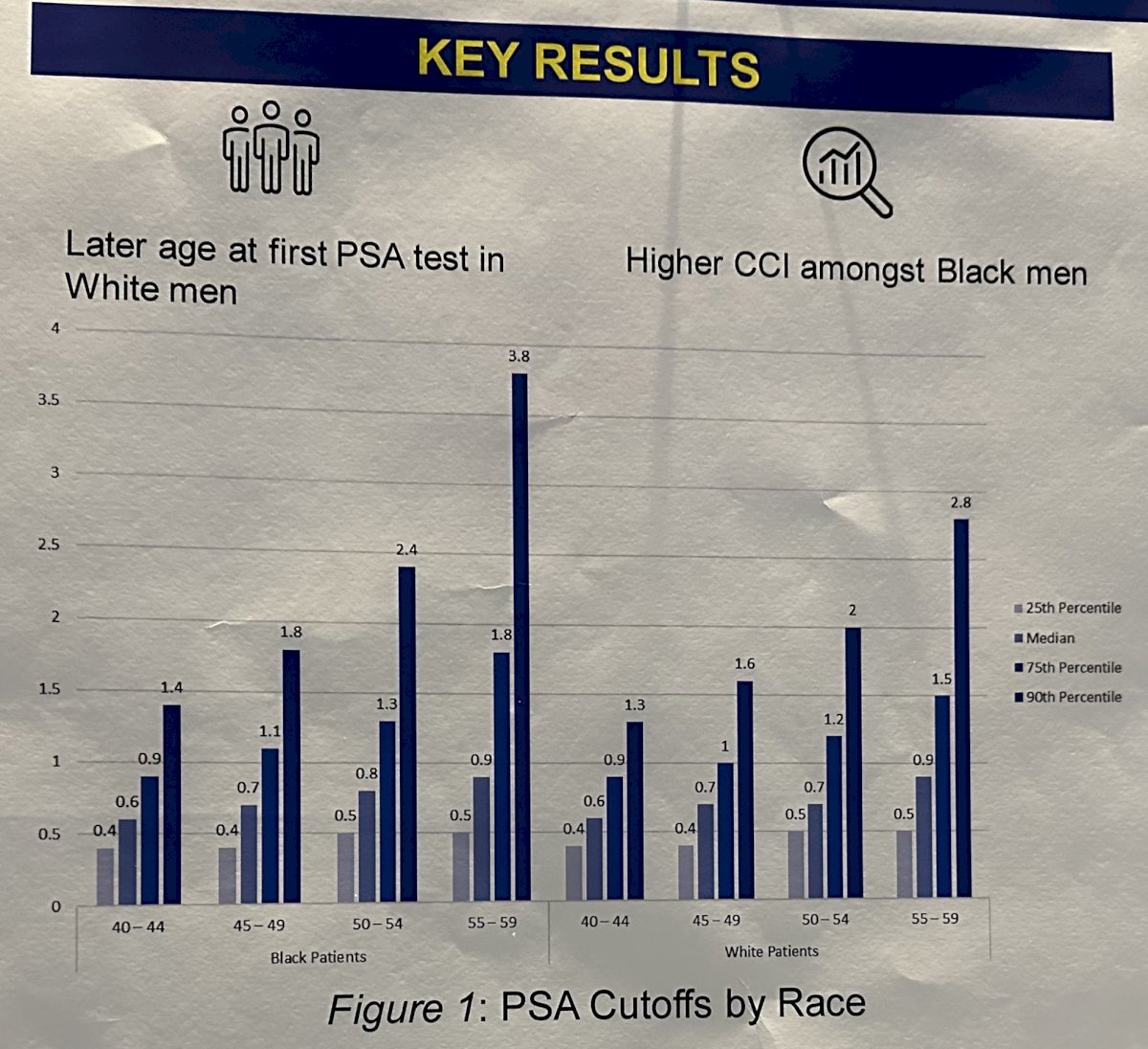
For each age category, the estimated rate of prostate cancer-specific mortality at 20 years was significantly higher in Black men when using the 90th percentile PSA cutoff. These findings were confirmed on multivariable analysis.
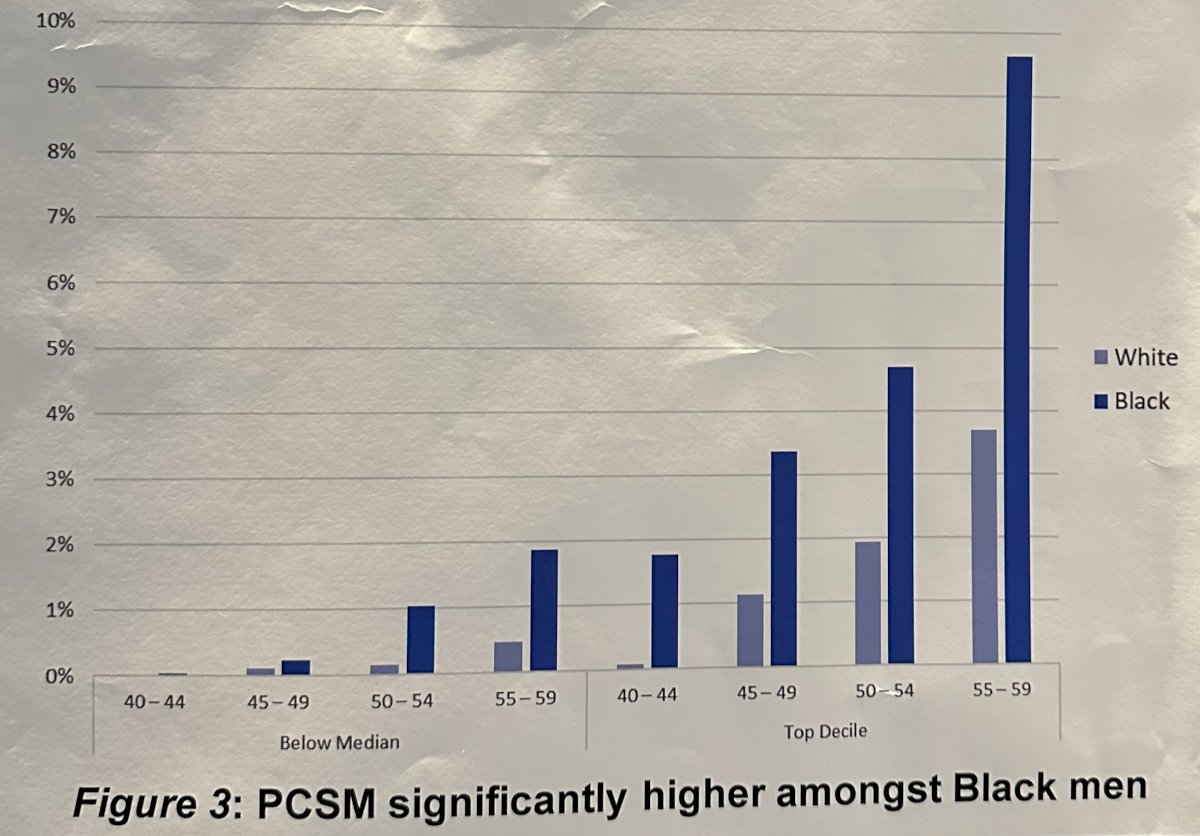
The investigators concluded that these findings suggest that Black men are significantly more likely to develop lethal PCa based on previously published midlife first-time PSA cutoffs. This information suggests that a lower midlife PSA cutoff could be considered amongst Black men when evaluating their future risks of prostate cancer-specific mortality, when compared to white men. This report is the first to examine racial disparities in lethal prostate cancer based on first-time PSA results in a diverse North American cohort.
Presented by: Matthew Davis, MD, Research Fellow at Henry Ford Health
Written by: Rashid K. Sayyid, MD, MSc – Society of Urologic Oncology (SUO) Clinical Fellow at The University of Toronto, @rksayyid on Twitter during the 2023 American Urological Association (AUA) Annual Meeting, Chicago, IL, April 27 – May 1, 2023
References:
- Preseton MA, et al. Baseline Prostate-Specific Antigen Levels in Midlife Predict Lethal Prostate Cancer. J Clin Oncol, 2016.


