(UroToday.com) The 2023 AUA annual meeting included an advanced prostate cancer session, featuring a presentation by Dr. Neal Shore discussing efficacy and safety of darolutamide in combination with ADT and docetaxel in the North American population in ARASENS. In ARASENS (NCT02799602), darolutamide + ADT + docetaxel significantly reduced the risk of death by 32.5% (HR 0.68, 95% CI 0.57–0.80; p < 0.0001) vs placebo + ADT + docetaxel in patients with metastatic hormone-sensitive prostate cancer (mHSPC).1 Additionally, darolutamide maintained quality of life, with similar control of disease-related physical symptoms and pain vs placebo, and had a favorable safety profile. At the 2023 AUA annual meeting, Dr. Shore and colleagues reported clinical outcomes in North American patients in ARASENS.
This international, double-blind, phase 3 trial randomized patients 1:1 to darolutamide 600 mg twice daily or placebo in addition to ADT + docetaxel. The primary endpoint was overall survival. Key secondary endpoints included time to castration-resistant prostate cancer (CRPC) and safety. Of 1,305 patients analyzed, 244 (18.7%) were enrolled in North America (US/Canada 218/26; darolutamide/placebo 125/119), and of these, 36 (14.8%) were Black/African American patients:

Baseline characteristics of the North American population were generally similar to those of the overall population, except for the proportion of patients with de novo metastatic disease (75.8% North American vs 86.1% overall):

In North American patients, darolutamide + ADT + docetaxel was associated with overall survival benefit vs placebo + ADT + docetaxel (HR 0.59, 95% CI 0.39–0.89), with 4-year survival rates of 66% vs 50%, respectively:

Furthermore, the darolutamide vs placebo group had a longer time to CRPC (HR 0.32, 95% CI 0.21–0.48):
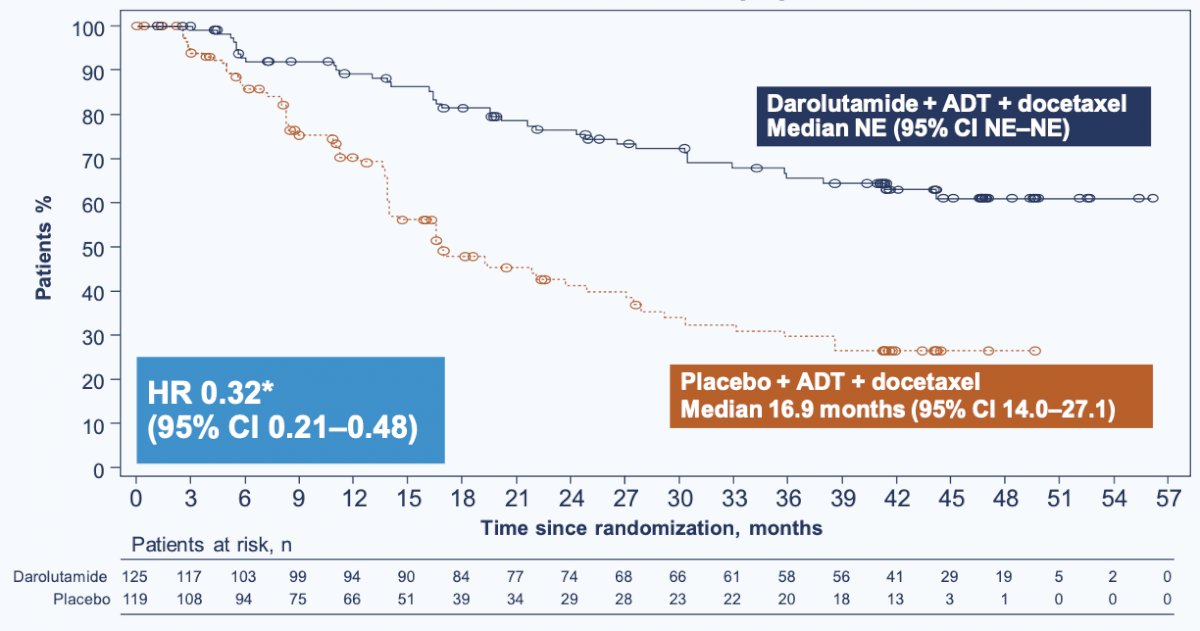
Darolutamide also showed an improvement compared with placebo in key patient-relevant secondary endpoint in the North American subpopulation:
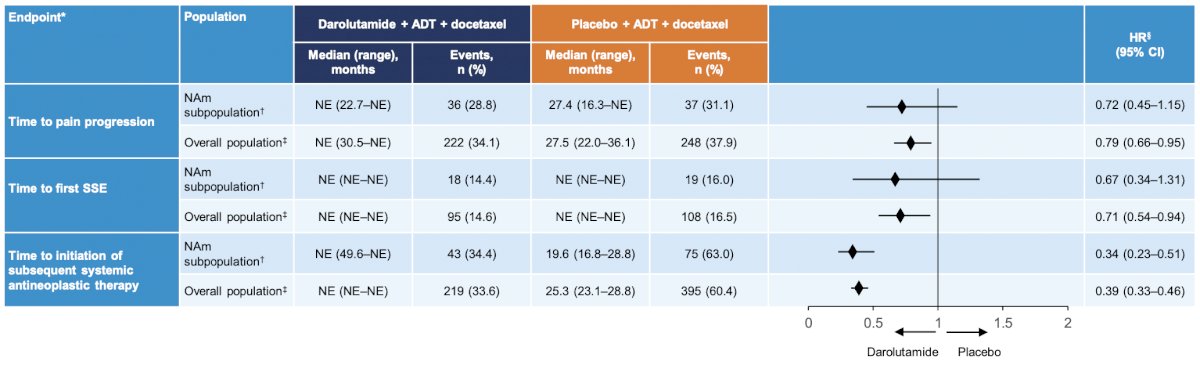
The safety profile of darolutamide in North American patients was consistent with that of the overall population: (i) grade 3/4 treatment-emergent adverse events 61% North American vs 66% overall, and (ii) serious treatment-emergent adverse events 44% North American vs 45% overall. The incidences of treatment-emergent adverse events associated with androgen receptor pathway inhibition for darolutamide vs placebo were generally consistent, particularly when adjusted for treatment exposure. The overall survival benefit and safety profile of darolutamide vs placebo was also seen in Black/African American patients, consistent with the overall population.
Dr. Shore concluded his presentation by discussing efficacy and safety of darolutamide in combination with ADT and docetaxel in the North American population in ARASENS with the following take-home messages:
- In North American patients with mHSPC, the addition of darolutamide to ADT + docetaxel led to a clinically meaningful reduction in risk of death by 41% and improved the key patient-relevant secondary endpoint of time to CRPC
- The North American subgroup analysis of the primary endpoint was planned, whereas the secondary endpoint analyses were post hoc analyses
- Incidences of treatment-emergent adverse events were generally similar between treatment groups in North American patients and consistent with the overall population
Presented by: Neal D. Shore, MD, FACS, Medical Director, Carolina Urologic Research Center, Atlantic Urology Clinics, Myrtle Beach, SC
Written by: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, @zklaassen_md on Twitter during the 2023 American Urological Association (AUA) Annual Meeting, Chicago, IL, April 27 – May 1, 2023
Reference:

