San Francisco, California (UroToday.com) Advanced imaging is increasingly being used across all stages of prostate cancer. Dr. Jeremie Calais from UCLA Medical Center discussed who should undergo prostate specific membrane antigen (PSMA) PET imaging in the current era.
PSMA is a cell surface protein that is specific to prostate cancer and is over-expressed by 94% of prostate cancer cells making it an ideal nuclear theranostics target. A number of peer-reviewed articles have directly compared PSMA PET to other advance imaging (i.e. Choline PET or Fluciclovine PET) finding that PSMA PET is superior. This is thought to be due to the fact that PSMA over-expression is a more sensitive biological target than upregulated metabolism, which is the target of other advanced imaging modalities.
One of the most commonly used indications for PSMA PET is to evaluate for M1b (osseous metastatic) disease. A head-to-head comparison of PSMA PET with bone scan in this clinical context found that PSMA PET had improved sensitivity (96% versus 73%) and specificity (99% vs 84%).1 The relatively poorer sensitivity of bone scan is thought to be due to bone scans missing bone marrow and lytic skeletal metastases.
Another common application of PSMA PET is to rule out the presence of N1 (pelvic nodal) disease. A recent meta-analysis of 18 studies reported the following test characteristic for detecting pelvic lymph node disease: 59% sensitivity, 93% specificity, 81% positive predictive value, 85% negative predictive value.2
A multicenter prospective trial presented as an abstract (586) at the 2019 Society of Nuclear Medicine and Molecular Imaging meeting reported lower sensitivity (31-42%) but higher specificity (96-99%). The positive predictive value (78-91%) and negative predictive value (81-84%) were similar. Notably, this prospective data indicates that approximately 2/3 of patients with nodal disease will be missed by PSMA PET.
In the setting of localized prostate cancer, the impact of PSMA PET on radiation planning has been studied. Importantly, PSMA PET detects not only in-field lesions but out-of-field lesions as well. A study by Calais et al found that PSMA PET identified disease outside of the radiation field in 16% of men with intermediate or high-risk localized prostate cancer, indicating that PSMA PET in localized disease could significantly change management in a large subset of patients.3
The utility of PSMA PET for accurate T staging has been evaluated. In this setting, it seems that there is less utility as a significant proportion of localized prostate cancers are missed by PSMA PET. There is, however, a significant correlation of SUVmax on PSMA PET with Gleason grade, highlighting a potential value of utilizing PSMA PET to guide prostate biopsy.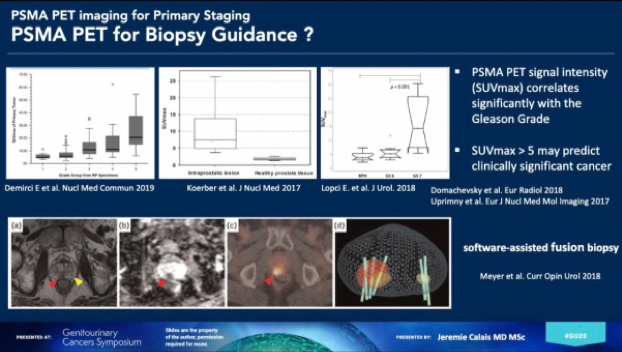
Dr. Calais concluded by highlighting that PSMA PET is re-defining prostate cancer disease stages. Examples include patients who are negative for lymph node or metastatic disease by conventional imaging, but positive on PSMA. Optimal treatment of these patients has not yet been established, though is an exciting area of active investigation in the field.
Presented by: Jeremie Calais, MD, Assistant Professor at the Ahmanson Translational Imaging Division of the Department of Molecular and Medical Pharmacology in the David Geffen School of Medicine at UCLA
Written by: Jacob Berchuck, MD, Medical Oncology Fellow at the Dana-Farber Cancer Institute (Twitter: @jberchuck) at the 2020 Genitourinary Cancers Symposium, ASCO GU #GU20, February 13-15, 2020, San Francisco, California
References:
- Lengana T, et al. 68Ga-PSMA PET/CT Replacing Bone Scan in the Initial Staging of Skeletal Metastasis in Prostate Cancer: A Fait Accompli? Clin Genitourin Cancer. 2018 Oct;16(5):392-401.
- Petersen LJ, Zacho HD. PSMA PET for primary lymph node staging of intermediate and high-risk prostate cancer: an expedited systematic review. Cancer Imaging. 2020 Jan 23;20(1):10.
- Calais J, et al. Potential Impact of 68Ga-PSMA-11 PET/CT on the Planning of Definitive Radiation Therapy for Prostate Cancer. J Nucl Med. 2018 Nov;59(11):1714-1721.


