(UroToday.com) The 2023 SESAUA annual meeting included a State-of-the-Art lecture presentation by Dr. Julio Pow-Sang discussing what has changed in advanced imaging for prostate cancer. Dr. Pow-Sang started by highlighting that much has changed of the past years, as highlighted by the following:
- Enhanced imaging technology – for diagnosis, staging, follow-up, and treatment
- Imaging is a critical component of newer technologies/processes improving prostate cancer care: with biomarkers, telemedicine, artificial intelligence, and office work flow
- Mastering imaging technology and their interpretation: prostate MRI, PSMA PET/CT, and prostate micro ultrasound
With regards to prostate cancer assessment tools, traditionally we have had clinical information (age, PSA, symptoms, signs, medical and surgical history), pathology (location, grade group, extension), and conventional imaging (bone scan, CT scan). However recently we have molecular biomarkers (blood, urine, tissue) and advanced imaging (prostate MRI, PSMA PET/CT, prostate micro ultrasound). Dr. Pow-Sang emphasized that the key is integration of these technologies and processes.
Dr. Pow-Sang then discussed a clinical case, but emphasized that we should think about the case like we are practicing in 2011 to emphasize how far we have come. This was a 50 year old male referred from primary care for evaluation of an elevated PSA to 5 ng/mL, AUA symptom score of 5, SHIM score of 25, and no significant medical history. His digital rectal exam was negative, repeat PSA was 4.8 ng/mL and free PSA was 18%. He subsequently underwent a 12 core transrectal ultrasound guided systematic biopsy, which was negative. In 2012, his PSA was now 6.5 ng/mL (15% free), he remained asymptomatic, his urine PCA3 was borderline at 45, but he was quite anxious about the increasing PSA. A repeat 12 core biopsy was again negative. In 2014, his PSA was now up to 10.3 ng/mL, a third biopsy was negative, however a ConfirmMDx test on his biopsy tissue was positive. Additionally, a PHI was 49 (0-26.9: 10% probability of cancer; >55: 50% probability of cancer). He then had a 4th, 20-core saturation biopsy that showed GG4 prostate cancer in the right anterior quadrant. His bone scan and staging CT pelvis was negative. He subsequently underwent a robotic prostatectomy with pelvic lymph node dissection in 2014 with pathology showing pT3N0M0 (0 out of 14 lymph nodes positive), GG 4 prostate cancer with extracapsular extension and positive margins. His one month post-op PSA was undetectable, and he was presented with the option of adjuvant versus salvage radiotherapy, electing for close follow-up of his PSA, which was undetectable for 3 years. Unfortunately, the patient had a PSA recurrence in 2017, with a PSA of 0.25 ng/mL, with a repeat 6 months later of 0.30 ng/mL. He underwent salvage radiotherapy and had an undetectable PSA for 2 years. However, in 2019, his PSA started to rise, his re-staging bone scan and CT scan were negative, and he continued to follow with periodic PSA surveillance. By 2020, his PSA doubling time was 10 months and he started on hormonal therapy.
Fast forwarding to 2023, if we saw this exact same patient, we would have multiple new options for workup. With regards to biomarkers, we could use blood (4Kscore, PHI) or urinary (ExoDx, SelectMDx) markers, and for imaging we have prostate MRI and micro ultrasound. This patient had a multiparametric MRI, which showed two PI-RADS 4 lesions in the center of the gland, no extracapsular extension, no lymphadenopathy, no bone lesions, a volume of 35 cc and a PSA density of 0.14:
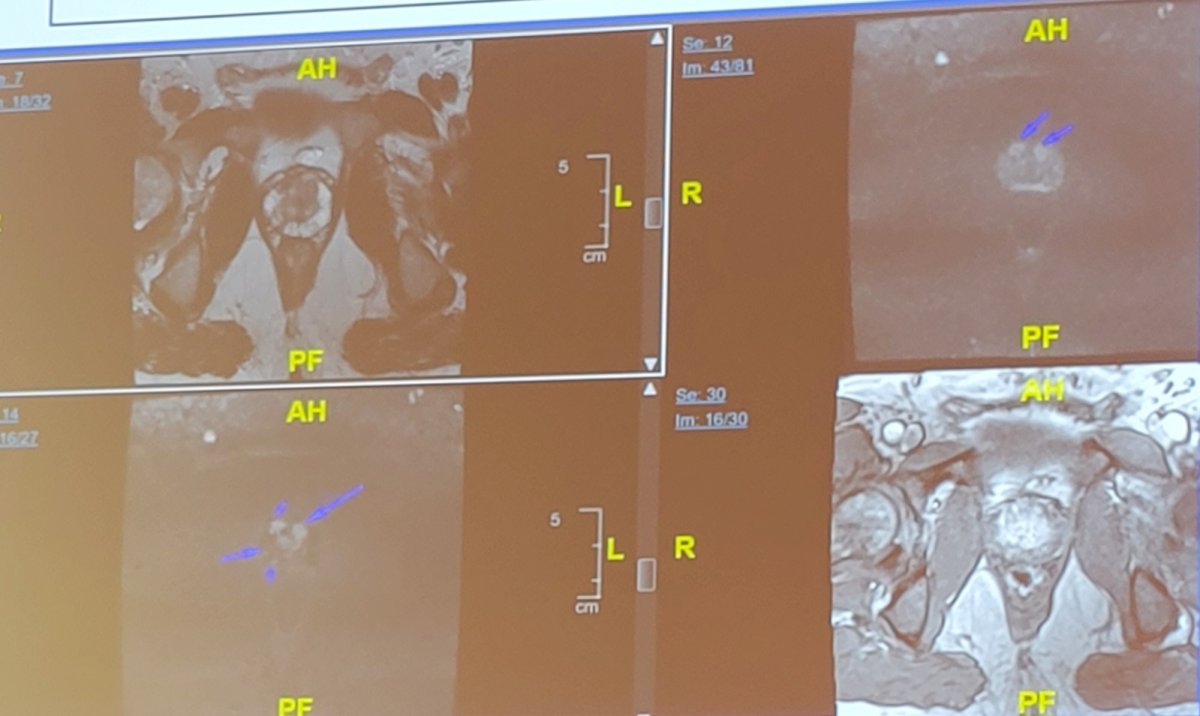
He then underwent a transperineal MRI fusion biopsy, with both regions of interest showing GG2 disease (40% of pattern 4 in each), and the 12-core systematic biopsy negative. He then underwent a robotic prostatectomy with GG2, organ confined disease, negative margins, pT2 prostate cancer.
Dr. Pow-Sang emphasized that multiparametric prostate MRI has changed the work and assessment of elevated PSA/prostate cancer. A well performed MRI gives the clinician T2W axial, T2W coronal, T2W sagittal, dynamic contrast enhanced (DCE), diffusion weighted (DWI), and ADC map images. The following figure highlights how we should think about PI-RADS lesions on the DWI/ADC and T2W image phases:1
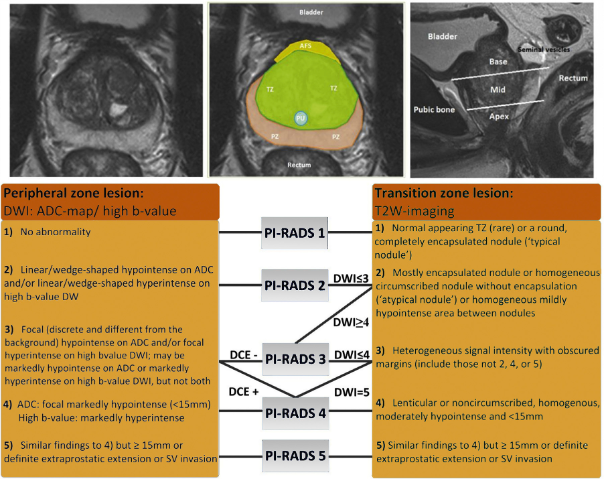
Dr. Pow-Sang summarized that four key trials have further clarified the role of targeted biopsy, notably the 4M trial2, PROMIS trial3, PRECISION4, and the MRI-FIRST trial5:

To conclude the MRI section of his talk, Dr. Pow-Sang notes that the next frontier is to improve cost, speed, and availability with the continued emergence of biparametric MRI versus multiparametric MRI.
Switching to PSMA PET/CT, Dr. Pow-Sang notes the history and PSMA milestones of this type of advanced imaging [6]:

To illustrate, Dr. Pow-Sang presented a case of a 71 year old that previously had undergone radiotherapy in 2015 with a subsequent PSA recurrence: 0.41 ng/mL in June 2021, and 0.74 ng/mL in August 2022. A prostate biopsy in September 2022 subsequent showed prostate cancer in the right mid gland and right base. He was interested in salvage therapy, thus underwent a bone scan that was negative, an MRI that was unclear, and eventually a PSMA PET/CT that showed seminal vesicle invasion, rectal wall involvement, and a presacral lymph node:
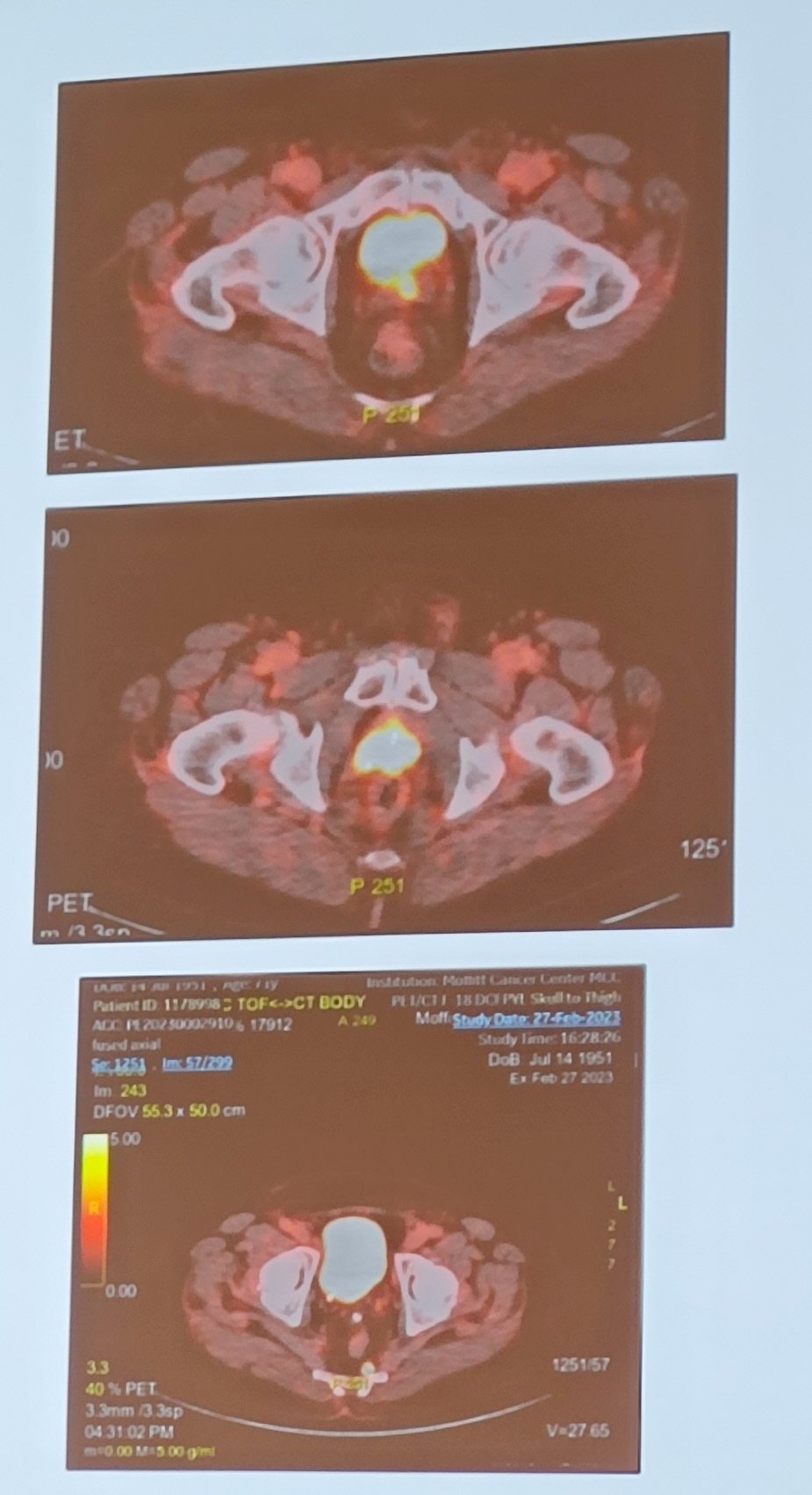
Dr. Pow-Sang emphasized that the most recent update of the NCCN prostate cancer guidelines state that for localized prostate cancer patients with unfavorable intermediate, high, and very high risk disease, “because of the increased sensitivity and specificity of PSMA PET tracers for detecting micrometastatic disease compared to conventional imaging (CT, MRI) at both initial staging and biochemical recurrence, the panel does not feel that conventional imaging is a necessary prerequisite to PSMA-PET and the PSMA-PET/CT or PSMA-PET/MRI can serve as an equally effective, if not more effective front-line imaging tool for these patients.” In fact, the PRIMARY score is also assessing the utility of PSMA PET/CT for intraprostatic assessment of clinically significant prostate cancer, with the following figure highlighting the PRIMARY scoring system:
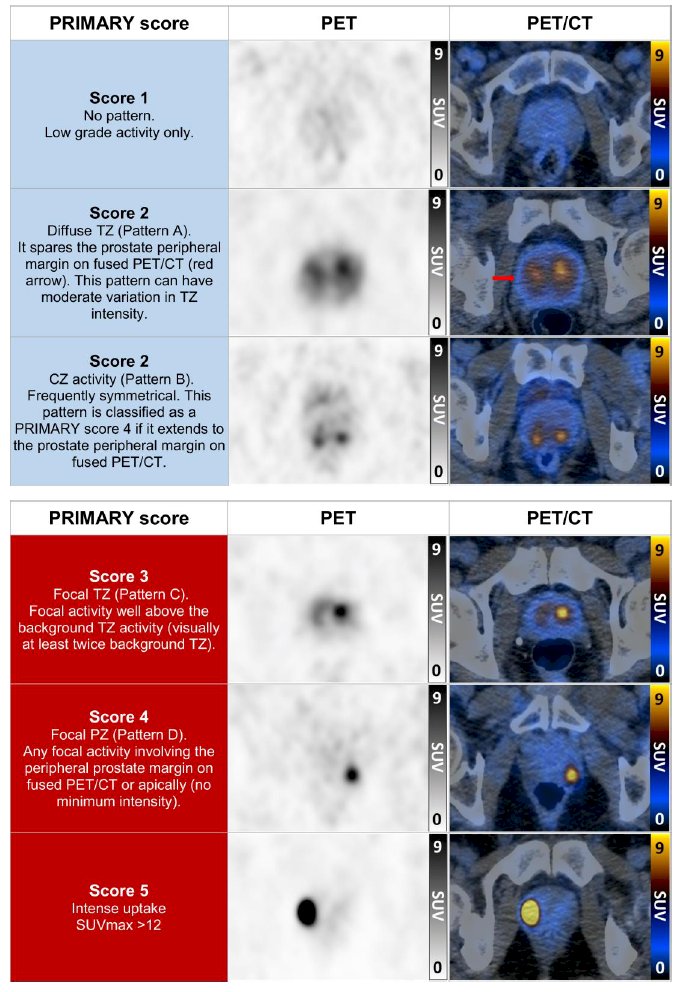
Additionally, the DEPROMP trial is assessing the additive value of PSMA PET/CT-guided biopsy for prostate cancer management in biopsy naïve men. The study design for this trial is as follows:

In this trial, all patients will undergo both mpMRI and PSMA-PET/CT, followed by all patients undergoing a systematic biopsy followed by a targeted biopsy of suspicious lesions (MRI and/or PSMA-PET/CT). At the time of the interim analysis of the 100 patients presented at EAU 2023, the addition of PSMA PET/CT-targeted biopsies to the standard of care practice (systematic + MR-targeted biopsies) was associated with a 4% increase in the detection of clinically significant prostate cancer and a 2% decrease in non-significant PCa. However, had PSMA-PET/CT-targeted biopsies been performed instead of MR-targeted biopsies, this would have led to a 3% increased detection of clinically significant prostate cancer and a 1% decrease in non-significant prostate cancer detection. Furthermore, the addition of a PSMA-PET/CT with targeted biopsies of positive lesions affected therapy decisions 53% of the time. This effect was most notable in the 48 patients with clinically significant prostate cancer, with treatment decision altered in 85% of patients (41/48).
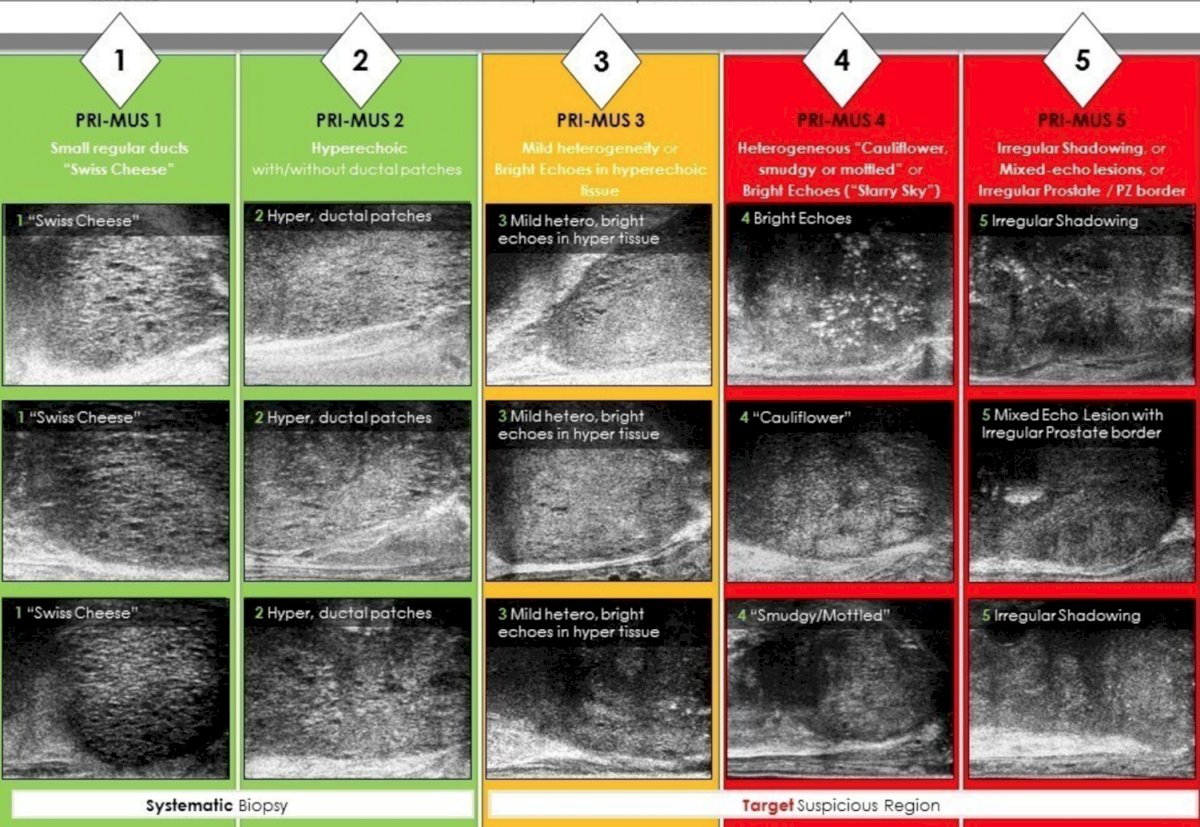
To conclude his state of the art lecture, Dr. Pow-Sang discussed micro-ultrasound. This technology uses 29 MHz, with 300x increased image resolution, derives a PRI-MUS score, and may be an alternative/complement to prostate MRI. The following figure summarizes the PRI-MUS score:
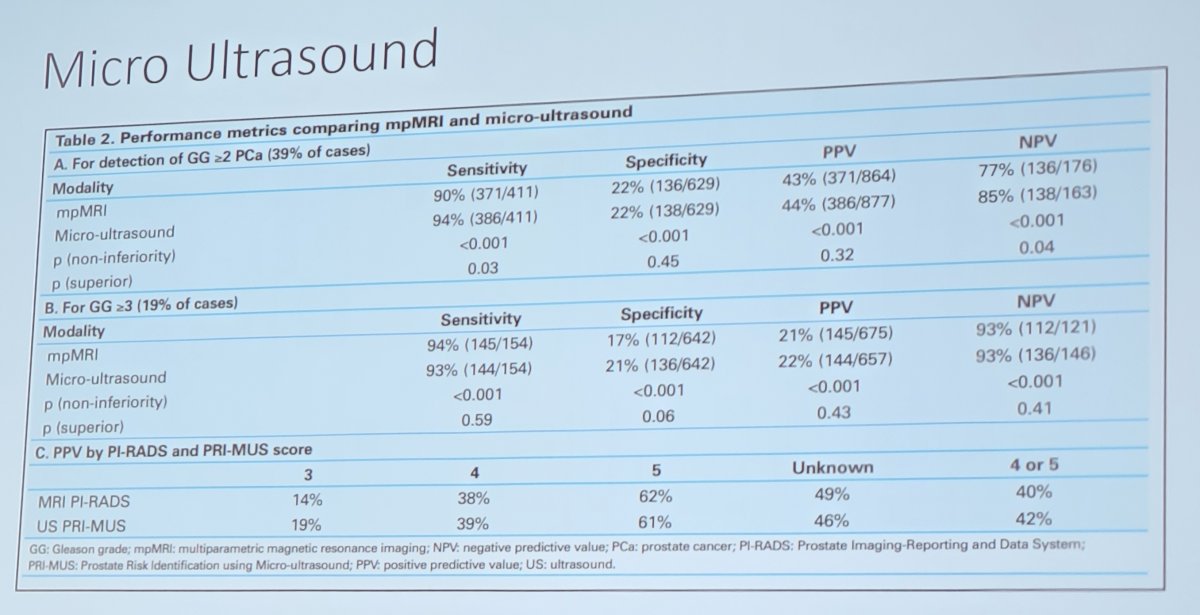
Work from Klotz et al. [8] showed that in a multicenter registry, micro-ultrasound had comparable or higher sensitivity for clinically significant prostate cancer compared to mpMRI, with similar specificity:
Dr. Pow-Sang concluded his presentation by highlighting what has changed in the last several years:
- Referrals for elevated PSAs
- Telemedicine initial assessment by Advanced Practice Providers
- Evaluation algorithms: biomarkers versus imaging
- Remote/local imaging with link to radiologists for review and interpretation
- Artificial intelligence, for example GPT-4, to aid urologists with imaging interpretation and plan of care
- Telemedicine/live follow-up with a urologist to review information and determine the need for biopsy
Presented by: Julio M. Pow-Sang, MD, Moffitt Cancer Center, Tampa, FL
Written by: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, @zklaassen_md on Twitter during the 2023 Southeastern Section of the American Urological Association (SESAUA) Annual Meeting, Amelia Island, FL, Wed, Mar 15 – Sat, Mar 18, 2023.
References:
- Israel B, van der Leest M, Sedelaar M, et al. Multiparametric Magnetic Resonance Imaging for the Detection of Clinically Significant Prostate Cancer: What Urologists Need to Know. Part 2: Interpretation. Eur Urol. 2020 Apr;77(4):469-480.
- van der Leest M, Cornel E, Israel B, et al. Head-to-head comparison of transrectal ultrasound-guided prostate versus multiparametric prostate resonance imaging with subsequent magnetic resonance-guided biopsy in biopsy-naïve men with elevated prostate-specific antigen: A Large Prospective multicenter study. Eur Urol. 2019 Apr;75(4):570-578.
- Ahmed HU, El-Shater Bosaily A, Brown LC, et al. Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): A paired validating confirmatory study. Lancet 2017;389(10071):815-822.
- Kasivisvanathan V, Rannikko AS, Borghi M, et al. MRI-targeted or standard biopsy for prostate cancer diagnosis. N Engl J Med 2018;378(19):1767-1777.
- Rouviere O, Renard-Penna R, Claudon M, et al. Use of prostate systematic and targeted biopsy on the basis of multiparametric MRI in biopsy-naïve patients (MRI-FIRST): A prospective, multicentre, paired diagnostic study. Lancet Oncol 2019 Jan;20(1):100-109.
- Kupperman D, Calais M, Marks LS. Imaging Prostate Cancer: Clinical Utility of Prostate-Specific Membrane Antigen. J Urol. 2022 Apr;207(4):769-778.
- Emmett L, Papa N, Buteau J, et al. The PRIMARY Score: Using Intraprostatic 68Ga-PSMA PET/CT Patterns to Optimize Prostate Cancer Diagnosis. J Nucl Med. 2022 Nov;63(11):1644-1650.
- Klotz L, Lughezzani G, Maffei D, et al. Comparison of micro-ultrasound and multiparametric magnetic resonance imaging for prostate cancer: A multicenter, prospective analysis. Can Urol Assoc J. 2021 Jan;15(1):E11-E16.

