Imaging in general decreases mortality (for example when used in cancer screening, such as mammography), decreases cost through accurate and prompt diagnosis (eliminating inappropriate surgery), and decreases length of an episode of care (accurate therapeutic monitoring). Imaging can significantly help in early detection, and aside from saving lives, it can significantly reduce costs. A permanent 10% reduction in cancer mortality rates would be worth 4.7$ trillion dollars to current and future Americans.
Dr. Pomper continued and described the small molecules used for detecting prostate cancer with PET. These include C- and F-labeled Choline, C-acetate, Fluciclovine, F-FDHT (androgen receptors), F-NaF, and Ga- and F-PSMA. PET-PSMA is emerging as the leading PET scan with the best sensitivity and specificity in PC diagnosis in its various states. There are several clinical spaces for imaging with PSMA. These include:
1. Selection of patients for active surveillance
2. Pre-surgical staging of patients at risk of occult metastatic disease
3. Direct therapy upon PSA recurrence following failed local therapy
4. Therapeutic monitoring of patients receiving focal therapy, radiation, or systemic therapy
Enhanced usage of PSMA scans in the future will enable to incorporate additional therapies for patients with rising PSA after radical prostatectomy. It will enable us to add to our armamentarium therapeutic options such as salvage pelvic lymph node dissection, and Stereotactic Ablative Radiotherapy (SABR) for oligometastasis.
There has been some development of using MRI imaging with incorporation of PSMA, demonstrating very interesting findings that are still being evaluated. Furthermore, the digitization of data will result in significant advancement in the field of imaging. This will allow image segmentation, extraction of radiomic features, and better classification/analysis of tumors (Figure 1).
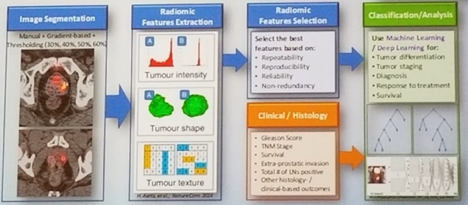
In the future, machine learning will enable computers to read all imaging and give better diagnostic results than any human can.
Dr. Pomper continued and discussed the usage of radiopharmaceutical therapy, such as Lutetium, which is being extensively researched with very promising results.
Lastly, Dr. Pomper discussed the integration of immunology with imaging, by using T cells to advance our imaging capabilities. It is possible to generate CD19 specific chimeric antigen receptor (CAR) T-cells co-expressing wild type or mutant PSMA, and assess function and detection with [18F]DCPyL. The next step will be to determine the sensitivity and specificity of CAR-T detection in vivo in localized and disseminated mouse tumor xenograft models.
In summary, there are several promising imaging and radiotheranostic agents for PC. Furthermore, radiopharmaceutical therapy is an expanding field with extensive research being currently conducted, demonstrating tremendous potential. Lastly, immunology can be incorporated with imaging, resulting in enhancement of our imaging capabilities.
Presented by: Martin Pomper, John Hopkins
Written by: Hanan Goldberg, MD, Urologic Oncology Fellow (SUO), University of Toronto, Princess Margaret Cancer Centre, Twitter:@GoldbergHanan at the 2018 ASCO Annual Meeting - June 1-5, 2018 – Chicago, IL USA


