In this study, 208 men with a median PSA of 0.8 underwent PyL PET/CT. The inclusion criteria and exclusion criteria are shown below. The PSA had to be ≥0.2 ng/mL in the post-RP patient and ≥2.0 ng/mL in the post-RT or cryotherapy patient.
The primary endpoint of the study was the correct localization rate (CLR), which is defined as the percentage of patients who had at least one lesion on PET which correlated with either pathology, correlative imaging, or PSA response.
The study design is shown below. There were three blinded independent 18F-DCFPyL-PET/CT readers and of note, a separate “truth panel”, which was guided on the above composite standard of truth to determine the CLR.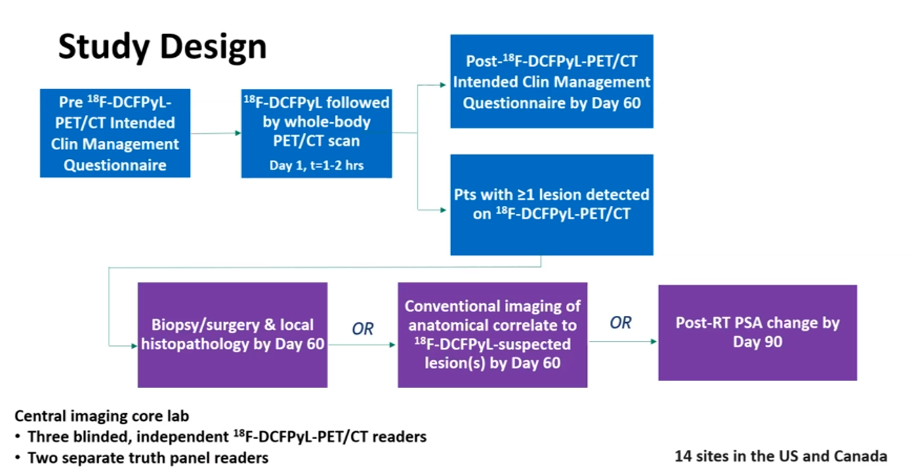
In terms of baseline characteristics, the median age was 68, with a median of 5.9 years from the time of original prostate cancer diagnosis. About half the patients had received radical prostatectomy only, 35% received RP and RT, and 15% received only RT. Most (73%) had a Gleason <8 and 34% of patients had a PSA <0.5.
In terms of detecting disease with 18F-DCFPyL-PET/CT, 59-65% of patients had positive imaging findings by PET. Of note, all of these patients had no evidence of disease with standard of care imaging. Of the positive findings, the majority of patients had clinical localization.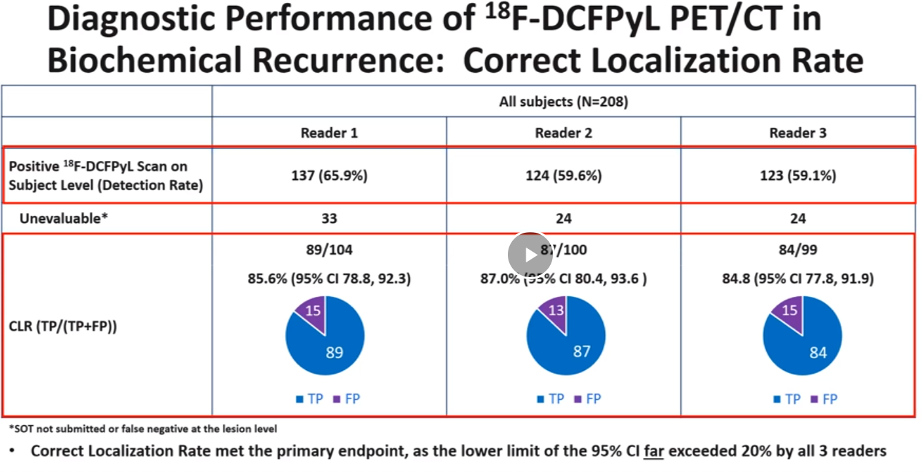
The CLR rate was 85-87% amongst the three PyL PET/CT readers. CLR was highest amongst patients with a PSA >5 (96%) but remained high even in patients with a PSA <0.5 (73%). For patients with a PSA >5, PyL PET detected disease in 96% of patients and up to 36% of patients with a PSA <0.5.

131/205 (64%) of patients had a change in intended management after PyL PET/CT. 21% of patients had a change in goal of treatment from non-curative intent to curative intent. The most common change was changing from salvage local therapy to systemic therapy (58/131). Other changes included changing from systemic therapy to salvage therapy (43/131), changing from treatment to observation (9/131). PyL was well tolerated and the most common AE was headache (n=4, 1.9%).
I think there is little doubt that PSMA imaging modalities are more sensitive than current standard of care imaging modalities. Data presented in this abstract on 18F-DCFPyL-PET/CT shows that DCFPyL-PET can detect disease in the majority of patients with a PSA>5 and even in a third of patients with a PSA<0.5 More importantly, this detection leads to a change in management for the majority of patients, some even changing treatment intent from palliative to curative. Once PSMA PET is approved in the United States, I think multidisciplinary tumor boards will have an even larger role to play as we find more early recurrences of disease.
Presented by: Michael J. Morris, MD., is the Clinical Director, Genitourinary Medical Oncology Service & Prostate Cancer Section Head, Division of Solid Tumor Oncology, Memorial Sloan Kettering Cancer Center, New York, NY.
Written by: Jason Zhu, MD. Medical Oncologist, Division of Genitourinary Cancers, Levine Cancer Institute, Twitter: @TheRealJasonZhu at the 2020 ASCO Annual Meeting, Virtual Scientific Program #ASCO20, May 29- 31, 2020
Reference:
1. Rowe SP, Macura KJ, Mena E, et al. PSMA-based [18 F] DCFPyL PET/CT is superior to conventional imaging for lesion detection in patients with metastatic prostate cancer. Molecular imaging and biology 2016;18:411-9.
Related Content:
Video: CONDOR: Study of 18F-DCFPyL PET/CT Imaging in Patients with Suspected Recurrence of Prostate Cancer - Michael J. Morris
Clinical Trial Information: NCT03739684: A Phase 3, Multi-Center, Open-Label Study to Assess the Diagnostic Performance and Clinical Impact of 18F-DCFPyL PET/CT Imaging Results in Men With Suspected Recurrence of Prostate Cancer

