- “When in doubt, take it out”
Subsequently, Dr. Heidenreich has challenged the dogma and published several papers describing partial orchiectomy (first in 1995), which required no testosterone supplementation during follow-up. An updated manuscript in 2001 of 73 patients with median 91 months (range 3-191) follow-up, reported that 98.6% of patients had no evidence of disease and one died of systemic tumor progression1. No relapsed occurred in 46 patients with associated testicular intraepithelial neoplasia treated with local radiation; 4 patients had local recurrence, salvaged with radical orchiectomy.
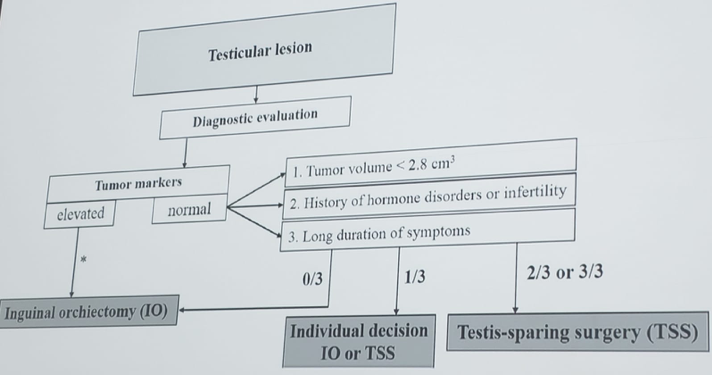
According to Dr. Heidenreich, organ-sparing surgery is indicated for:
- Bilateral metachronous/synchronous testis cancer
- Tumor diameter < 2 cm (50% parenchyma remaining)
- Normal serum testosterone and LH
- Postoperative radiation therapy
- “Always act bilateral”
Dr. Heidenreich concluded stating:
- “When in doubt, take it out” – when in doubt, take a frozen section and save the testis
- “Always act bilateral” – only act bilateral if residual masses are outside the primary template
Presented by: Axel Heidenreich, Professor of Urology, Chairman, and Director of the Department of Urology, Uro-Oncology, Robot-Assisted, and Specialized Urologic Surgery at the University Hospital in Cologne Germany
Written by: Zachary Klaassen, MD, MSc – Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, Twitter: @zklaassen_md, at the 16th Meeting of the European Section of Oncological Urology, #ESOU19, January 18-20, 2019, Prague, Czech Republic
References:
- Heidenreich A, Weissbach L, Holtl W, et al. Organ sparing surgery for malignant germ cell tumor of the testis. J Urol 2001 Dec;166(6):2161-2165.
- Paffenholz P, Held L, Loosen SH, et al. Testis sparing surgery for benign testicular masses: Diagnostics and Therapeutic Approaches. J Urol 2018 Aug;200(2):353-360.
- Beck SD, Foster RS, Bihrle R, et al. Is full bilateral retroperitoneal lymph node dissection always necessary for postchemotherapy residual tumor? Cancer 2007 Sep 15;110(6):1235-1240.
- Heidenreich A, Pfister D, Witthuhn R, Thuer D, Albers P. Postchemotherapy retroperitoneal lymph node dissection in advanced testicular cancer: radical or modified template resection. Eur Urol 2009 Jan;55(1):217-224

