Eight centers across Canada (Renal Cell Carcinoma Consortium of Canada) prospectively enrolled patients with an incidental SRM diagnosis for initial AS in a Phase II trial between August 2004 to December 2015 and was pooled with the prospectively maintained Princess Margaret Cancer Centre AS cohort for the same period. All patients received renal mass biopsy for pathologic diagnosis and were followed with serial imaging using CT, MRI, and ultrasound. Tumor progression was defined by (a) large size (sustained maximum diameter >4 cm in at least two measurements within 15 months) and/or (b) rapid growth (doubling of tumor volume within 1 year).
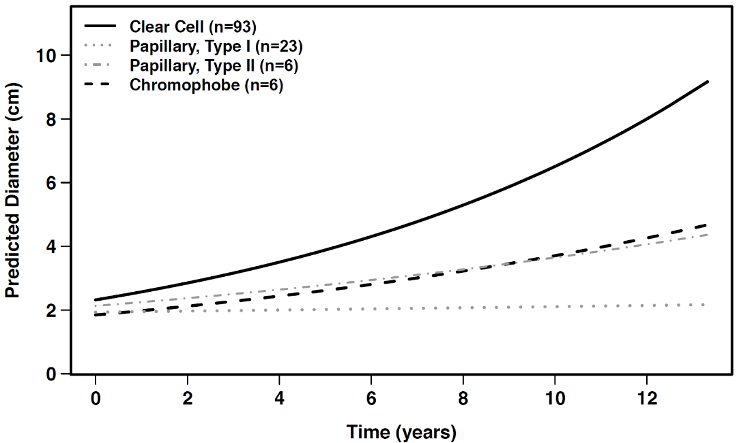
Overall, the average growth rate in maximal tumor diameter was 8%/yr (0.17 cm/yr in the first year, 0.19 cm/yr over the first three years, and 0.28 cm/yr predicted growth over 12 years). Notably, however, we were able to observe significant differences between and within histologic subtypes (see Figure). For the most frequent subtype, clear cell RCC, these lesions displayed substantial heterogeneity: most demonstrated stable or little growth for years (average 0.28 cm/yr), while a small subset (15%) exhibited growth ≥0.5 cm/yr. Strikingly, all metastases had clear cell histology. In contrast, papillary type 1 RCC lesions remained stable throughout observation, exhibiting near-zero growth (average 0.017 cm/yr) and had no documented metastases.
Furthermore, given the long term follow-up of our study, we observed that some SRMs demonstrated little growth initially, but accelerated at a later date. This emphasized the need for continued AS despite an initial suggestion of indolence and may reflect ongoing genomic/biological evolution in the tumor and host. Overall, the probability of progression at five years was 54% (95% confidence interval: 43-64%).
Equally important, disparities in tumor measurement from image to image (e.g. growing/progressing tumors that were stable in subsequent observations) raised important considerations of inter- and intra-observer variability, and stochasticity in growth. By reviewing the imaging (and its growth trajectory) and re-imaging (sometimes after a two- to three-month interval), apparent progression often did not occur, suggesting that clinical decisions should be delayed until sustained growth is confirmed through axial imaging.
This is the largest biopsy-proven cohort of sporadic SRM (RCC) followed by AS. Substantial heterogeneity within and between histologic subtypes was observed, with significant differences across growth and progression rates. Pathology from renal mass biopsy is valuable in counseling patients and personalizing the management of SRMs until non-tissue-based markers are developed.
Written by: Douglas C. Cheung, MD, MBA, MSc(c), and Antonio Finelli, MD, MSc, FRCSC, Division of Urology, Department of Surgery, Princess Margaret Cancer Centre and the University Health Network, University of Toronto, Toronto, Ontario, Canada
Read the Abstract

