According to Dr. Kerr, almost two-thirds of women report waking up at night at least twice by the age of 70. Previous studies show prevalence of nocturia increases with age for men and women (Figure 1). As a result, this condition is viewed as a normal part of aging by patients and clinicians.

Figure 1.
Dr. Kerr pointed out that a degree of bother wasn’t previously considered as an important characteristic of patient’s quality of life. Research shows that bother is positively correlated to the number of nocturic episodes. The immediate effects and long-term consequences can explain poor quality of life caused by nocturia. Daytime drowsiness, decreased daytime energy and concentration, altered mood and memory are examples of short-term outcomes. Long-term effects include increased risk of mortality, severe sleep and mood disturbances, high risk for falls and subsequent fractures. Figure 2 shows a link between nocturia and mortality.
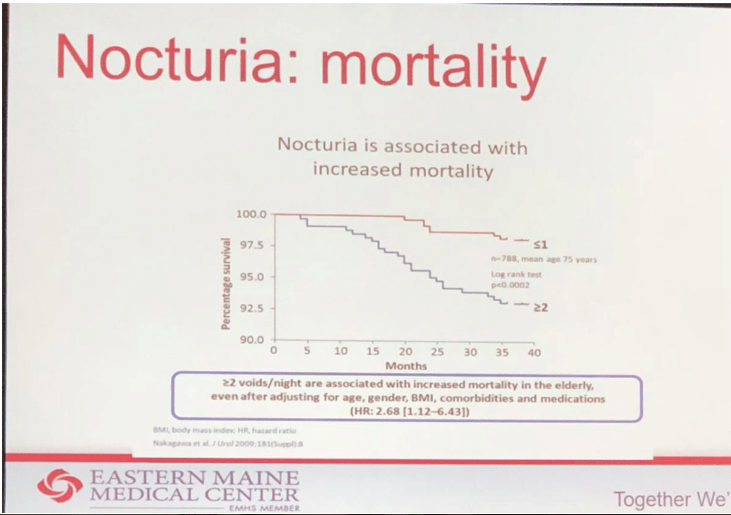
Figure 2.
How should nocturia be evaluated in a medical practice? Dr. Kerr proposed to start with a three-day frequency volume chart (FVC) followed by medical history collection and physical exam. While FVC will allow establishing a type of nocturia, medical history and physical will help to show underlying medical conditions (hypertension, arthritis, depression/anxiety, COPD, sleep apnea, diabetes mellitus or insipidus) or medications (lithium , SSRIs, tetracycline, calcium channel blockers, ketamine, etc.) that could be causing this symptom.
Medical assessment of nocturia was summarized in Figure 3.

Figure 3.
Finally, presenter reviewed novel diagnostic tools and available treatment options for nocturnal polyuria. Quality of Life – INTU QoL PRO Impact of Nighttime Urination is a new questionnaire developed to assess nocturia’s impact on mood, energy and irritability. Other survey instruments include N-QoL and ICIQ-nQoL.
Treatment choice would depend on a type of nocturia (global polyuria, reduced bladder capacity, nocturnal polyuria, and mixed disorders) and corresponding health outcomes. Previous data show that overactive bladder medications improve nocturia only if patient has already been diagnosed with OAB. If there are no abnormalities on the voiding diary, sleep disorders, psychological problems, and lifestyle choices should be considered.
Antidiuretic therapy with desmopressin was named as an only FDA-approved treatment option for people with nocturnal polyuria. It comes in a form of IV, tablet, melt, and nasal spray. While desmopressin is linked to the development of hyponatremia, this adverse event can be avoided by monitoring serum sodium levels and offering a low dose of medication (Noctiva nasal spray).
Presented by: Lindsey A. Kerr, MD, Pelvic Care and Continence Specialists, Eastern Maine Medical Center, Bangor, ME
Written by: Hanna Stambakio, BS, Clinical Research Coordinator, Division of Urology, University of Pennsylvania

