In this study, the authors look at the data from the initial and confirmatory biopsy in a novel way, in an effort to better identify men who will progression onto treatment. This study describes a novel clinical marker, called total cancer location (TCLo) density index, and aimed to determine its performance in predicting clinical progression (CP) and grade progression (GP).
The authors completed a retrospective study of patients on AS at their institution, one with a long history of AS utilization. They only looked at men who were eligible for AS after confirmatory biopsy (CBx). They excluded patients with Gleason ≥7 at CBx, less than 2 years follow-up and incomplete data.
They defined TCLo as the number of locations with positive cores at diagnosis (DBx) and CBx. This was not limited to sextant region, so the TLCo could range higher than 6. However, if the same terminology was used in subsequent biopsies, then they were considered the same region. At a minimum, TCLo was 1.
TCLo density was TCLo / prostate volume (PV). Prostate volume was determined by TRUS (at the time of TRUS Biopsy). Clinical progression (CP) was defined as progression to any active treatment while grade progression (GP) occurred if Gleason ≥7 was identified on repeat biopsy or surgical pathology.
Between 2012-2015, 421 patients had a CBx; of these, 181 patients met inclusion criteria. The mean age of patients at the start of AS was 62.6 years (SD=7.13) and the median PSA at diagnosis was 5.16 ng/mL (IQR=3.44). Mean PV was 41.0 mL (IQR 22.5).
The median TCLo density was 0.049 (IQR=0.06). This was used as a cutoff as a high (>0.05) and low (<= 0.05).
A high TCLo density score (>0.05) was independently associated with time to CP (HR 4.7, 95% CI: 2.62-8.42, p<0.001) and GP (HR 4.25, 95% CI: 2.06-8.74, p<0.001). This is demonstrated in the figure below:
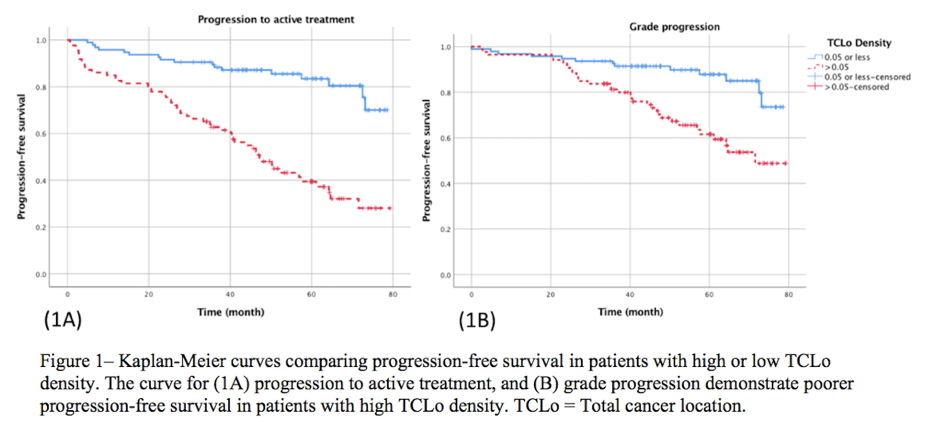
When compared to %positive cores, another commonly used clinical biomarker, TCLo density performed better than percentage positive cores at confirmatory biopsy in predicting CP – see figure below:
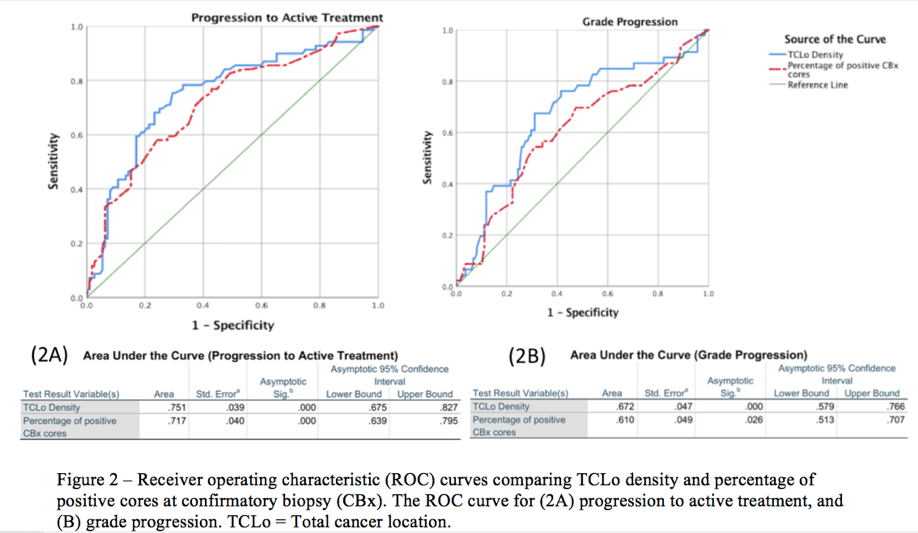
It did not predict GP, however.
Based on this, the authors feel that this may be an additional biomarker that may be utilized to better select patients for AS or primary treatment. Yet, some caveats:
- This data is similar to PSA density and %positive cores – both of which have an important role in clinical models
- Requires validation in other large datasets
- Due to the nature of the TCLo definition, there could be a high degree of variability in TCLo scoring – making comparisons more difficult
Presented by: Guan Hee Tan, Clinical Fellow in Uro-Oncology at the University of Toronto
Written by: Thenappan Chandrasekar, MD (Clinical Instructor, Thomas Jefferson University) (twitter: @tchandra_uromd, @TjuUrology) at the 34th European Association of Urology (EAU 2019) #EAU19, conference in Barcelona, Spain from March 15-19, 2019.

