Prostate cancer is the most common malignancy among US men, with an estimated annual incidence of 180,890, accounting for one in five new cancer cases in men.1 The second-most common cause of cancer death in US men, prostate cancer is expected to claim the lives of 26,120 men in this country in 2016.1 For men with castration-resistant prostate cancer (CRPC), median survival ranges from nine to 34 months, depending upon numerous factors, including but not limited to, the presence of metastases, the location and volume of metastases, the presence of co-morbidities, the degree of acknowledged and interrogated symptomatology, etc.2
Whereas metastases may be widely disseminated in advanced prostate cancer,3 the disease predominantly affects the bone compartment. Indeed, prostate cancer has an affinity to metastasize to bone, which provides a matrix rich in factors that stimulate the growth of tumor cells and promotes a vicious cycle of metastases and bone pathology.4 In the early stages of advanced prostate cancer, malignant cells detached from the primary tumor migrate locally, invade blood or lymphatic vessels, and may disperse throughout the body.4-6 Once in the bloodstream, metastatic cells (i.e., the “seeds”) have a decreased survival outside of the primary tumor (i.e., the “homeland”) due to the defense of the immune system and thus require the appropriate “soil” for implantation.5 Consequently, the “seeds” may preferentially migrate to bone (i.e., the “hostland,” as illustrated in Figure 1).4-6
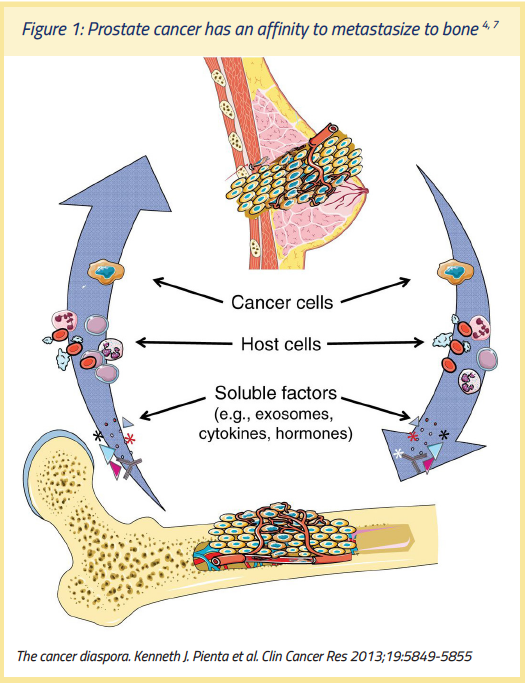
Approximately 90% of men with advanced prostate cancer will develop bone metastases,8 and approximately 50% of men who convert from androgen sensitive state to nonmetastatic (M0) CRPC will develop bone metastases within two years.9 Metastases preferentially arise in bones of the spine, pelvis, and ribs, where red marrow is most abundant,5,6 as well as arise in the skull and long bones of the extremities.5,6,8
Variable Migratory Pathways of Bone Metastases
Most men with clinically localized prostate cancer who develop bone metastases will do so many years after the primary tumor has been removed, suggesting a delay of time between the initial interventional therapy and the initial indication of biochemical recurrence/PSA relapse, thus suggesting micrometastases.3 Metastatic prostate cancer cells are thought to remain dormant in the bone marrow for several years before transforming into a proliferative phenotype that drives metastatic progression.3 Whole genome sequencing has illuminated the genomic evolution of CRPC, from initial tumorigenesis, through acquisition of metastatic potential, to the development of castration resistance.10 Results from genomic studies support the theory of progression from dormancy to proliferation, whereby tumor cells sharing a common heritage travel from one site to another while retaining their genetic imprint.10 In those studies, monoclonal and polyclonal metastatic tumor cells have been shown to preferentially and frequently migrate between distant sites rather than as separate waves from the primary tumor (Figure 2).10 Those observations support the “seed and soil” hypothesis, which holds that metastatic potential is not always a variable solely of the primary tumor, but may be acquired as a delayed event or occur at distant sites of metastases.10
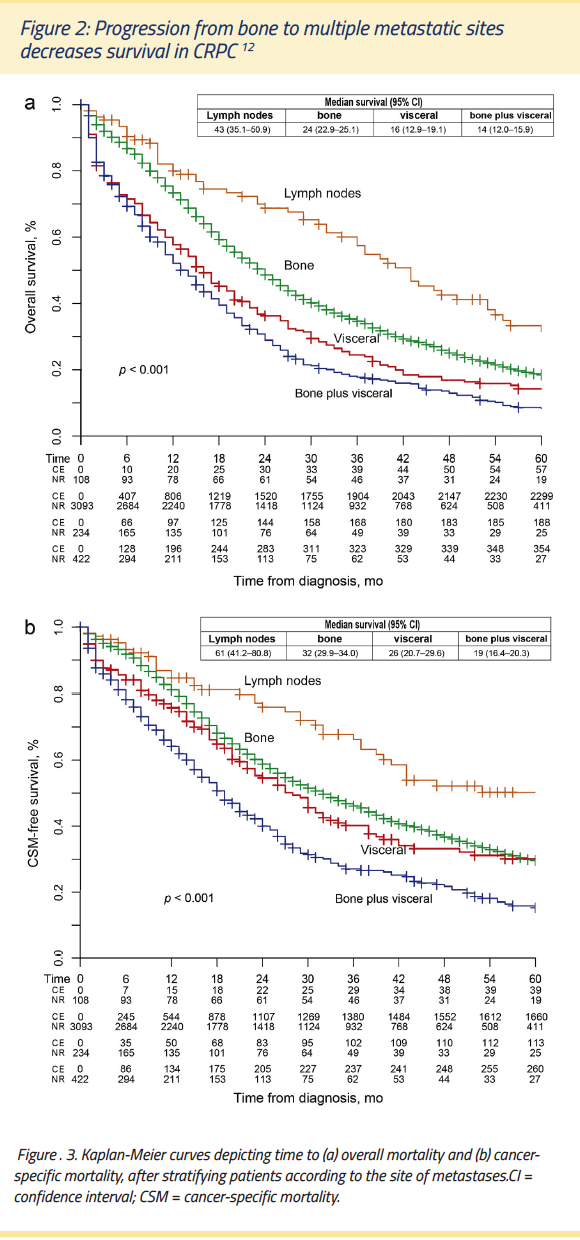
Bone metastases are associated with higher mortality
Bone metastatic disease indicates a poor prognosis in men with prostate cancer, and correlates with significant mortality. In a Danish cohort study of 23,087 incident patients with prostate cancer, of the 22,404 men without bone metastases at diagnosis, 56% were alive at five years (95% confidence interval [CI]: 54.9-56.7), compared to 3% of the 2,578 men who were diagnosed with bone metastases (95% CI: 2.2-3.4).11 The site of metastases may have profound prognostic implications. In an analysis of 3,857 men from the SEER database who presented with metastatic prostate cancer between 1991 and 2009, progression from bone to multiple metastatic sites was associated with increasing mortality (Figure 3).12 In that analysis, the site of metastases, after adjusting for confounders, emerged as an independent prognostic factor.12 Notably, patients who had bone metastases alone had a 1.5-fold higher probability of death compared to men with lymph node involvement only (P=0.02).12 Additionally, men with bone plus visceral metastases had a 1.3-fold higher probability of dying versus men who only had bone metastases.12 (See Figure 3)

Impact of Bone Metastases on Quality of Life
Mortality considerations aside, bone metastases can also significantly impact quality of life as a consequence of their associated effects [13]. Whereas fatigue is the most stressful symptom cited by men with mCRPC,14 patients with bone metastases may also experience pain as well as activity limiting lifestyle, discomfort,15,16 extremity weakness,15 neurological impairment,17 dyspnea,15 impaired mobility,15 loss of bladder and bowel function,15 mild sensory loss or numbness,15 loss of appetite,18 sleep disturbance.16 Notably, a 2015 US survey commissioned by Bayer HealthCare suggests that nearly seven out of 10 (68%) of men with advanced prostate cancer ignore or under-report their symptoms to their healthcare providers.19 The most commonly reported symptoms by survey participants included:19
- • Fatigue: 85%
- • All over body pain or aches: 55%
- • Numbness or weakness: 55%
- • Difficulty sleeping as a result of pain: 42%
- • Difficulty performing normal activities: 40%
- • Anxiety or distress as a result of pain: 40%
- • Vomiting: 25%18
- • Loss of appetite18
Economic Burden of Bone Metastases
Bone metastatic disease also carries a significant economic burden to the US healthcare system, particularly when patients experience skeletal-related events (SREs). A model drawn from the SEER database estimated a lifetime medical care cost of $140,501 (95% CI: $140,252-$140,780) per person for men ≥65 years old who were diagnosed with prostate cancer from 1991 to 2002 [20]. In a matched case-control study of health care utilization costs among of 1,131 elderly patients with stage IV metastatic (M1) prostate cancer and SREs, those undergoing spinal cord compression with concurrent surgery incurred an average cost of $82,868 (95% CI: $67,472-$98,264). The next most expensive SRE groups were those who had bone surgery only ($37,496; 95% CI: $29,684-$45,308), pathological fracture with concurrent surgery ($34,169; 95% CI: $25,837-$42,501), spinal cord compression only ($25,793; 95% CI: 20,933-$30,653), and pathological fracture only ($14,649; 95% CI: 6,537-$22,761) [21].
Is Earlier Detection of Bone Metastatic Disease of Value?
The significant prognostic and economic implications of bone metastases in prostate cancer have prompted researchers to investigate whether earlier detection of bone metastatic disease is of value. For men with stage M0 castrate-resistant disease (i.e., prostate cancer that has not spread beyond nearby lymph nodes), the Prostate Cancer Radiographic Assessments for Detection of Advanced Recurrence (RADAR) group recommends a first imaging scan when the prostate-specific antigen (PSA) level is at least 2 ng/mL. If the previous scan is negative, the RADAR group recommends a second scan when PSA equals 5 ng/mL, and repeat scanning at every doubling of PSA level thereafter, based on PSA testing every three months. The group cautions against overimaging in practice, and therefore does not recommend scanning newly diagnosed low-risk patients and most intermediate-risk patients. In terms of cost-effectiveness, the RADAR group recommends conventional bone scintigraphy using technetium 99 (99mTc) and abdomen/pelvis/chest computed tomography (CT) as imaging modalities for initial testing.22 Other novel imaging modalities are available (Table 1), and the RADAR group suggests using plain radiography, magnetic resonance imaging (MRI), and 18F-sodium fluoride (NaF) with positron emission tomography (PET) or CT (particularly for detection of osseous metastases); these tests should be conducted at the physician’s discretion when necessary, as they may be needed to clarify equivocal lesions.22,23 (see Table 1)
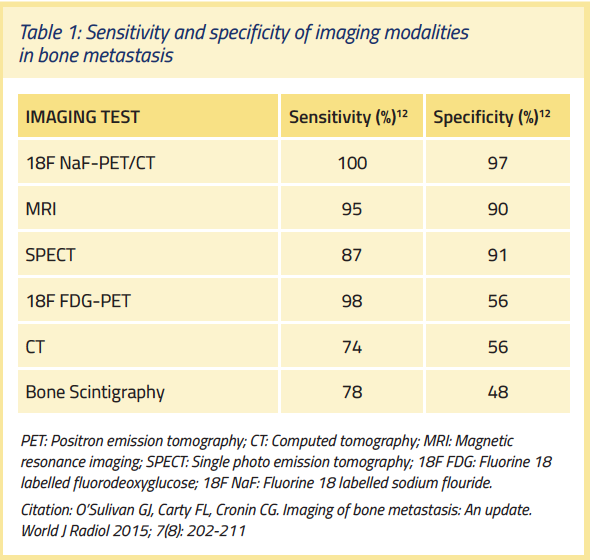
As shown in Table 1, PET/CT scans using tracers, such as 18F-NaF, offer sensitivity and specificity that are superior to bone scintigraphy and are frequently incorporated into guidelines.22
Use of ALP and PSA to Predict Risk of Bone Metastatic Disease
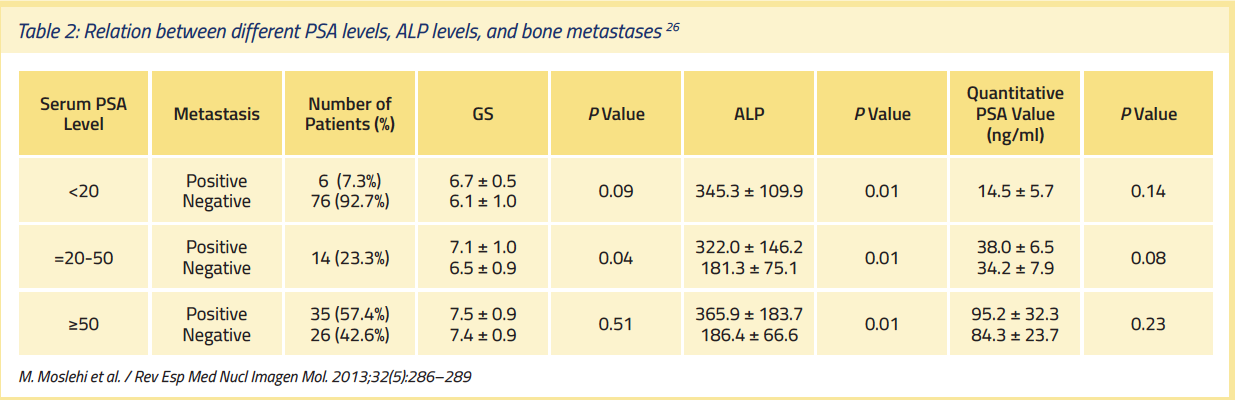
Bone alkaline phosphatase (ALP), when used in combination with PSA, can be an effective independent marker for predicting the risk of developing bone metastatic disease, as reported in a study of 203 men with asymptomatic, treatment-naïve prostate cancer (Table 2) [26]. In multivariate analyses from this study, the combination of elevated ALP and PSA (in which patients with either elevated PSA [>20 ng/mL] OR elevated ALP were categorized as positive) exhibited the best screening value for detecting bone metastases, with a sensitivity of 98.2% and a specificity of 48.6%.26 ALP and PSA, along with the RADAR group recommendations, may thus be used to detect the onset of bone metastases in asymptomatic individuals.22,26 (See Table 2)
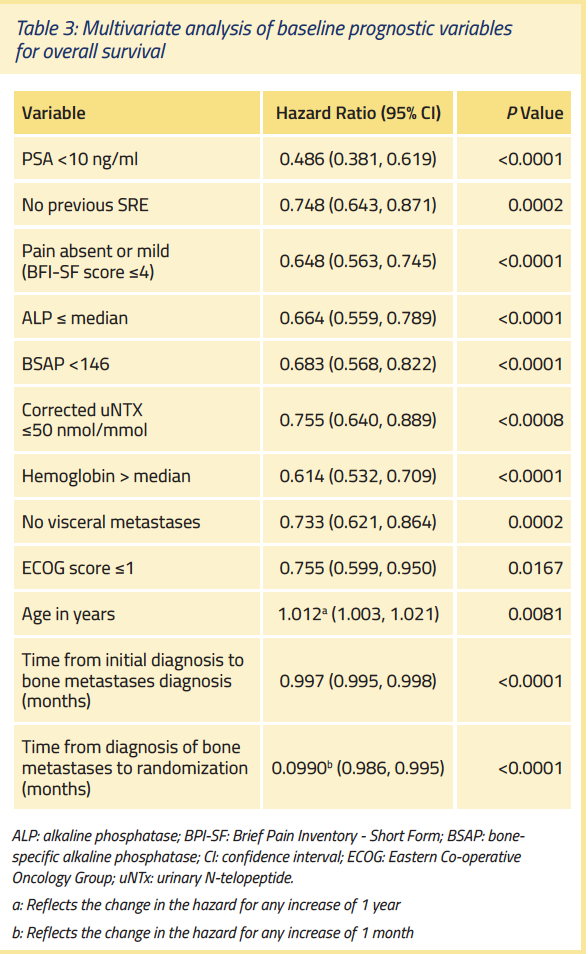
Monitor Key Bone-related Parameters as Prognostic Factors for Overall Survival
Several bone-related parameters, including those listed in Table 3, have been validated as individual prognostic variables for overall survival in patients with mCRPC.27 In an analysis of the prognostic value of multiple bone-specific parameters in 1,901 patients enrolled in an international, multicenter, randomized, double-blind phase 3 trial, the following factors were significantly associated with longer survival.27 (See Table 3)
Change Therapeutic Approach as Disease Progresses
The presence or absence of metastases is one of the most important factors affecting the clinical approach to managing prostate cancer.22 The site/volume of metastatic prostate cancer may evolve over time for individual patients, a process which has important clinical implications.22 When cancer spreads to the bone, the clinician should reconsider the therapeutic approach as one that shifts from treating not only the primary prostate cancer but also for treating the bone metastases, as clinical therapeutic interventions in bone metastatic disease can impact outcomes.3,10 Similarly, when cancer spreads from the bone to the viscera, the clinical approach should focus on treating visceral metastases as well.28
Summary
In devising a treatment plan for prostate cancer , the clinician should consider the implications of how metastatic disease site, location, and tumor burden may evolve over time.10,22 Advanced prostate cancer is notable for predominantly residing in the bones.4-6 As the great majority of men with advanced prostate cancer will develop bone metastases, the presence of which indicates a poor prognosis, is also associated increased mortality and morbidity.8,12 Men with bone metastases typically experience multiple and varied symptoms that may negatively impact quality of life.13-18
Early detection of bone metastases can therefore inform clinical decision-making and may be interrogated by the evaluation of laboratory, clinical, and patient and caregiver symptom assessment. The RADAR group recommends specific strategies for enabling early identification of metastases in patients with prostate cancer.22 Additionally, ALP plus PSA can be an effective marker for predicting risk of bone metastatic disease.26 Finally, because prostate cancer is associated with increased mortality as the disease migrates from localized to multiple metastatic sites,12 it is important for clinicians to adjust their clinical approach as the disease progresses.22
Written by: Neal Shore, MD, FACS
References
1. Siegel, R.L., K.D. Miller, and A. Jemal, Cancer statistics, 2016. CA: a cancer journal for clinicians, 2016. 66(1): p. 7-30.
2. Kirby, M., C. Hirst, and E.D. Crawford, Characterising the castration-resistant prostate cancer population: a systematic review. International journal of clinical practice, 2011. 65(11): p. 1180-92.
3. van der Toom, E.E., J.E. Verdone, and K.J. Pienta, Disseminated tumor cells and dormancy in prostate cancer metastasis. Current opinion in biotechnology, 2016. 40: p. 9-15.
4. Yin, J.J., C.B. Pollock, and K. Kelly, Mechanisms of cancer metastasis to the bone. Cell research, 2005. 15(1): p. 57-62.
5. Bagi, C.M., Skeletal implications of prostate cancer. Journal of musculoskeletal & neuronal interactions, 2003. 3(2): p. 112-7.
6. Kingsley, L.A., et al., Molecular biology of bone metastasis. Molecular cancer therapeutics, 2007. 6(10): p. 2609-17.
7. Pienta, K.J., et al., The cancer diaspora: Metastasis beyond the seed and soil hypothesis. Clinical cancer research : an official journal of the American Association for Cancer Research, 2013. 19(21): p. 5849-55.
8. Bubendorf, L., et al., Metastatic patterns of prostate cancer: an autopsy study of 1,589 patients. Human pathology, 2000. 31(5): p. 578-83.
9. Smith, M.R., et al., Disease and host characteristics as predictors of time to first bone metastasis and death in men with progressive castration-resistant nonmetastatic prostate cancer. Cancer, 2011. 117(10): p. 2077-85.
10. Gundem, G., et al., The evolutionary history of lethal metastatic prostate cancer. Nature, 2015. 520(7547): p. 353-7.
11. Norgaard, M., et al., Skeletal related events, bone metastasis and survival of prostate cancer: a population based cohort study in Denmark (1999 to 2007). The Journal of urology, 2010. 184(1): p. 162-7.
12. Gandaglia, G., et al., Impact of the Site of Metastases on Survival in Patients with Metastatic Prostate Cancer. European urology, 2015. 68(2): p. 325-34.
13. Resnick, M.J. and D.F. Penson, Quality of life with advanced metastatic prostate cancer. The Urologic clinics of North America, 2012. 39(4): p. 505-15.
14. Colloca, G., et al., Incidence and Correlates of Fatigue in Metastatic Castration-Resistant Prostate Cancer: A Systematic Review. Clinical genitourinary cancer, 2016. 14(1): p. 5-11.
15. Farrell, C., Bone metastases: assessment, management and treatment options. British journal of nursing, 2013. 22(10): p. S4, S6, S8-11.
16. Autio, K.A., et al., Prevalence of pain and analgesic use in men with metastatic prostate cancer using a patient-reported outcome measure. Journal of oncology practice / American Society of Clinical Oncology, 2013. 9(5): p. 223-9.
17. Selvaggi, G. and G.V. Scagliotti, Management of bone metastases in cancer: a review. Critical reviews in oncology/hematology, 2005. 56(3): p. 365-78.
18. Hamilton, W., et al., Clinical features of metastatic cancer in primary care: a case-control study using medical records. The British journal of general practice : the journal of the Royal College of General Practitioners, 2015. 65(637): p. e516-22.
19. MenWhoSpeakUp Prostate Cancer Symptoms Survey -- US Results. 2015 May 27, 2016]; Available from: https://www.menwhospeakup.com/prostate-cancer-survey/.
20. Stokes, M.E., et al., Lifetime economic burden of prostate cancer. BMC health services research, 2011. 11: p. 349.
21. Jayasekera, J., et al., The economic burden of skeletal-related events among elderly men with metastatic prostate cancer. PharmacoEconomics, 2014. 32(2): p. 173-91.
22. Crawford, E.D., et al., Challenges and recommendations for early identification of metastatic disease in prostate cancer. Urology, 2014. 83(3): p. 664-9.
23. Koo, P.J. and E. David Crawford, (1)(8)F-NaF PET/CT and (1)(1)C-Choline PET/CT for the initial detection of metastatic disease in prostate cancer: overview and potential utilization. Oncology, 2014. 28(12): p. 1057-62, 1064-5.
24. O'Sullivan, G.J., F.L. Carty, and C.G. Cronin, Imaging of bone metastasis: An update. World journal of radiology, 2015. 7(8): p. 202-11.
25. Mhawech-Fauceglia, P., et al., Prostate-specific membrane antigen (PSMA) protein expression in normal and neoplastic tissues and its sensitivity and specificity in prostate adenocarcinoma: an immunohistochemical study using mutiple tumour tissue microarray technique. Histopathology, 2007. 50(4): p. 472-83.
26. Moslehi, M., et al., Predictors of bone metastasis in pre-treatment staging of asymptomatic treatment-naive patients with prostate cancer. Revista espanola de medicina nuclear e imagen molecular, 2013. 32(5): p. 286-9.
27. Fizazi, K., et al., Bone-related Parameters are the Main Prognostic Factors for Overall Survival in Men with Bone Metastases from Castration-resistant Prostate Cancer. European urology, 2015. 68(1): p. 42-50.
28. Halabi, S., et al., Meta-Analysis Evaluating the Impact of Site of Metastasis on Overall Survival in Men With Castration-Resistant Prostate Cancer. Journal of clinical oncology : official journal of the American Society of Clinical Oncology, 2016. 34(14): p. 1652-9.

