(UroToday.com) In an oral abstract on the third day of the American Society for Clinical Oncology (ASCO) Genitourinary Cancer Symposium 2022 focused on renal cell cancer, Dr. Bex presented results of the NeoAvAx study examining neoadjuvant avelumab and axitinib following nephrectomy for patients who are at high risk for recurrence.
In the past five years, combination therapy with immune checkpoint inhibition has become the standard of care as first line therapy for patients with metastatic renal cell carcinoma (mRCC). Subsequently, combination therapy including both immune checkpoint inhibitor and vascular endothelial growth factor (VEGF) inhibitors have shown benefit and have become a standard first line treatment approach. In kidney cancer, neoadjuvant therapy may be considered for primary tumor downstaging and to reduce the risk of recurrence. For patients with high-risk RCC, five-year recurrence rates are 60%.
The NeoAvAx trial tests the neoadjuvant use of a combination of the immune checkpoint inhibitor avelumab and the VEGF-inhibitor axitinib (NCT03341845). This single arm phase II trial enrolled adult patients (age 18 years and older) with clinically high-risk clear cell RCC, WHO performance status 0-1, and no comorbidities that preclude surgery or systemic therapy. Patients were defined as having high-risk ccRCC if they had cT1b-T2a grade 4 disease, cT2b-3a grade 3-4 disease, cT3-4 disease of any grade, or resectable node-positive disease regardless of primary tumor stage or grade.
Following enrollment, patients received 12 weeks of neoadjuvant avelumab and axitinib prior to nephrectomy.

The primary endpoint was RECIST 1.1 partial response (PR) in the primary tumor (PT) in ≥25%. Forty patients were required to demonstrate a 25% PR rate with an alpha of 0.05 and a power of 80% using a Simon two-stage minimax design. The authors further assessed a number of secondary endpoints including disease-free survival (DFS), overall survival (OS) and safety. Finally, as an exploratory analysis, the authors considered a biomarker analysis on sequential paired tissue samples including PD-L1 (SP263), CD8+, CD8-granzyme-B (CD8/GZMB)+, Foxp3+ cells, CD8/CD39+ and MHC-I on pre-treatment biopsy and nephrectomy samples from 34 patients.
Between May 2018 and October 2021, 40 patients were enrolled. The median age was 63 years (range 47-74). Eight patients (20%) had T4 disease and 17 (42.5%) had node positive disease. Baseline tumor diameter was 10.3 cm (range 5.6 to 18.8 cm) and baseline lymph node diameter (in 17 patients with nodal disease) was 2.6 cm (range 1.1 to 7.1 cm).
Twelve patients (30%) had a partial response of the primary tumor. The median primary tumor downsizing was 20% (+3.8 to -43.5%). No patient had a primary tumor progression, per RECIST v1.1.
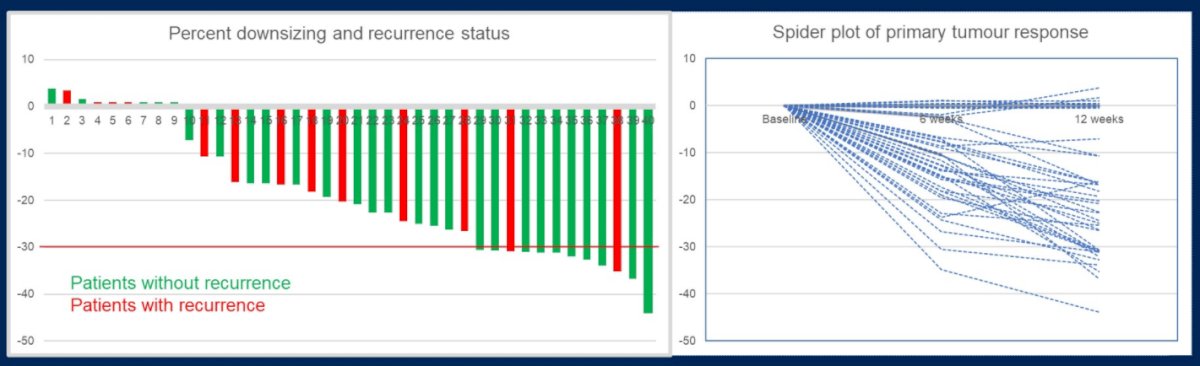
Among the 12 patients with a partial response of the primary tumor, 10 (83%) were disease-free. At a median follow-up of 23.5 months, recurrence occurred in 13 (32%) patients at a median of 8 (2-23) months and 3 died of disease. Neither median DFS nor OS were reached to date.

Intraoperative adverse events occurred in two patients with bowel damage and splenectomy each in one patient. Postoperative adverse events occurred in 13 patients, 4 of which were Clavien Dindo grade 3a (10%) and one of which was grade 4a (2.5%). All serious adverse events were attributable to either prolonged hospitalization or readmission. One patient had surgery early at week 6 for suspected tumor progression which turned out to be biopsy related hematoma and one patient had a delay of surgery for 3 weeks due to grade 2 hypothyroidism. One patient developed systemic disease with liver metastasis during neoadjuvant therapy.
Four patients had axitinib dose escalation to 10 mg PO BID, 7 to 7mg PO BID, 23 remained at the starting dose of 5 mg PO BID while 6 had a dose reduction to 3 mg PO BID. In terms of avelumab, no patients required dose reduction but 3 had a dose interruption of one cycle and 3 required discontinuation. Five patients needed hydrocortisone for an infusion related reaction.
In terms of biomarker analysis, post-treatment samples showed upregulation of PD-L1 expression (p <0.0001) and total CD8+ densities (p < 0.01) when compared to pre-treatment biopsies. Post-treatment tumor samples among those patients with recurrence had lower densities of total, intra-epithelial and stromal CD8+ and intra-epithelial CD8+CD39+ cells (all p<0.05) and total CD8+GZMB+ (p=0.1) while pre-treatment biopsies showed no clear differences.
Thus, Dr. Bex concluded that this is the first neoadjuvant trial using combination immune checkpoint inhibitor and VEGF inhibitor in patients with locally advanced high-risk RCC. A partial response was seen in 30% of patients.
Presented by: Axel Bex, MD, PhD, The Netherlands Cancer Institute


