To do so, the authors performed an explorative, multicenter, retrospective study among124 men with mCRPC who were treated with 177Lu-PSMA and underwent PSMA-PET/CT at baseline (bPET) and at interim after two cycles of treatment (iPET). The authors assessed the primary endpoint of overall survival (OS).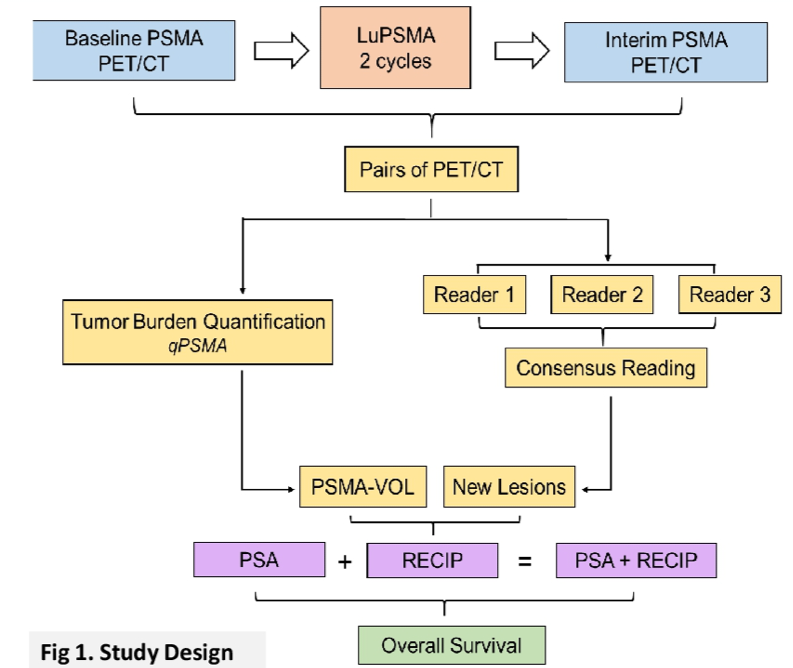
For each patient, three independent readers examined the baseline and interim PSMA-PET/CT images to identify the interval development of new lesions. qPSMA software was used for tumor lesion segmentation and total PSMA-positive tumor volume (PSMA-VOL) was calculated. The authors then assessed changes in the volume of PSMA-avid lesions on the interim PET relative to the baseline scan. After being tested separately for associations with overall survival, appearance of new lesions and changes in PSMA-VOL were combined to develop RECIP.
The median OS in this cohort was 13.5 months (95%CI, 11.6-15.4) from index. Compared to baseline PSMA-PET/CT, 73 (59%) patients had interval development of at least one new lesion on their interim PSMA-PET/CT. Development of new lesions between the baseline and interim PSMA-PET/CT was associated with an increased risk of death (hazard ratio [HR] for OS = 2.23; 95% CI, 1.51-3.28; P<.001).
Utilizing the available data, the authors then derived the Response Evaluation Criteria In PSMA-imaging (RECIP), defined as:
(1) partial response (PSMA-PR) as a decline ≥20% in PSMA-VOL and no appearance of new lesions;
(2) progressive disease (PSMA-PD) as an increase ≥20% in PSMA-VOL and appearance of new lesions;
(3) stable disease (PSMA-SD) was defined as any condition but not PSMA-PR or PSMA-PD.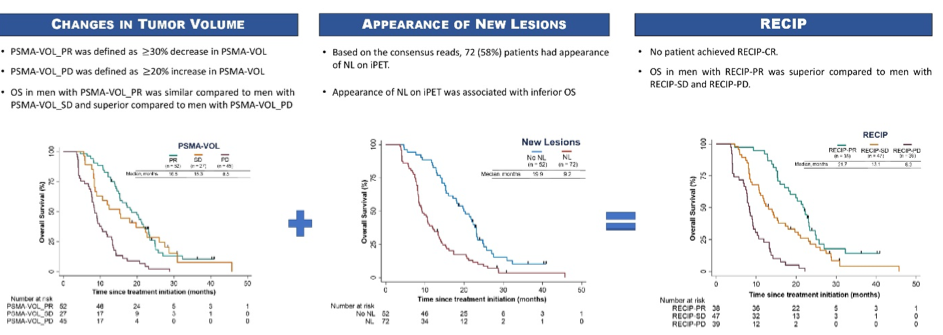
These RECIP strata were significantly associated with overall survival: with PSMA-PD (n = 41) had significantly worse survival compared to men with PSMA-SD (n = 47; HR 2.52; 95% CI, 1.61–3.93; P<.001) and those with PSMA-PR (n = 36; HR 4.16; 95% CI, 2.54–6.78; P<.001). Further, PSMA-SD was associated with significantly worse OS compared to PSMA-PR (HR 1.65; 95% CI, 1.02–2.65; P =.039).
The authors conclude that interim PSMA-PET/CT following two cycles of 177Lu-PSMA was prognostic for survival in men undergoing theranostic treatment. The proposed RECIP criteria require validation.
Presented by: Andrei Gafita, MD, Postdoctoral Scholar in the Ahmanson Translational Theranostics Division of the Department of Molecular and Medical Pharmacology at UCLA.
Written by: Christopher J.D. Wallis, MD, Ph.D., Urologic Oncology Fellow, Vanderbilt University Medical Center, Contact: @WallisCJD on Twitter at the 2021 American Society of Clinical Oncology (ASCO) Annual Meeting, Virtual Annual Meeting #ASCO21, June, 4-8, 2021

