Dr. Richard De Abreu Lourenco from the University of Technology Sydney started by discussing the cost-effectiveness of PSMA PET/CT. Based on the proPSMA study,1 colleagues from Australia showed that 68Ga-PSMA-11 PET/CT is more accurate for staging than conventional imaging. In this study, prospective data was collected to assess cost-effectiveness, including time and resource use for PSMA production, quantity produced per elution, and time taken per scan (PSMA PET/CT and CT/bone scan). The primary within-trial analysis included cost per additional accurate case control and secondary longer-term analysis included cost per quality-adjusted life year (QALY). From their analysis, PSMA PET/CT was more effective and less costly, showing a 27% greater accuracy than conventional imaging (95% confidence interval [CI] 23-31%, p<0.001). Longer-term, PSMA PET/CT was also shown to be cost-effective with $10,629 per QALY-gained, given that more men receive treatment that reflects their disease stage such that there is an improvement of resources used and patient outcomes. As follows is the analysis of production and imaging as well as scan time:
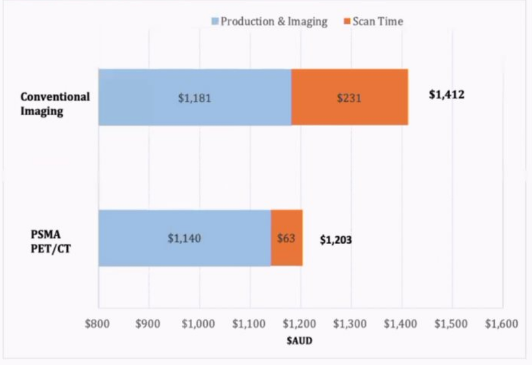
Next, Dr. Hui-Ming Lin from the Garvan Institute of Medical Research discussed a lipidomic analysis of circulating lipids across the natural history of prostate cancer and the identification of aberrant ceramide metabolism. Dr. Lin notes that there is epidemiological evidence of obesity leading to increased prostate cancer mortality, and there is molecular evidence that prostate cancer cells have increased lipid synthesis and lipolysis. Regarding circulating lipids, >700 species have been identified including sphingolipids, sterol lipids, prenols, fatty acyls, glycerolipids, and glycerol-phospholipids. The primary aim of their study was to assess the relationship between the plasma lipidome and clinical outcome in localized and metastatic prostate cancer. They found that lipidomic associated with worse clinical outcomes have higher levels of circulating ceramides among patients with localized, hormone-sensitive, and castration-resistant disease.
Third, Dr. Cynthia Hawks from Royal Perth Hospital in Perth presented her research “Analysis of the resource utilization, efficacy and the economic impact of a same-day prostate cancer assessment and/or diagnostic clinic at a public tertiary hospital in Australia.” This was a prospective study from August 2011 through November 2017 looking specifically at referrals and follow-up. They also did a retrospective analysis of resource utilization, as well as an analysis of outpatient clinic costs. In their cohort, there were 466 men that were deemed rural and 534 that were metro, including 568 referrals that were de novo and 452 that had previous urologic consults prior to attending the one-stop pathway clinic. There were 805 men that were scheduled subsequent follow-up in the one-stop pathway and 195 that were able to be discharged to their general practitioner. The one-stop clinic pathway ended up saving 575 clinic visits for rural men, which equated to 1.5 million kilometers saved in travel. In terms of per-patient costs, the one-stop pathway cost $284.34 compared to $832 for a regular clinic visit.
Next, Dr. Pravin Viswambaram from the UWA Medical School at the University of Western Australia in Perth discussed his research “A retrospective comparison of 18F-FDG-PET with CT in the detection of nodal and distant metastasis in urothelial carcinoma.” Dr. Viswambaram notes that according to the European Association of Urology (EAU) guidelines for muscle-invasive bladder cancer, there is currently insufficient data regarding the use of diffusion-weighted imaging (DWI) and FDG-PET/CT in muscle-invasive bladder cancer to allow for recommendations to be made. In their study, they retrospectively reviewed 90 patients, of which 78 had open radical cystectomy and pelvic lymph node dissection (21 had neoadjuvant chemotherapy). Both imaging modalities were compared to histology, including sensitivity, specificity, PPV, and NPV for detecting pelvic lymph nodes. As follows are the results of their study: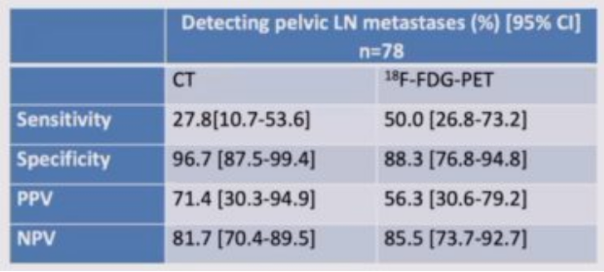
Ultimately, 18F-FDG-PET identified otherwise undetected metastatic disease in 4/85 patients. Dr. Viswambaram concluded that their data suggests that 18F-FDG-PET is more sensitive than CT for pelvic lymph node metastases and that 18F-FDG-PET significantly altered management in 4.7% of patients.
Finally, Dr. Deepti Pandey from the Centre for Biostatistics and Clinical Trials at the Peter MacCallum Cancer Centre presented research on “Central review of tumor assessment data: UNISoN study experience (ANZUP 1602)”. The aims of this study were:
- Sharing experience of central review of tumor assessment data of the UNISoN study
- Highlight common issues noted during a central review of the tumor assessment data
- Identify potential dimensions for improvements
The additional methods were as follows: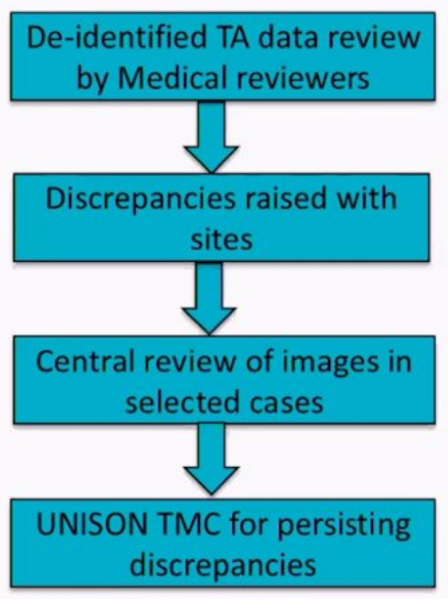
There were 85 total participants, 591 scans reviewed, and 1,035 total manually generated tumor assessment queries. When assessing RECIST queries by site, there was considerable variation. Furthermore, issues identified during the central review included (i) selection of target lesions at baseline (45%), (ii) documentation on RECIST worksheets and scan reports (12%), and (iii) measurement-related issues (4%). Additionally, incorrect identification of target lesions at baseline led to two patients being ineligible for activity assessment. Dr. Pandey concluded that central review of tumor assessment is complex but essential for accurate study outcomes. Second, there is considerable variability between sites in the conduct of RECIST, in that a percentage of sites used RECIST1.1/iRECIST accurately, but there was site variability in per patient RECIST queries were between 0 to 7.25. Finally, Dr. Pandey noted that adopting standardized processes, standardized RECIST worksheet, and site training in RECIST1.1/iRECIST to minimize variability and to minimize the issues are recommended for future trials.
Presented by: Shomik Sengupta, MD, MS, FRACS, Professor of Surgery, Eastern Health Clinical School, Monash University, Melbourne, Australia
Lisa Horvath, MBBS, FRACP, PhD, Director of the Department of Medical Oncology, Senior Staff Specialist, Conjoint Chair of Medical Oncology (Genitourinary Cancers), Chris O'Brien Lifehouse, Professor of Medicine, Central Clinical School University of Sydney, Darlinghurst, Australia
Written by: Zachary Klaassen, MD, MSc, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, Augusta, Georgia, Twitter: @zklaassen_md during the 2020 Australian and New Zealand Urogenital and Prostate Cancer Trials Group (ANZUP) Mini Annual Scientific Meeting (ASM), November 29 - 30, 2020
Reference:
1. Hofman, Michael S., Nathan Lawrentschuk, Roslyn J. Francis, Colin Tang, Ian Vela, Paul Thomas, Natalie Rutherford et al. "Prostate-specific membrane antigen PET-CT in patients with high-risk prostate cancer before curative-intent surgery or radiotherapy (proPSMA): a prospective, randomised, multi-centre study." The Lancet (2020).

