(UroToday.com) Most patients newly diagnosed with bladder cancer have non-muscle invasive disease (NMIBC). While the risk of disease progression is non-negligible, a significant portion of the health care burden associated with this condition is due to recurrence. Previous studies have demonstrated that the use of blue light flexible cystoscopy (BLFC) may increase the detection of additional cancers missed with white light cystoscopy (WLC) alone. However, its role in the surveillance of patients following intravesical therapy has not been established. In a podium presentation at the American Urologic Association Virtual Annual Meeting, Dr. Seyedian and colleagues presented the results of their analysis examining this question.
The authors examined clinicopathologic information from consecutive patients undergoing office-based BLFC who were enrolled in the Cysview registry between May 2018 and December 2020 at two high-volume academic centers. The authors excluded patients with last intravesical treatment >1 year prior. Data were stratified based on the time from last intravesical treatment.
The authors included 136 patients with a mean age of 73 years of whom 85% were male, 61% had a history of smoking and 30% had at least 2 prior bladder cancer recurrences. Prior to undergoing BLFC, 74% had high grade (HG) disease, and the highest stage prior to BLFC was Ta, T1, carcinoma in situ (CIS), and Ta/T1+CIS in 40%, 34%, 17%, and 9%, respectively. In terms of adjuvant intravesical therapy, Bacillus Calmette–Guérin (BCG) and intravesical chemotherapy were used in 83% and 17%, respectively.
Among the 136 included patients, a total of 277 BLFC were performed. WLC and BLFC were both normal in 162 (58.5%) procedures. WLC or BLFC was abnormal in 40% of post BCG and 37% of post intravesical chemotherapy cystoscopies. A total of 52 office biopsy were taken, of which, 23/52 (44%) demonstrated malignancy.
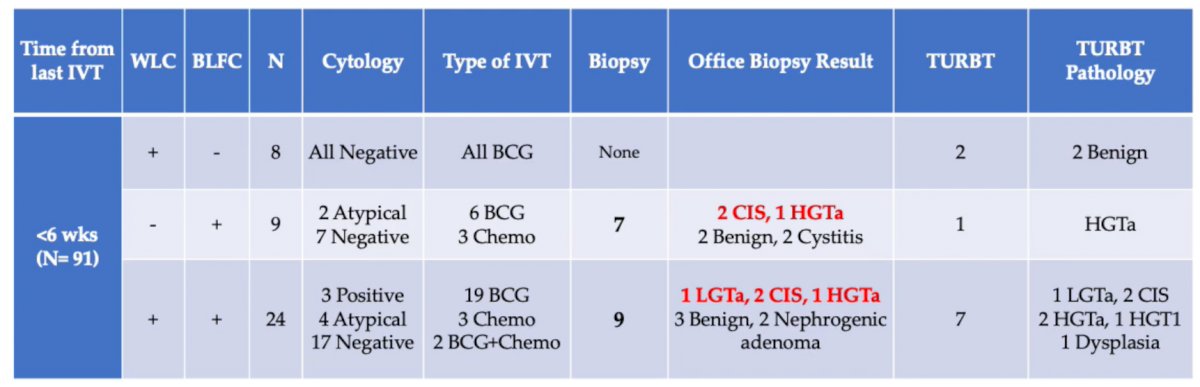
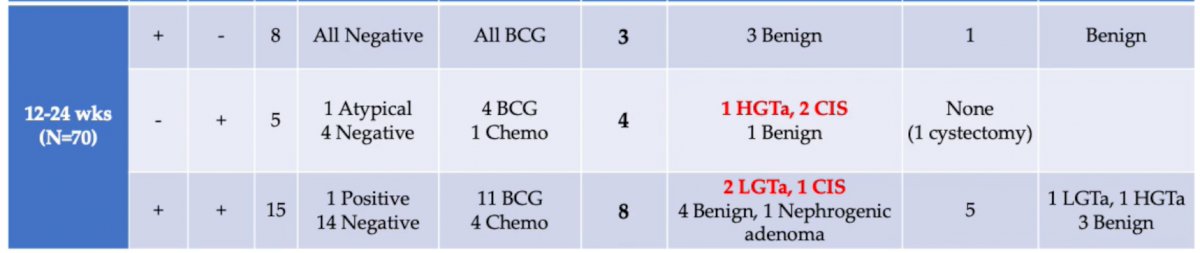
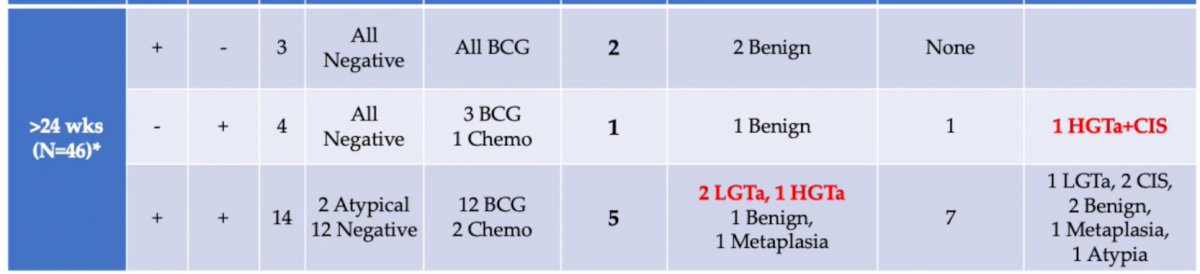
BLFC was abnormal among all patients with positive biopsies, while only 3 of 23 had positive or atypical cytology. Thus, with the gold standard of biopsy, BLFC was 100% sensitive for the detection of cancer in this cohort. WLC was normal and BLFC was abnormal in 23 (8%) procedures. Of these, 16 of 23 had an office-based biopsy, and cancer was detected in 9 of 16. Notably, as can be seen in the table, BLFC had the highest false-positive rate at <6 weeks post intravesical therapy.
Thus, the authors concluded that office-based BLFC may help improve early detection of recurrence in patients with NMIBC who have undergone intravesical therapy.
Presented by: Sanam Seyedian, MD, Department of Urology, Norris Cancer Center, University of Southern California
Written by: Christopher J.D. Wallis, University of Toronto, Twitter: @WallisCJD during the 2021 American Urological Association, (AUA) Annual Meeting, Fri, Sep 10, 2021 – Mon, Sep 13, 2021.

