(UroToday.com) The 2022 American Urological Association (AUA) Annual Meeting included the Society of Urologic Oncology (SUO) session and a presentation by Andrew Hung discussing artificial intelligence in urologic oncology. Dr. Hung started his presentation by highlighting several important definitions. First, artificial intelligence is the ability of a machine to independently replicate intellectual processes typical of human cognition. Second, machine learning is algorithms that parse data, learn from that data, and then apply what they’ve learned to make informed decisions. Third, deep learning is a form of machine learning that is inspired by the structure of the human brain and is particularly effective in feature detection. Dr. Hung notes, that over the last several years, there has been a drastic increase in the number of artificial intelligence publications in the urology literature, with nearly 180 publications in 2021.
Artificial intelligence in urologic oncology is made up of several components. The first is diagnosis, which relies on radiomics, pathomics, genomics, and/or computer vision. Radiomics relies on sequential integration of:
- Imaging
- Segmentation
- Feature extraction
- Model training
- Validation
One example of radiomics is using artificial intelligence to assess imaging for prostate cancer. Prostate segmentation is performed with ultrasound or MRI, with studies showing radiomics performs better for detecting prostate cancer in PI-RADs 2 lesions (AUC >0.98 vs AUC 0.87). Additionally, radiomics may be used for assessing grade classification and extracapsular extension. With regards to pathomics, using software called the Paige Prostate, artificial intelligence leads to an AUC of >0.98, allowing pathologists to exclude 65%-75% of slides while retaining 100% of sensitivity:1
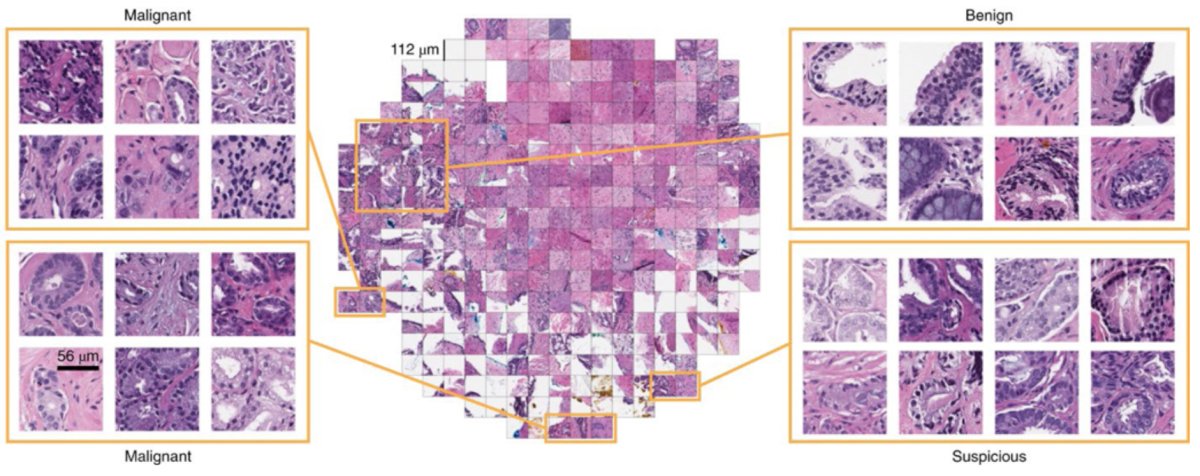
Dr. Hung noted that genomic analysis of plasma cell-free DNA also has allowed the development of genome derived tumor type prediction for informing clinical cancer care, and computer vision artificial intelligence, particularly in the field of bladder cancer, have improved tumor localization, intraoperative navigation, and surgical resection of bladder cancer:
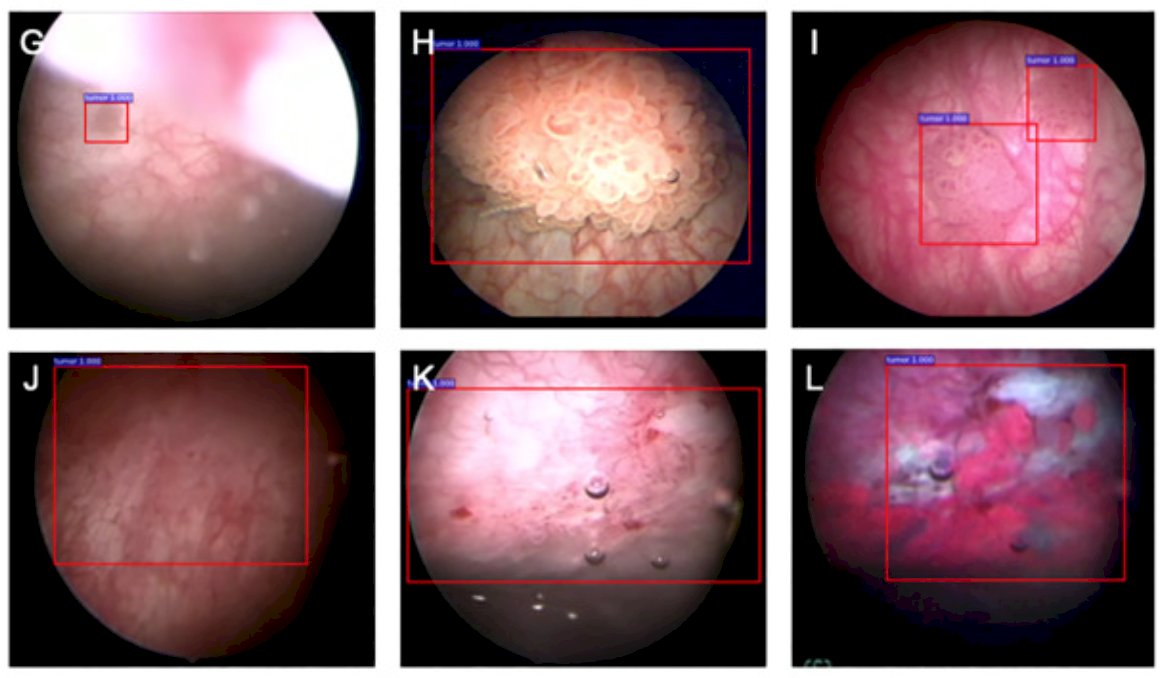
The second role of artificial intelligence in urologic oncology is aiding in prediction. Alessandrino et al.3 assessed the predictive ability of CT texture analysis for progression-free survival (PFS) in patients with metastatic urothelial carcinoma treated with PD-1/PD-L1 inhibitors. Among 31 included patients, 18 patients had PFS <12 months. Overall, 25 baseline CT and 29 first follow-up CT scans met the inclusion criteria. In patients with PFS <12 months, entropy and mean were higher on first follow-up CT (p=0.02 and p=0.005, respectively). A predictive model including mean and entropy on first follow-up CT yielded 95% sensitivity, 80% specificity, 90% positive predictive value, 89% negative predictive value, and 90% accuracy (AUC 0.963) to identify patients with PFS <12 months. As follows is a region of interest contouring and texture analysis evaluation on first follow-up CT, whereby histogram analysis of the two lesions show different shapes of the histogram and higher values of the lesion of patient A (PFS < 12 months) versus patient B (PFS > 12 months), reflecting higher mean and higher entropy:
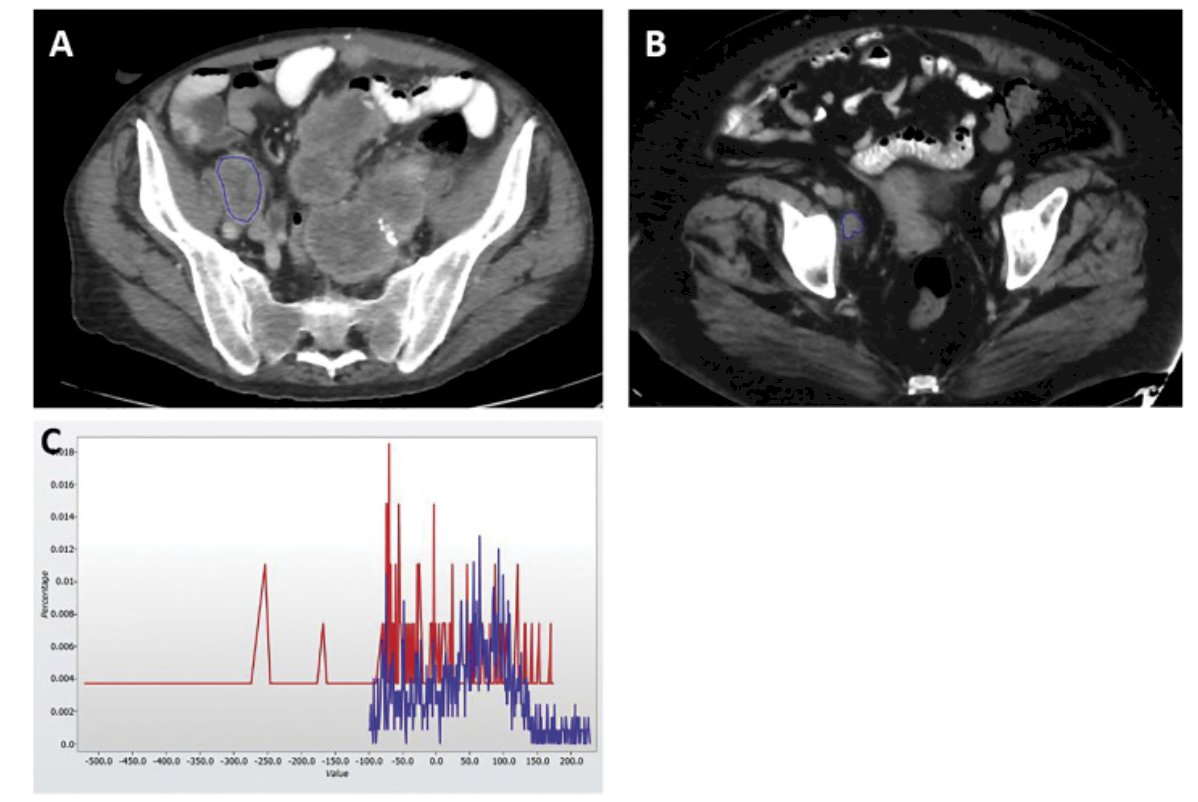
The third role of artificial intelligence in urologic oncology is aiding in surgical education. Dr. Hung’s group previously led a study assessing survival analysis using surgeon skill metrics and patient factors to predict urinary continence recovery after robotic assisted radical prostatectomy.4 The aim of this study was to evaluate the contributions of patient and treatment factors, surgeon efficiency metrics, and surgeon technical skill scores, especially for vesicourethral anastomosis, to models predicting urinary continence recovery following robot-assisted radical prostatectomy. Automated performance metrics (instrument kinematics and system events) and patient data were collected, and Robotic Anastomosis Competency Evaluation (RACE) scores during vesicourethral anastomosis were manually evaluated. The median RACE score was 28/30 (IQR 27-29), and among the individual datasets, technical skills (RACE) produced the best models (C index: Cox PH 0.695, deep learning survival analysis: 0.708). Among summary automated performance metrics, posterior/anterior vesicourethral anastomosis yielded superior model performance over other prostatectomy steps (C index 0.543-0.592). Among detailed automated performance metrics, metrics for needle driving yielded top-performing models (C index 0.614-0.655) over other suturing phases:

Dr. Hung concluded his presentation discussing artificial intelligence in urologic oncology with the following concluding statements:
- AI applications are helpful in urologic oncology with regards to diagnosis, prognosis, and surgical education
- Model performance is robust
- However, we must be careful with regards to reproducibility and replicability
Presented by: Andrew Hung, MD, AI Center at USC Urology, University of Southern California, Los Angeles, CA
Written by: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, @zklaassen_md on Twitter during the 2022 American Urological Association (AUA) Annual Meeting, New Orleans, LA, Fri, May 13 – Mon, May 16, 2022.
References:
- Campanella G, Hanna MG, Geneslaw L, et al. Clinical-grade computational pathology using weakly supervised deep learning on whole slide images. Nat Med. 2019 Aug;25(8):1301-1309.
- Shkolyar E, Jia X, Chang TC, et al. Augmented bladder tumor detection using deep learning. Eur Urol. 2019 Dec;76(6):714-718.
- Alessandrino F, Gujrathi R, Nassar AH, et al. Predictive role of computed tomography texture analysis in patients with metastatic urothelial cancer treated with programmed death-1 and programmed death-ligand 1 inhibitors. Eur Urol Oncol. 2020 Oct;3(5):680-686.
- Trinh L, Mingo S, Vanstrum EB, et al. Survival analysis using surgeon skill metrics and patient factors to predict urinary continence recovery after robotic assisted radical prostatectomy. Eur Urol Focus 2021 Apr 12;S2405-4569(21)00107-3.

