(UroToday.com) In this plenary session, Dr. William Thomas Lowrance summarized the 2021 AUA/ASTRO/SUO guidelines on advanced prostate cancer, with key take-home points highlighted. The full 2 part guidelines1,2 can be found online at They are also published in the Journal of Urology.
He reiterated that these guidelines were produced by a multidisciplinary panel with representation from the AUA, ASCO, ASTRO, and SUO. They also included a patient advocate.
The aims of the guidelines are to assist in clinical decision-making and provide evidence-based guideline recommendations across the entire continuum of advanced prostate cancer.
They utilized a statement evidence rating ranging from A through C, with A representing high certainty and C representing very low certainty.
He notes off the bat that the therapeutic landscape of advanced prostate cancer now necessitates multidisciplinary patient care, including a urologist, medical oncologist, radiation oncologist, pathologist, genetic counselor, and palliative care. The treatment includes a combination of systemic therapy with or without local therapy, Advanced imaging, and germline and somatic genetic testing.
As seen in his slide below, the guidelines focus on four main patient populations. They exclude patients with localized prostate cancer and only discuss patients who are assumed to have exhausted all local therapy options. There are a separate set of guidelines for localize prostate cancer.
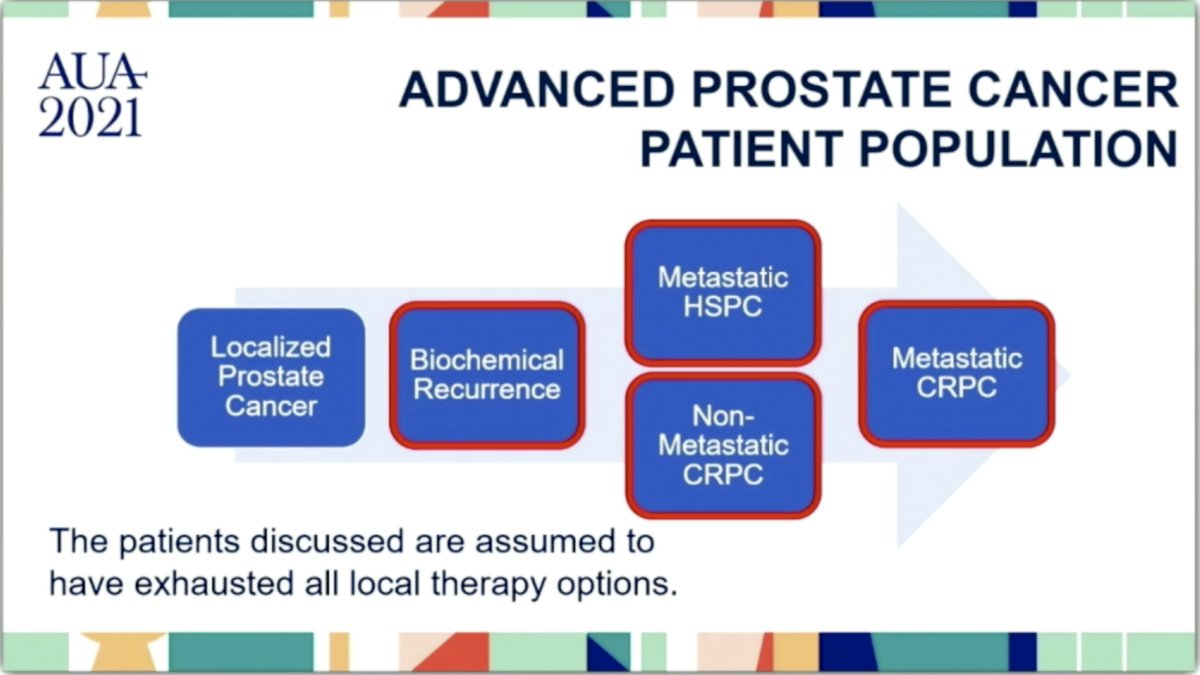
He then reviewed the key guideline recommendations for each of the above four categories which I summarize below.
1) Biochemical Recurrent Prostate CancerIn the hormone-sensitive setting, PSA recurrence almost always precedes clinical detection of metastases. In these patients the guidelines recommend:
- Clinicians should inform patients with PSA recurrence after exhaustion of local therapy regarding the risk of developing metastatic disease.
- Serial PSA measurements
- Clinical evaluation
- Staging evaluation – with conventional imaging (CT A/P or MRI and NM Bone Scan)
He notes that clinicians may consider radiographic assessments based on overall PSA and PSA kinetics (Clinical Principle), but patients can be risk-stratified. In patients who are at higher risk for the development of metastases (e.g., PSADT <12 months), they recommend that clinicians should perform periodic staging evaluations consisting of cross-sectional imaging (CT, MRI) and technetium bone scan. (Clinical Principle)
When it comes to novel PET-CT scans (e.g., fluciclovine, choline, PSMA), the authors do NOT recommend these as routine testing. However, they can be considered as an alternative to conventional imaging or in the setting of negative conventional imaging. (Expert Opinion)
As for treatment:
- If there is no demonstrated metastatic disease by conventional imaging, clinicians should offer observation or clinical trial enrollment.
- They recommend AGAINST routine use of ADT in this setting - ADT should not be routinely initiated in this population (Expert Opinion). However, if ADT is initiated in the absence of metastatic disease, intermittent ADT may be offered in lieu of continuous ADT due to a lower side effect profile.
2) Metastatic Hormone Sensitive Prostate Cancer (mHSPC)
This category encompasses men with radiographically evident metastatic disease who are still hormone-sensitive. The presence and extent of metastatic disease plays a central role in determining which and if any therapy is beneficial. Hence, they recommend the following:
- Radiographic assessment with conventional imaging of extent of disease burden (bone, lymph node and visceral metastasis) – stratify into high and low volume metastatic burden
- High-volume is defined as greater than or equal to four bone metastases with at least one metastasis outside of the spine/pelvis and/or the presence of visceral metastases. (Moderate Recommendation: Evidence Level: Grade B) - Discussion of symptoms – evaluate if patient is experiencing any symptoms from metastatic burden
- Baseline and Serial PSA - Clinicians should obtain a baseline PSA and serial PSAs at 3-6 intervals after initiation of ADT in mHSPC patients and consider periodic conventional imaging
- Genetic counseling and germline geniting testing – for all men regardless of age and family history
Clinicians should offer ADT with either LHRH agonists or antagonists or surgical castration in patients with mHSPC.
The treatment options for this patient population include:- ADT with LHRH agonist/antagonist or surgical castration
- Continued ADT with androgen pathway directed therapy (enzalutamide, apalutamide, abiraterone) or chemotherapy (docetaxel)
- Trials Supporting Docetaxel: CHAARTED, STAMPEDE
- Trials Supporting Abiraterone: LATITUDE, STAMPEDE
- Trials Supporting Enzalutamide: ARCHES, ENZAMET
- Trials Supporting Apalutamide: TITAN
- ADT with primary radiotherapy to the prostate – in low volume disease.
They note that clinicians should not offer first generation antiandrogens (bicalutamide, flutamide, nilutamide) in combination with LHRH agonists in patients with mHSPC, except to block testosterone flare. They also note that clinicians should not offer oral androgen pathway directed therapy (e.g., abiraterone acetate plus prednisone, apalutamide, bicalutamide, darolutomide, enzalutamide, flutamide, nilutamide) without ADT for patients with mHSPC.
3) Non-metastatic Castration Resistant Prostate Cancer (nmCRPC, cM0 CRPC)
This category includes men with a rising PSA but no visible metastatic disease on conventional imaging despite medical or surgical castration. This represents a uniquely distinct disease state. For patients with this condition, monitoring includes:- Serial PSA every 3-6 months
- Conventional Imaging every 6-12 months
Recently three androgen receptor antagonist were approved for these patients as they demonstrated prolonged metastasis free survival compared to ADT Plus placebo. These include abiraterone, enzalutamide, apalutamide. The data from the key trials are listed below:

He highlighted the fact that PSADT could risk stratify patients for receipt of AR directed therapies.
- Clinicians should offer apalutamide, darolutamide, or enzalutamide with continued ADT to nmCRPC patients at high risk for developing metastatic disease (PSADT ≤10 months).
- Clinicians may recommend observation with continued ADT to nmCRPC patients, particularly those at lower risk (PSADT >10 months) for developing metastatic disease.
In this disease space, chemotherapy and immunotherapy should not be offered outside of clinical trial.
4) Metastatic castration-resistant prostate cancer (mCRPC)
The treatment of patients with mCRPC has drastically changed over the past decade, there are now numerous treatment options for these patients.
Patients with mCRPC require a thorough prognostic assessment, including:- baseline labs (psa, testosterone, LDH, Hgb, alkaline phosphatase)
- Disease related symptom assessment
- Performance Status
- Conventional staging imaging – at least annually or based on patient symptoms
- Germline and somatic tumor testing – for all patients - to identify DNA repair deficiency mutations (DDR mutations) and microsatellite instability (MSI) status that may inform prognosis and counseling regarding family risk as well as potential targeted therapies.
Since the initial approval of docetaxel, there have been multiple agents that have demonstrated survival benefit on the strength of randomized controlled trials. These agents have been tested in multiple “disease states” within mCRPC.
He did not delve into a great deal of detail of the various trials that led to these medications being approved. However, he did summarize the key indications for their use.
- Continued ADT – all patients should be maintained on continued ADT
- Abiraterone, enzalutamide or docetaxel - All patients should be offered continued ADT with abiraterone acetate plus prednisone, docetaxel, or enzalutamide. (Strong Recommendation; Evidence Level: Grade A [abiraterone acetate plus prednisone and enzalutamide]/B [docetaxel])
- Sipaleucil-T - can be offered to patients with mCRPC patients who are asymptomatic or minimally symptomatic
- Radium-223 – can be offered to patients with symptoms from bony metastases from mCRPC and without known visceral disease or lymphadenopathy >3cm.
- Cabazitaxel
- In mCRPC patients who received prior docetaxel chemotherapy with or without prior abiraterone acetate plus prednisone or enzalutamide for the treatment of CRPC, clinicians may offer cabazitaxel
- In mCRPC patients who received prior docetaxel chemotherapy and abiraterone acetate plus prednisone or enzalutamide, clinicians should recommend cabazitaxel rather than an alternative androgen pathway directed therapy. - Olaparib / PARP inhibitors - Clinicians should offer a PARP inhibitor to patients with deleterious or suspected deleterious germline or somatic homologous recombination repair gene-mutated mCRPC following prior treatment with enzalutamide or abiraterone acetate, and/or a taxane-based chemotherapy. If that cannot tolerate a PARP inhibitor, these patients should be considered for platinum based chemotherapy.
- Pembrolizumab – for patients with mismatch repair deficient or microsatellite instability high mCRPC, pembro should be considered.
In sequencing the above therapies, clinicians should consider prior treatment and consider recommending therapy with an alternative mechanism of action. Therefore, if a certain AR targeted agent fails, subsequent therapy should not be another AR targeted agent.
5) Bone Health
His last section of the guidelines focused on bone health. He notes that several factors conspire to place the average patient with metastatic prostate cancer at a higher risk of bone complications, including:
- Patients with prostate cancer tend to be older, and there is a component of age-related osteoporosis
- Patients with advanced prostate cancer are exposed to ADT which has a demonstrated deleterious effects on bone mineral density
- Prostate cancer has a tendency to metastasize to the bone hence pathologic fractures are also a concern
Based on these guidelines recommend the following:
- Clinicians should recommend preventative treatment for fractures and skeletal-related events, including supplemental calcium, vitamin D, smoking cessation, and weight-bearing exercise, to advanced prostate cancer patients on ADT.
- In advanced prostate cancer patients at high fracture risk due to bone loss, clinicians should recommend preventative treatments with bisphosphonates or denosumab and referral to physicians who have familiarity with the management of osteoporosis when appropriate.
- Clinicians should prescribe a bone-protective agent (denosumab or zoledronic acid) for mCRPC patients with bony metastases to prevent skeletal-related events.
Concluding remarks:
Lastly, he noted that there are several key areas of future research that have not been fully integrated into the guidelines including:
- Integration of multidisciplinary care
- Advanced PET imaging
- Biomarkers
- Other systemic therapies
These will likely need to be included in the future as their level of evidence increases.
Presented by: William Thomas Lowrance, MD, MPH, MBA, Assistant professor in the Division of Urology at the University of Utah School of Medicine, Bon Secours Mercy Health
Written by: Thenappan (Thenu) Chandrasekar, MD – Urologic Oncologist, Assistant Professor of Urology, Sidney Kimmel Cancer Center, Thomas Jefferson University, @tchandra_uromd on Twitter during the 2021 American Urological Association, (AUA) Annual Meeting, Fri, Sep 10, 2021 – Mon, Sep 13, 2021.
References:
1. Lowrance WT, Breau RH, Chou R et al: Advanced Prostate Cancer: AUA/ASTRO/SUO Guideline PART I. J Urol 2021; 205: 14
2. Lowrance WT, Breau RH, Chou R et al: Advanced Prostate Cancer: AUA/ASTRO/SUO Guideline PART II. J Urol 2021; 205: 22.


