(UroToday.com) The 2022 GU ASCO Annual meeting included a prostate cancer oral abstract session featuring Dr. Kim Chi and colleagues presenting the first results of the MAGNITUDE phase 3 trial assessing niraparib with abiraterone acetate and prednisone as first-line therapy in patients with metastatic castration-resistant prostate cancer (mCRPC) with and without HRR gene alterations.
Up to 30% of patients with mCRPC have alterations in genes associated with HRR and are responsive to PARP inhibitors such as niraparib. Androgen receptor signaling regulates DNA repair in prostate cancer, providing a rationale for combined androgen receptor targeting with PARP inhibitor. Niraparib, a potent inhibitor of PARP1 and PARP2, has anti-tumor activity in heavily pretreated patients with HRR-gene altered mCRPC. The MAGNITUDE trial assessed whether adding niraparib to abiraterone acetate/prednisone improves outcomes in patients with mCRPC with or without alterations in HRR associated genes.
MAGNITUDE (NCT03748641) is a randomized, double-blind phase 3 study. In eligible mCRPC patients, ≤4 months of prior abiraterone acetate/prednisone for mCRPC was allowed. Patients with (HRR biomarker positive: ATM, BRCA1, BRCA2, BRIP1, CDK12, CHEK2, FANCA, HDAC2, PALB2) and without specified gene alterations (HRR biomarker negative) were randomized 1:1 to receive niraparib 200 mg once daily + abiraterone acetate/prednisone or placebo + abiraterone acetate/prednisone. The primary endpoint was radiographic progression-free survival (rPFS) assessed by blinded independent central review in the BRCA1/2 group followed by all HRR biomarker positive patients. Secondary endpoints were time to initiation of cytotoxic chemotherapy, time to symptomatic progression, and overall survival. Other endpoints included time to PSA progression and objective response rate. The trial design for MAGNITUDE is as follows:
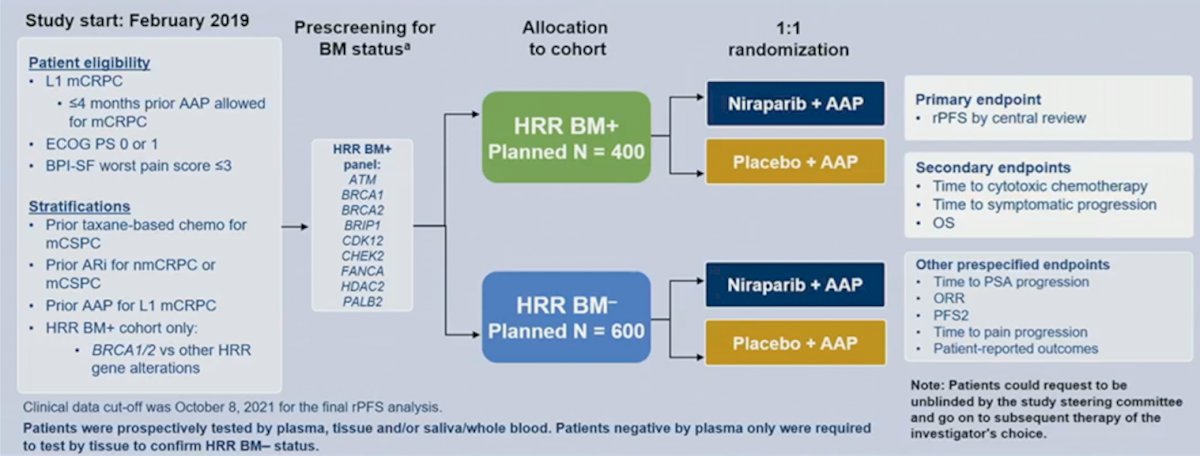
The MAGNITUDE statistical analysis plan included a prospective a priori approach to examining outcomes in HRR biomarker positive and HRR biomarker negative cohorts. In the HRR biomarker negative cohort, a prespecified futility analysis was planned after enrolling ~200 of a planned 600 patients and ~125 composite progression events (first of either radiographic or PSA progression or death). IDMC was to recommend whether the HRR biomarker negative cohort should continue or discontinue enrollment to support patient safety and prevent overtreatment. In the HRR biomarker positive cohort, the primary and secondary endpoints were tested using a prespecified statistical hypothesis testing strategy to control the family-wise Type I error rate at a 2-sided level of 0.05. For the primary endpoint, the BRCA1/2 subgroup was specifically powered and tested first and if statistical significance was reached all HRR biomarker positive patients were to be tested. A total of 400 patients were planned to be enrolled into the HRR biomarker positive cohort; ~50% were to be BRCA1/2 positive.
The preplanned futility analysis in 233 HRR biomarker negative patients showed no benefit of adding niraparib to abiraterone acetate/prednisone in the prespecified composite endpoint (first of PSA progression or rPFS: HR 1.09, 95% CI 0.75-1.59):

There were 423 HRR biomarker positive patients randomized to niraparib + abiraterone acetate/prednisone (n = 212) or placebo + abiraterone acetate/prednisone (n = 211). The median age was 69 years, 23% had prior abiraterone acetate/prednisone, 21% had visceral metastases, and 53% had BRCA1/2 mutations. The baseline characteristics for the HRR biomarker positive cohort are as follows:

The median follow-up for this analysis was 18.6 months. Niraparib + abiraterone acetate/prednisone significantly improved rPFS by blinded independent central review in the BRCA1/2 subgroup reducing the risk of progression or death by 47% (16.6 vs 10.9 months)

and in all HRR biomarker positive patients by and 26% (16.5 vs 13.7 months; HR 0.74, 95% CI 0.57-0.97). Investigator assessed rPFS was consistent with blinded independent central review. Niraparib + abiraterone acetate/prednisone delayed time to initiation of cytotoxic chemotherapy (HR 0.59, 95% CI 0.39-0.89)
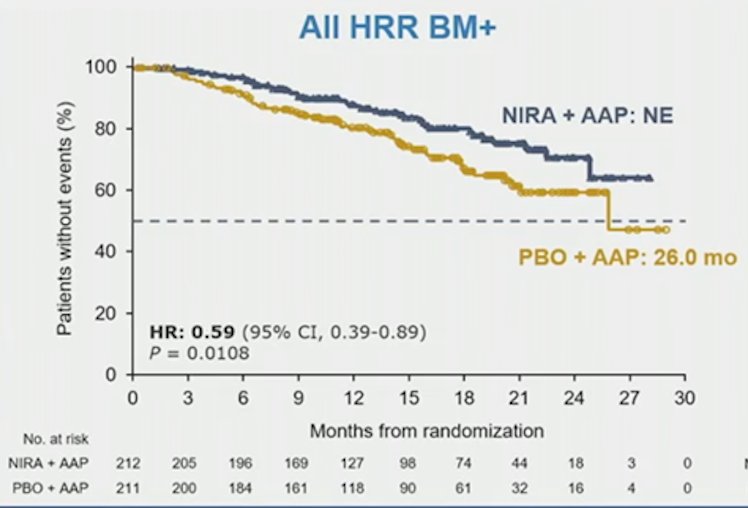
time to symptomatic progression (HR 0.69, 95% CI 0.47-0.99)
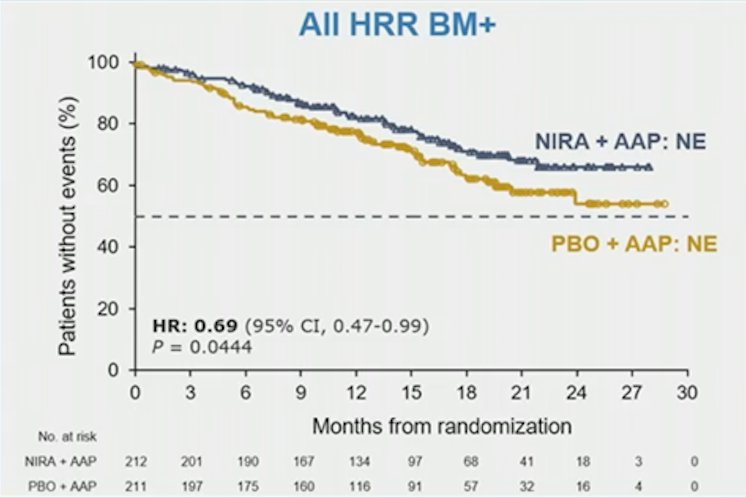
and time to PSA progression (HR 0.57, 95% CI 0.43-0.76)
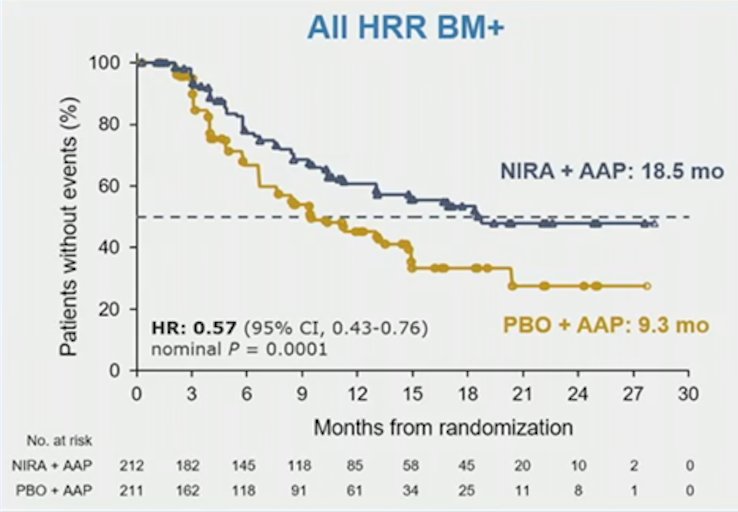
as well as improved objective response rate in HRR biomarker positive patients. At the time of the first interim analysis, overall survival data is immature (27% of deaths observed: HR 0.767, 95% CI 0.525-1.119). No new safety signals were seen. In HRR biomarker positive patients, 67% and 46.4% had grade 3/4 adverse events and 9% and 3.8% discontinued treatment in the niraparib + abiraterone acetate/prednisone and placebo + abiraterone acetate/prednisone arms, respectively. There were no clinically significant differences in overall quality of life (FACT-P):

Dr. Chi provided the following summary points for the MAGNITUDE trial:
- MAGNITUDE was pragmatically designed to test the benefit of the combination of niraparib + abiraterone acetate/prednisone for mCRPC in patients prospectively identified with and without alterations in genes associated with HRR using both tissue and blood-based approaches
- There was no benefit was observed with niraparib + abiraterone acetate/prednisone in patients who were HRR biomarker negative
- Niraparib + abiraterone acetate/prednisone significantly improved the primary clinical outcome in HRR biomarker positive patients:
- 47% improvement in rPFS in patients with BRCA 1/2 alterations and 27% across all HRR biomarker positive patients
- 41% improvement in time to cytotoxic chemotherapy
- 31% improvement in time to symptomatic progression
- 43% improvement in PSA progression
- Higher rate of objective response (including complete responses) with a relative risk of 2.13
- Niraparib + abiraterone acetate/prednisone had a manageable safety profile with no new safety signals identified and health-related quality of life was maintained
Dr. Chi concluded noting that MAGNITUDE highlights the importance of testing for HRR gene alterations in patients with mCRPC, to identify who will optimally benefit from the combination of niraparib + abiraterone acetate/prednisone. The MAGNITUDE study results support niraparib + abiraterone acetate/prednisone as a new first-line treatment option for patients with mCRPC and alterations in genes associated with HRR.
Presented By: Kim N. Chi, MD, FRCP(C), University of British Columbia, BC Cancer-Vancouver Center, Vancouver, BC, Canada
Co-Authors: Dana E. Rathkopf, Matthew Raymond Smith, Eleni Efstathiou, Gerhardt Attard, David Olmos, Ji Youl Lee, Eric Jay Small, Andrea Gomes, Guilhem Roubaud, Marniza Saad, Bogdan Zurawski, Valerii Sakalo, Gary Mason, Adam del Corral, George C. Wang, Daphne Wu, Brooke Diorio, Angela Mennicke Lopez- Gitlitz, Shahneen Kaur Sandhu
Affiliations: Memorial Sloan Kettering Cancer Center and Weill Cornell Medical College, New York, NY, Massachusetts General Hospital Cancer Center and Harvard Medical School, Boston, MA, Houston Methodist Cancer Center, Houston, TX, University College London, London, United Kingdom, Department of Medical Oncology, Hospital Universitario 12 de Octubre. Instituto de Investigación Sanitaria Hospital 12 de Octubre (imas12), Seoul St. Mary's Hospital, The Catholic University of Korea, Seoul, South Korea, University of California San Francisco, Helen Diller Family Comprehensive Cancer Center, San Francisco, CA, Liga Norte Riograndense Contra O Câncer, Department of Medical Oncology, Institute Bergonié, Department of Clinical Oncology, University of Malaya Medical Centre, Kuala Lumpur, Malaysia, Department of Outpatient Chemotherapy, Professor Franciszek Lukaszczyk Oncology Center, Bydgoszcz, Poland, Kyiv City Clinical Oncology Center, Kyiv, Ukraine, Janssen Research & Development, Spring House, PA, Janssen Research & Development, Bridgewater, NJ, Janssen Research & Development, Los Angeles, CA, Janssen Research & Development, Titusville, NJ, Peter MacCallum Cancer Center and the University of Melbourne, Melbourne, Australia
Written by: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, @zklaassen_md on Twitter during the 2022 Genitourinary (GU) American Society of Clinical Oncology (ASCO) Annual Meeting, San Francisco, Thurs, Feb 17 – Sat, Feb 19, 2022.


