Based on the IGCCCG classification update from ESMO 2019, data suggests that overall survival at the five year mark has improved since 1997 from 48% to 67%. What is driving this improvement. The presenter argues that this is not from significant improvements in the chemotherapy regimen used and showed the below table of essentially negative trials (with the exception of Fizazi 2014) for changing standard of care chemotherapy. The dose dense high intensity regimen from Fizazi in 2014 that conferred improved PFS in patients that did not have a satisfactory tumor marker decrease while undergoing BEP has not been widely adopted, perhaps in part due to the complexity of the regimen.
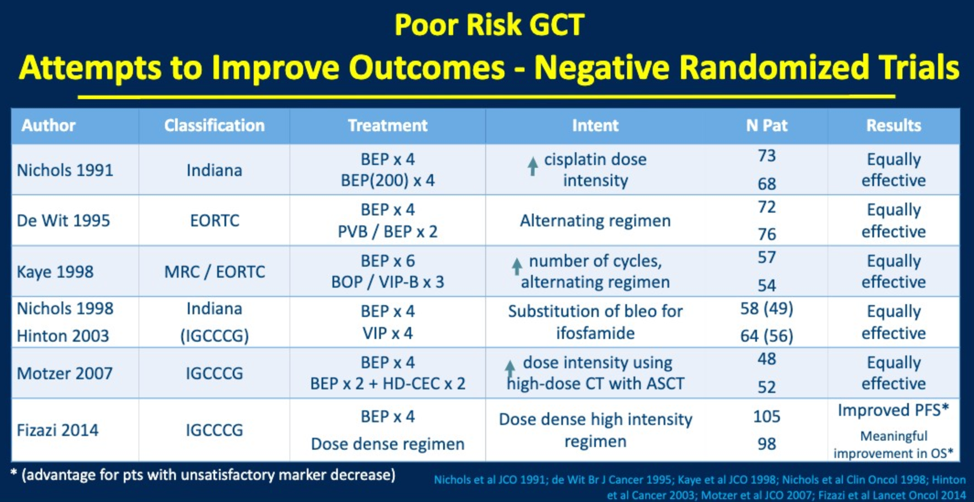
Rather, Dr. Kollmansberger argues that increased adoption of the standard of care regimen and guideline-based care, more appropriate utilization of post-chemotherapy surgery, and improved supportive care (including venous thromboembolism recognition and management) are being improved patient outcomes.
The presenter then reviewed the standard of care therapeutic options for poor-risk metastatic testicular germ cell tumors. Important points to note about chemotherapy in this setting are that therapy is not held based on cytopenias, G-CSF is given with each cycle, and bleomycin is often held for treatments 11 and 12 (during cycle 4) for patients who will likely need to undergo resection especially of pulmonary metastatic disease. 
Another important management point about poor-risk germ cell tumor patients is that they often present quite sick with organ dysfunction that limit your ability to give full-dose standard of care chemotherapy. An example of a case where the patient presented with a markedly elevated bilirubin was offered, which precluded upfront etoposide therapy. In such cases, providers may consider a “mini” cycle (Honecker and Bokemeyer Annals Oncology 2010). This allows a temporizing therapy to be given and allows full-dose therapy to be given soon after. There is no standard regimen for this, but 20 mg/m2 cisplatin and/or etoposide 100 mg/m2 for 3-4 days is one possibility.
Next, Dr. Kollmansberger discussed the thrombosis risk in metastatic germ cell tumors. In a series of 1135 patients, 13% developed VTE either prior to, during or within 90 days of chemotherapy. Fortunately, only 1 patient died, but a significant portion of patients required hospitalization for management. The two statistically significant risk factors for VTE in this cohort was the presence of retroperitoneal lymphadenopathy > 3.5 cm (OR 1.81,95% CI 1.1-3, p = 0.02) and retroperitoneal primary (OR 3.3, 95% CI 1.01-10.83, p = 0.04). In light of this data, the presenter does two things: (1) tries to avoid indwelling venous access as this is a nidus for clot, and (2) considered VTE prophylaxis in all patients in the peri-chemotherapy period with the exception of patients with choriocarcinoma (especially with brain lesions) as these patients have high risk of spontaneous hemorrhage.
The issue of delayed marker normalization was covered as well. This is a significant problem, as patients who do not have marker normalization will either get more chemotherapy than recommended by guidelines or be started unnecessarily on salvage therapy. In a series of 41 patients with bHCG > 50,000 at presentation, 75% of patients had a persistently abnormal HCG 1 month after therapy. 48% of these patients remained with no evidence of disease and their HCG eventually normalized (Zon, Nichols et al JCO 1998), and 16% were cured after salvage therapy. The take home message is that so long as the tumor markers are dropping, one must be patient and wait. Salvage therapy is only indicated if the tumor marker starts to rise again. Additional cycles of the same chemotherapy are unlikely to be helpful but are likely to contribute excess toxicity.
Approximately 15-20% of poor risk germ cell tumor patients will have brain metastases. There are no specific guidelines for this, but a multimodality approach is essential. Importantly, the role or either surgery or radiation in patients who have brain metastases that go into remission with chemotherapy alone is unclear. Further study is required to better understand the optimal management of patients with brain metastases.
Finally, the resection of residual lesions > 1 cm after treatment is essential. The approach to residual lesions is shown in this slide. 
In summary, Dr. Kollmansberger provided a concise but broad summary of the approach and important issues surrounding management of patients with poor risk advanced testicular germ cell tumors. In addition to the points above, he discussed that treatment of these patients is a team sport best accomplished at a center with extensive expertise in the various disciplines required for the care of these patients (urology, medical oncology, radiation oncology).
Presented by: Christian K Kollmannsberger MD, Clinical Professor of Medical Oncology, BC Cancer-Vancouver Centre
Written by: Alok Tewari, MD, PhD, Medical Oncology Fellow at the Dana-Farber Cancer Institute, at the 2020 ASCO Genitourinary Cancers Symposium (#GU20), February 13th- February 15th, San Francisco, CA

