(UroToday.com)The 2022 Genitourinary (GU) American Society of Clinical Oncology (ASCO) Annual Meeting included a prostate cancer session highlighting work from Dr. Kim Chi and colleagues presenting results of their study assessing exposure-adjusted safety analyses of the phase 3 VISION trial of 177Lu-PSMA-617 in patients with metastatic castration-resistant prostate cancer (mCRPC). In the VISION trial,1 targeted radioligand therapy with 177Lu-PSMA-617 significantly prolonged radiographic progression free survival (rPFS) and overall survival when added to standard of care in patients with advanced prostate-specific membrane antigen (PSMA)-PET-positive mCRPC. There was a higher incidence of treatment-emergent adverse events with 177Lu-PSMA-617 + standard of care vs standard of care. However, treatment exposure was more than three times longer in the 177Lu-PSMA-617 + standard of care arm and thus relative toxicity may have been overestimated. Presented at GU ASCO 2022, a post hoc analysis of the relationship between exposure and frequency of treatment-emergent adverse events was performed to facilitate the comparison of rates between arms.
In this international, open-label study, adult patients previously treated with ≥ 1 androgen receptor pathway inhibitors and 1–2 taxane regimens were randomized 2:1 to 177Lu-PSMA-617 (7.4 GBq Q6W, ≤ 6 cycles) + standard of care or standard of care alone. Safety was a secondary endpoint in this phase 3 trial. Treatment-emergent adverse events (regardless of causality) were reported from start of randomized treatment for up to 30 days after last treatment administration (including standard of care) or 1 day before subsequent anticancer treatment, whichever occurred first. Overall treatment-emergent adverse event incidence was adjusted for treatment exposure by calculating incidence per 100 patient treatment years. The analysis was performed for the first occurrence of treatment-emergent adverse events.
Exposure-adjusted incidence of any grade, grade ≥ 3, and selected treatment-emergent adverse events are listed in the following table:
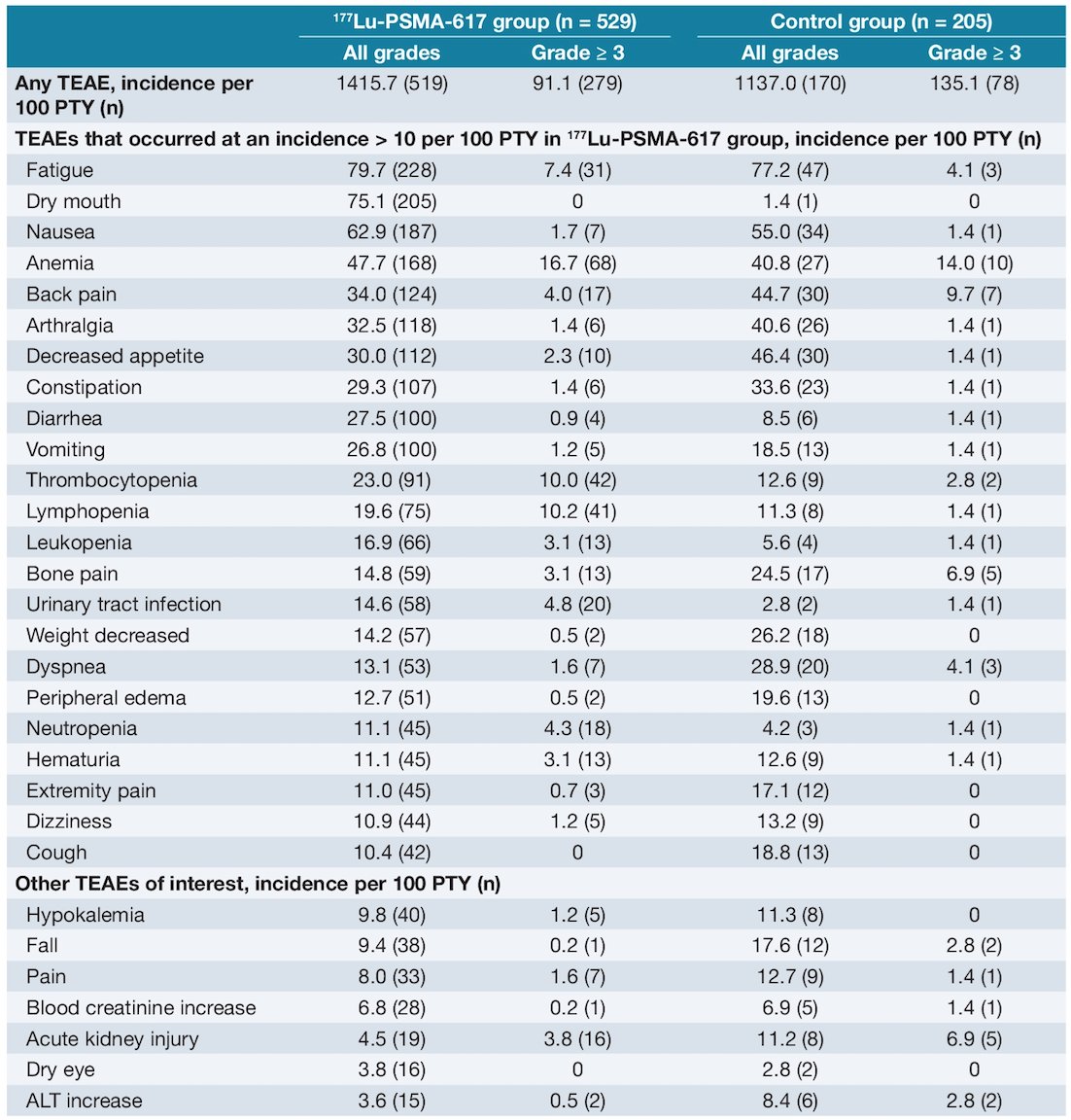
There was similar exposure-adjusted incidence of gastrointestinal events and fatigue
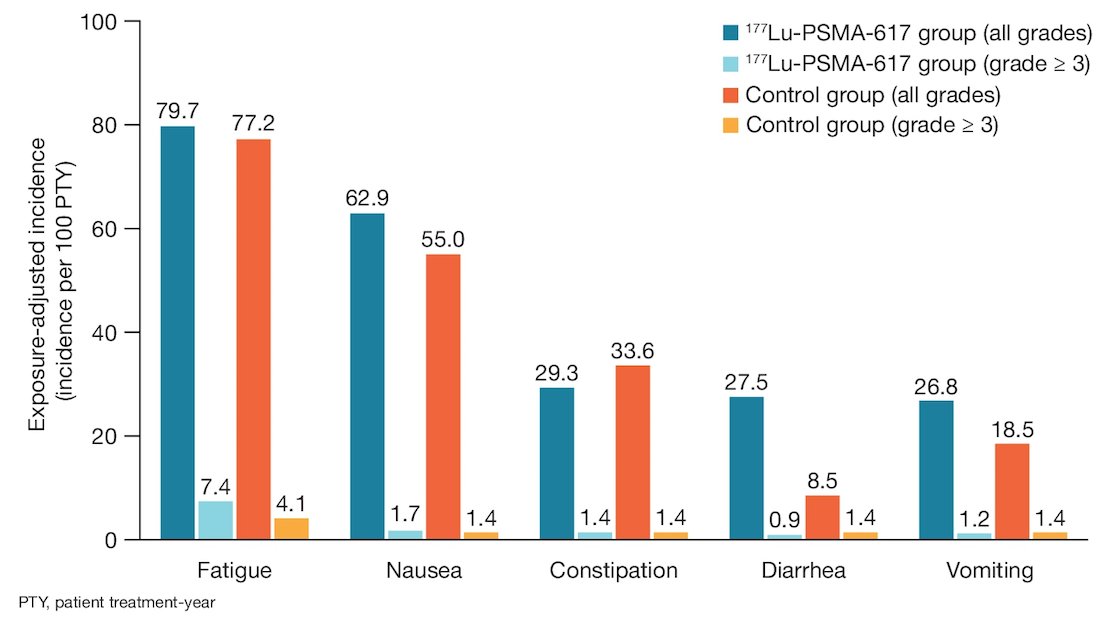
and higher exposure-adjusted incidence of musculoskeletal and renal events with standard of care compared with 177Lu-PSMA-617 + standard of care suggesting an association with treatment exposure rather than 177Lu-PSMA-617:

Dry mouth, dry eye and acute myelosuppression maintained a higher incidence, confirming relationship with 177Lu-PSMA-617 treatment:

Dr. Chi concluded this assessment of exposure-adjusted safety analyses of the VISION trial of 177Lu-PSMA-617 in patients with mCRPC with the following take-home messages:
- Treatment exposure was more than three times longer in the 177Lu-PSMA-617 group than in the control group
- The adjusted safety analysis, accounting for a longer safety observation due to longer rPFS in patients receiving 177Lu-PSMA-617, reveals a comparable incidence of treatment-emergent adverse events between arms
- The adjusted analysis provides evidence that dry mouth, dry eye, and acute myelosuppression have a relationship with 177Lu-PSMA-617 treatment
- This confirms a favorable risk/benefit profile of 177Lu-PSMA-617 added to standard of care in this patient population
- Future analyses are planned to examine the relationship of the duration and recurrence of treatment-emergent adverse events with 177Lu-PSMA-617
Presented by: Kim N. Chi, BC Cancer Agency, University of British Columbia, Vancouver, BC, Canada
Co-Authors: Nabil Adra, Rohan Garje, Jeff M. Michalski, Jules Lavalaye, Mette Moe Kempel, Marcia Brackman, Kevin Perraud, Geoffrey Holder, Andrew J. Armstrong
Written by: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, @zklaassen_md on Twitter during the 2022 Genitourinary (GU) American Society of Clinical Oncology (ASCO) Annual Meeting, San Francisco, Thurs, Feb 17 – Sat, Feb 19, 2022.
References:

