(UroToday.com) The first Renal Cancer session at this year’s European Association of Urology (EAU) Section of Oncological Urology (ESOU) 2021 virtual annual meeting focused on localized disease and was divided into two primary sections, the first focusing on key points in partial nephrectomy while the second examined approaches to larger renal masses. In the first mini-session examining key points in partial nephrectomy, Dr. Mottrie discussed considerations when considering ischemia versus no ischemia in robotic-assisted partial nephrectomy.
Dr. Mottrie began by highlighting data from a systematic review published in European Urology which, after including 91 studies performed between 2005 and 2014, concluded that 20-25 minutes represents the most accurate cut-off for clinically relevant ischemia. The authors also concluded that the use of no-ischemia or partial occlusive approaches may improve functional outcomes.
A more recent systematic review compared no-ischemia versus warm ischemia. Among 14 included studies of approximately 1400 patients, no-ischemia approaches were associated with better preservation of renal function without significant differences in operative time or estimated blood loss. Similarly, a systematic review of selective versus main artery clamped demonstrated no differences in ischemia time or complications but did show a lower decrease in renal function for patients who received selective clamping. However, selective clamping had a longer operative time and greater blood loss.
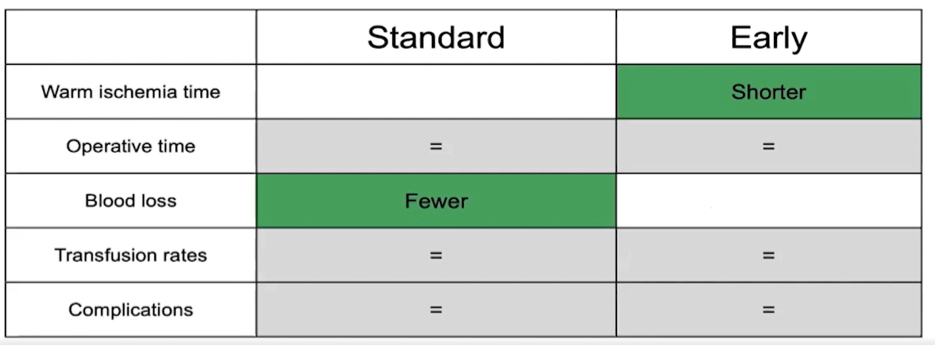
In addition to the question of what to clamp is when to unclamp. Dr. Mottrie then highlighted data comparing standard with early unclamping. Early unclamping was associated with shorter warm ischemia time at the expense of higher blood loss.
He then described a recent systematic review of ischemia techniques in nephron-sparing surgery, again published in European Urology, which included 156 studies and 22,626 patients comparing cold vs. warm vs. no-ischemia techniques. Overall, the authors concluded that there were significant limitations to the available literature and thus, no approach could be recommended over the others.
Dr. Mottrie then highlighted what he sees at four key points in performing robotic-assisted partial nephrectomy:
1. avoiding renal artery clamping where feasible, or performing superselective clamping
2. performing surgery at the lowest feasible intra-abdominal pressure (5 mmHg)
3. avoiding placement of a drain, when safe and feasible
4. avoiding suture of the resection bed, again when technically feasible. This is based on the rationale that penetration of the needle into renal parenchyma may cause vascular injuries leading to an increased loss of functional nephrons.
These four approaches aim to preserve renal function. Dr. Mottrie then highlighted their own data comparing suture-less robotic-assisted partial nephrectomy to a standard approach, based on a propensity score-matched cohort. The suture-less approach was associated with shorter ischemia and operative times, similar rates of complications, and shorter length of stay. Notably, among 29 patients, there were no patients who experienced bleeding or urine leaks.

Presented by: Alex Mottrie, MD, PhD, Head of the Urology Department of the Onze Lieve Vrouwziekenhuis (OLV) Hospital in Aalst, Belgium, CEO of the ORSI Academy in Melle, Belgium.
Written by: Christopher J.D. Wallis, MD, Ph.D., FRCSC, Instructor in Urology, Vanderbilt University Medical Center, Nashville, Tennessee @WallisCJD on Twitter during the 18th Meeting of the EAU Section of Oncological Urology (ESOU21), January 29-31, 2021

