(UroToday.com) As part of the Master Class session on genomic testing and recurrence in prostate cancer at the 2020 Société Internationale d'Urologie (SIU) virtual annual meeting, Dr. Shusuke Akamatsu discussed liquid biopsy in prostate cancer.
Dr. Akamatsu started by outlining the landscape of advanced prostate cancer, starting with Dr. Huggins innovating surgical castration in 1941 through olaparib being approved in 2020:
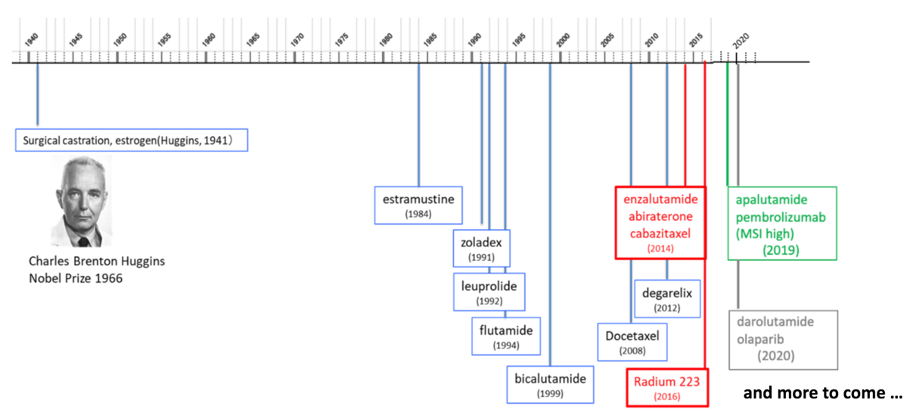
However, there are too many drugs for a trial and error approach, and as such, there is a need to optimize treatment sequences based on biomarkers. Entering the era of precision medicine, we ideally want genomic analysis each time a new treatment is initiated, given the change in the dynamic DNA alteration during the course of the disease. However, there is limitations of tissue-based genomic medicine in castration-resistant prostate cancer (CRPC), which predominantly metastasizes to the bone. In contrast, liquid biopsy offers a non-invasive method that allows repeat testing. This includes, most commonly, circulating tumor cells (CTCs) and cell-free DNA (cfDNA):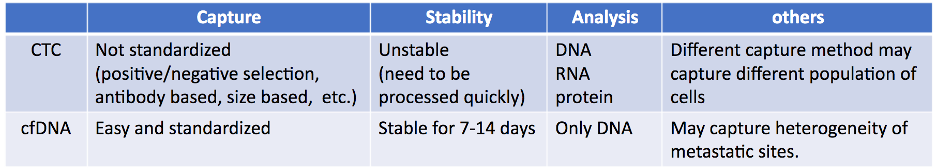
Circulating tumor cell number (enumeration) as a response measure has been assessed in patients with metastatic castration-resistant prostate cancer (mCRPC). Heller et al. used week 13 CTC and PSA response end points in five prospective randomized phase III trials that enrolled a total of 6,081 patients from COU-AA-301, AFFIRM, ELM-PC-5, ELM-PC-4, and COMET-1.1 Among eight response end points, CTC0 (baseline CTC ≥1 0 CTC at 13 weeks) and CTC conversion (baseline CTC ≥5 CTC ≤4 at 13 weeks) had the highest weighted c-indices. For CTC0, the mean was 0.81 (SD 0.04), for CTC conversion, 0.79 (SD 0.03), for 30% decrease in CTC count 0.72 (SD 0.06), for 50% decrease in CTC count 0.72 (SD 0.06), for 70% decrease in CTC count 0.73 (SD 0.05), for 30% decrease in PSA level 0.71 (SD 0.03), for 50% decrease in PSA level 0.72 (SD 0.06), and for 70% decrease in PSA level 0.74 (SD 0.05).
AR-V7 in CTCs is another candidate biomarker of interest. AR-V7 detection by both RT-PCR (Adna test) and Epic AR-V7 assay (IHC staining) were associated with shorter progression-free survival (PFS) and overall survival (OS) in patients treated with enzalutamide or abiraterone after adjusting for CTC number and clinical factors in a prospective trial.2 But generally, data is conflicting and robust clinical assessment of the assays is required before routine clinical use.
cfDNA is plasma circulating free DNA that is released into the bloodstream from necrotic or apoptotic cells. However, identifying tumor-derived cfDNA (ctDNA) from the entire pool of cfDNA (often less than 10%, sometimes less than 1%) is the equivalent of finding a needle in a haystack. There are two widespread methods for ctDNA detection:
- Digital PCR: has a sensitivity of ~0.1-0.01%, with the need to analyze each locus separately
- Target gene capture and next-generation sequencing: has a sensitivity of ~1-2%, whereby 30-40% of mCRPC patients have no detectable ctDNA with a VAF cutoff of 2%. Additional sensitivity measures, such as molecular barcoding is necessary to accurately detect variants with VAF <1%.
Androgen receptor aberrations in cfDNA have also been of great interest. As follows are summary tables of two studies from Vancouver and the Johns Hopkins group in this disease space: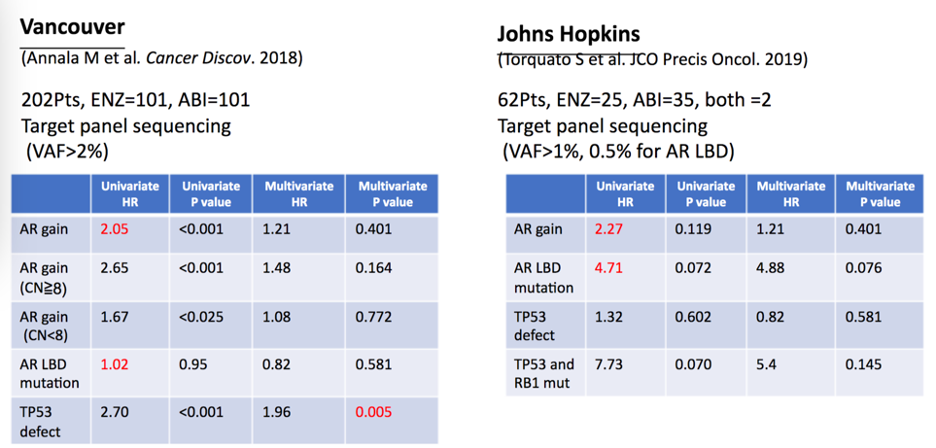
These early results suggest that androgen receptor (AR) amplification in cfDNA does not preclude the use of androgen receptor-axis-targeted therapies, and androgen receptor ligand-binding domain mutations if analyzed to below 1%, may have predictive value. Target sequencing of cfDNA is also feasible, as well as cfDNA analysis as companion diagnostics. A recent study used cfDNA to detect BRCA2 somatic mutations and also reversion mutation at the time of PARP inhibitor recurrence.3
Timely, non-invasive detection of somatic mutations with cfDNA is a powerful tool to push forward precision medicine in prostate cancer. However, Dr. Akamatsu notes that there are several challenges:
- How sensitive does the assay have to be? VAF cut-off of 2%? 1%? 0.1%? Less?
- Is repeat testing with next-generation sequencing really clinically applicable?
- Can more simplified (and cheaper) tests with digital PCR be developed for each clinical context?
Dr. Akamatsu concluded his presentation with the following summary points:
- To proceed with precision medicine in CRPC, which predominantly metastasizes to the bone, timely evaluation of somatic mutations by liquid biopsy is necessary
- CTC and cfDNA are powerful tools to capture dynamic genomic heterogeneity of CRPC, however, their utility needs to be rigorously tested in large prospective trials before broader clinical application
- There requires consideration of cost-effective ways to utilize liquid biopsy
Written by: Zachary Klaassen, MD, MSc – Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, Twitter: @zklaassen_md at the 2020 Société Internationale d'Urologie Virtual Congress (#SIU2020), October 10th - October 11th, 2020
References:
1. Heller G, McCormack R, Kheoh T, et al. Circulating Tumor Cell Number as a Response Measure of Prolonged Survival for Metastatic Castration-Resistant Prostate Cancer: A Comparison with Prostate-Specific Antigen Across Fie Randomized Phase III Clinical Trials. J Clin Oncol2018 Feb 20;36(6):572-580.
2. Armstrong AJ, Halabi S, Luo J, et al. Prospective multicenter validation of androgen receptor splice variant 7 and Hormone Therapy Resistance in High-Risk Castration-Resistant Prostate Cancer: The PROPHECY Study. J Clin Oncol2019 May 1;37(13):1120-1129.
3. Goodall J, Mateo J, Yuan W, et al. Circulating cell-free DNA to Guide Prostate Cancer Treatment with PARP Inhibition. Cancer Discov2017 Sep;(7)9:1006-1017.

