He again reviewed the basics of bladder cancer management. As background, it is well established that 20-30% of newly diagnosed bladder cancers are muscle-invasive (MIBC), and for these patients (and patients who progress to MIBC), the standard of care treatment is neoadjuvant chemotherapy and radical cystectomy with urinary diversion. Alternatives include trimodal therapy, though this is not yet considered a standard of care. Radical cystectomy is associated with significant detrimental effects on patient quality of life, urinary and sexual function, and has an impact on patient social and emotional health, body image and psychosocial stress. While most patients undergo urinary diversion with an incontinent ileal conduit, some patients (male and female) undergo continent neobladder formation.
In prostate cancer management, the goal is for the trifecta: disease free, potency and continence. With radical cystectomy and neobladder formation, that is also the same goal – achieve oncologic control similar to radical cystectomy with ileal conduit, without sacrificing voiding and sexual function. Yet, it is not always easy to achieve.
Urs Studer first published the concept of nerve sparing with orthotopic neobladder formation in 20041, demonstrating improved continence and erectile function even at that time. In a systematic review, sexual function was preserved with robotic cystectomy in 63-100% of patients2. This demonstrates that good nerve sparing is associated with good functional outcomes after robotic surgery. But, finding that nerve-sparing plane is important.
In the diagram below3, the difference in planes between a standard non-nerve sparing radical cystectomy, a nerve-sparing radical cystectomy, and a prostate sparing radical cystectomy are demonstrated.
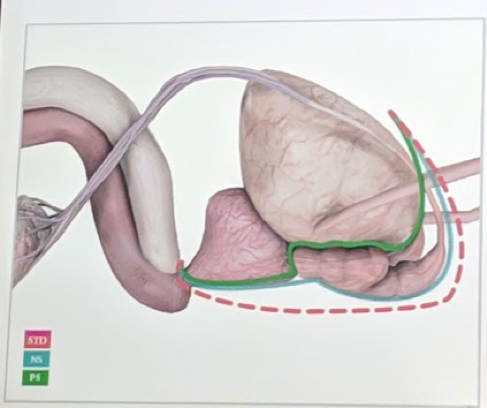
The blue line is the nerve-sparing plane. The green line is one of the prostate sparing planes.
He then reviewed a video of their nerve sparing during a robotic radical cystectomy. Essentially, the key is to really hug the prostate and the seminal vesicles, sparing all the tissue laterally and inferior to the prostate without violating the capsule.
He then reviewed a more recent report of his institution’s functional outcomes in robotic nerve-sparing radical cystectomy4. In this, they found that 90% of men had sexual function return sufficiently to have intercourse, 3 of them with medical assistance. By 12 months, 90% were also continent – 95% had good daytime continence and 85% good night-time continence. He did note that 4 had to self-catheterize.
Contraindications to nerve-sparing are:
Clinical T4a disease
Presence of ipsilateral hydronephrosis
Suspicion for tumor invasion at the bladder neck
Previous erectile dysfunction
Presented by: Joan Palou, MD, Ph.D., FEBU, Chairman, Department of Urology, Fundació Puigvert, University Autonoma of Barcelona, Spain Barcelona
Written by: Thenappan Chandrasekar, MD. Clinical Instructor, Thomas Jefferson University, Twitter: @tchandra_uromd, @TjuUrology, at the 16th Meeting of the European Section of Oncological Urology, #ESOU19, January 18-20, 2019, Prague, Czech Republic
References:
1. Urs Studer, 2004 (JUrol)
2. Yuh et al. (EU 2015)
3. Puppo et al (J Urol 2007)
4. Kanashiro et al. (2016) Asociación Española de Urología, Elsevier España
Further Related Content:
Open Nerve-Sparing Radical Cystectomy
Prostate Sparing Approaches

