(UroToday.com) The 2023 SESAUA annual meeting included a bladder cancer session, featuring a presentation by Dr. Pushan Prabhakar discussing mental health changes in patients undergoing radical cystectomy with urinary diversion. For decades, radical cystectomy with urinary diversion has been the standard treatment for localized muscle-invasive bladder cancer, however this procedure can adversely affect a patient’s quality of life. Very few studies in the literature have focused on mental health outcomes such as depression in these patients, with an estimated prevalence of mental health illness of ~50%.1 Dr. Prabhakar and colleagues aimed to explore the depression score changes perioperatively for patients undergoing radical cystectomy with urinary diversion.
This was a consecutive series (September 2021 – present) of patients undergoing radical cystectomy with urinary diversion for muscle-invasive bladder cancer that were screened using the Beck Depression Inventory-II (BDI-II). Responses were recorded pre-surgery, 6 weeks after surgery, 3 months after surgery, and 6 months after surgery. Based on guidelines, the BDI-II was scored as:
- Minimal range: 0-13
- Mild depression: 14-19
- Moderate depression: 20-28
- Severe depression: 29-63
At the time of the analysis, 47 patients had completed the pre-surgery questionnaire with a mean age of 73.8 years. Of these patients, 34 were males and 13 were females, with 45 undergoing an ileal conduit for urinary diversion. At baseline, the mean BDI-II score was 5.36 (range 0-16). At 6 weeks after surgery, 31 patients had minimal range, one patient each had mild, and moderate depression with a mean score 6.0 (range 0-22). From the baseline, two patients had no change, 14 scored lower, and 17 patients had an increased score. One patient had a significant migration between groups from minimal to moderate depression. At 3 months post surgery, 27 patients scored in the minimal range category with a mean BDI-II of 4.0 (0-13). The most notable finding was that 18 patients had a decrease in their score. Finally, at 6 months, the mean BDI-II score was 2.58 (0-5) with six patients showing no change, four showing a decrease, and only 1 patient having an increase. A summary of the findings is as follows:
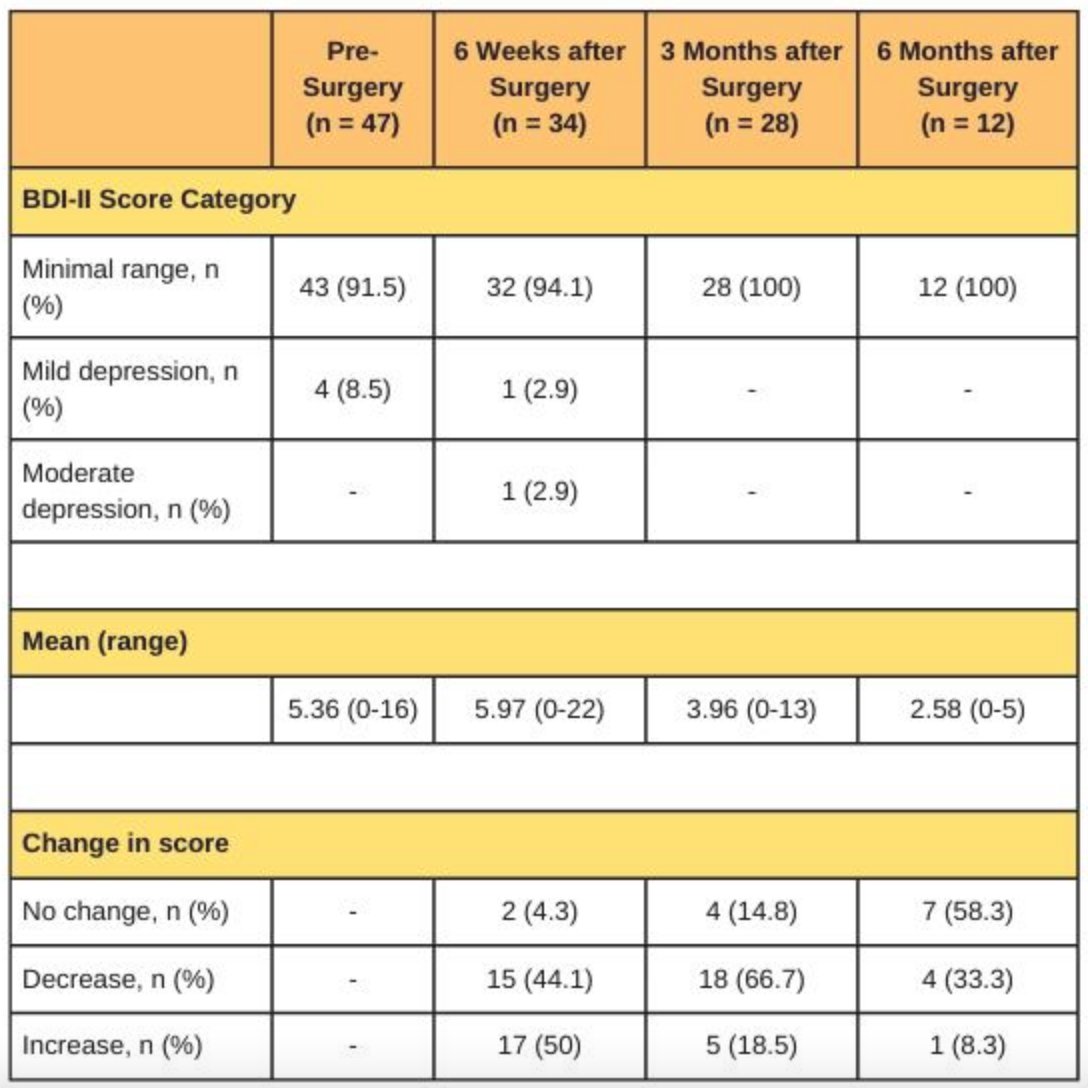
Dr. Prabhakar concluded his presentation discussing mental health changes in patients undergoing radical cystectomy with urinary diversion with the following take-home messages:
- The BDI-II scores predominantly increased over time from pre-surgery to 6 weeks after surgery
- Following this, the trend in the scores showed a decrease over time or no significant change
- This shows that the immediate post-operative period is when patients would require effective counseling and referrals to supportive services as needed
- This study is ongoing and objective evaluation of depression in postoperative cystectomy patients with a larger patient population would be beneficial
Presented By: Pushan Prabhakar, MBBS, MPH, Miami Cancer Institute, Baptist Health South Florida, Miami, FL
Co-Authors: Hariharan Ganapathi, MD2, Nikhil Kulkarni3, Ahmed Eldefrawy, MD1,3, Jorge Caso, MD1,3, Murugesan Manoharan, MD1,3
Affiliations: 1. Miami Cancer Institute, Baptist Health South Florida, Miami, FL, 2. University of South Florida, Tampa, FL, 3. FIU Herbert Wertheim College of Medicine, Miami, FL
Written by: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, @zklaassen_md on Twitter during the 2023 Southeastern Section of the American Urological Association (SESAUA) Annual Meeting, Amelia Island, FL, Wed, Mar 15 – Sat, Mar 18, 2023.
References:
1. Jazzar U, Yong S, Klaassen Z, et al. Impact of psychiatric illness on decreased survival in elderly patients with bladder cancer in the United States. Cancer 2018 Aug 1;124(15):3127-3135.


