215 men on AS with Gleason score (GS) 3+3 and low volume (≤33% positive cores) GS 3+4 PCa who underwent GPS testing at diagnostic or confirmatory biopsy within 24 months at the University of California San Francisco (UCSF) were evaluated. Patients had stage T1 or T2 disease, PSA <20, and clinical Cancer of the Prostate Risk Assessment (CAPRA) score <6. The primary outcome was adverse pathology at delayed RP, defined as GS ≥ 4+3, and/or stage≥ pT3a or pN1. Cox proportional hazards regression was performed to evaluate the association between GPS and adverse pathology, adjusting for age at diagnosis, clinical CAPRA at diagnosis, PSA density at the time of GPS, whether the patient had an additional GPS test, and whether the biopsy was performed at UCSF.
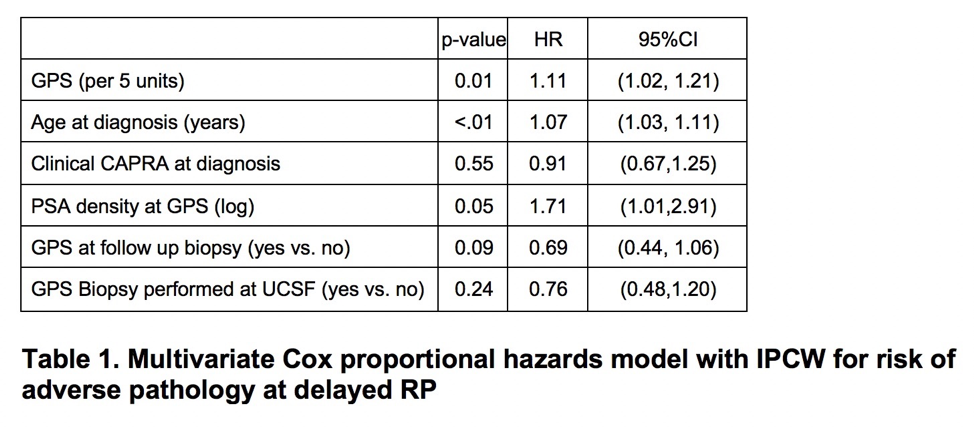
Dr. Kornberg then summarized the results of this study. 83% of men (N=179) were low risk, and 17% of men (N=36) were intermediate risk by CAPRA scoring. Median GPS was 26.4. Median time from diagnosis to RP was 23 months. 121 men had adverse pathology on delayed RP at a median time of 26 months to prostatectomy. In a multivariate proportional hazards model, GPS was associated with increased risk of adverse pathology at delayed RP (Hazard Ratio per 5 units: 1.11, 95% CI: 1.02). Age at diagnosis was the only other covariate associated with adverse pathology.
Dr. Kornberg summarized that in patients who undergo radical prostatectomy after a relatively short period on active surveillance, a higher Genomic Prostate Score is associated with an increased risk for adverse pathology.
Presented by: Zachary Kornberg, Staff Research Associate, University of California, San Francisco, CA
Written by: Abhishek Srivastava, MD, Society of Urologic Oncology Fellow, Fox Chase Cancer Center, Philadelphia, PA, Twitter: @shekabhishek at the American Urological Association's 2019 Annual Meeting (AUA 2019), May 3 – 6, 2019 in Chicago, Illinois

