In this trial, six Canadian centers were involved (Ottawa, Hamilton, Toronto, London, Quebec City, and Halifax). Patients from all centers were randomized 1:1 with the intervention group receiving 10 min of cooling with ice slush after clamping, and the control group going directly to the resection following clamping (1). In the intervention arm, the ice slush was applied in a 2 cm thick layer around the kidney, immediately following hilar clamping for 10 minutes. The ice slush was then removed, and tumor resection was performed. The randomization was performed intra-operatively before hilar clamping. The patients, pathologists, lab technicians, and data analysts were all blinded to the randomization.
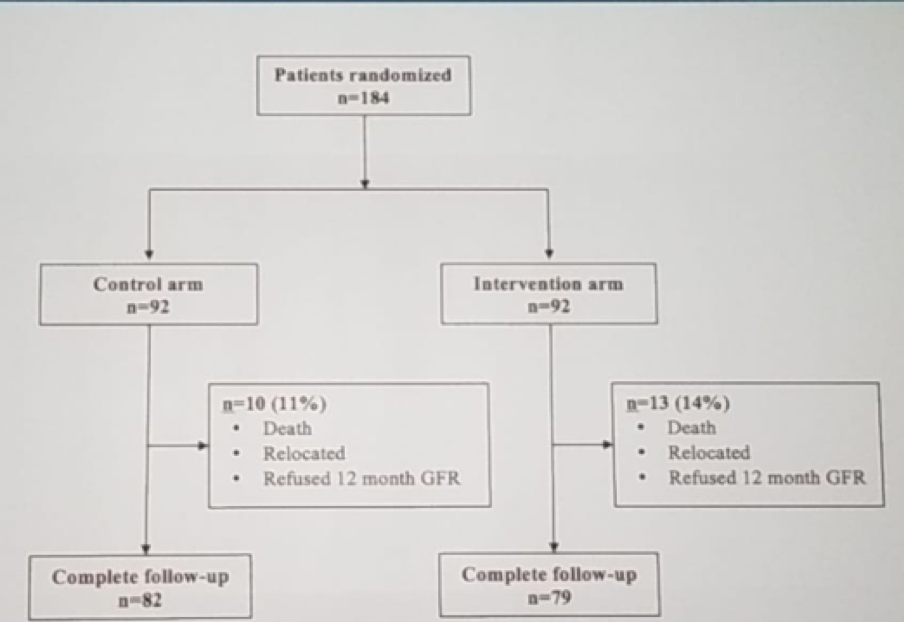
The inclusion criteria included all patients older than 18 with planned clamping on the renal hilum, and patients with multiple tumors, bilateral tumors, and a single kidney were permitted to participate. The exclusion criteria included patients on dialysis, presence of cold agglutinins, robotic partial nephrectomy planned, and planned surgery on the contralateral kidney within 12 months. The primary outcome was a renal function (Glomerular filtration rate - GFR) at 12 months with the GFR measured by DTPA plasma clearance. The secondary outcome included specifically the operated renal kidney function at 12 months. Several subgroup analyses were performed as well. These included stratification by baseline GFR (>60 vs. <60), patient age (above and below the median), and clamp time (20 and 30 min). The sample size was powered at 90% to detect a 10 ml/min/1.73 m2, with an alpha of 5%, and an estimated 5% loss to follow-up. The study flow diagram is shown in figure 1.
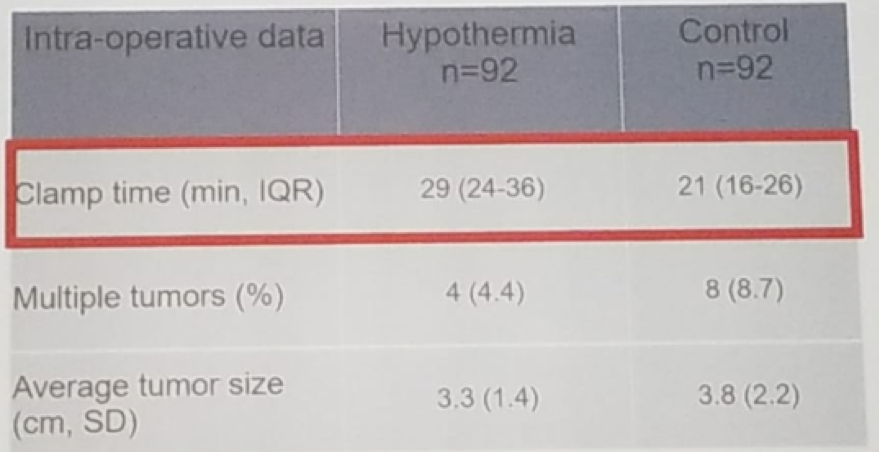
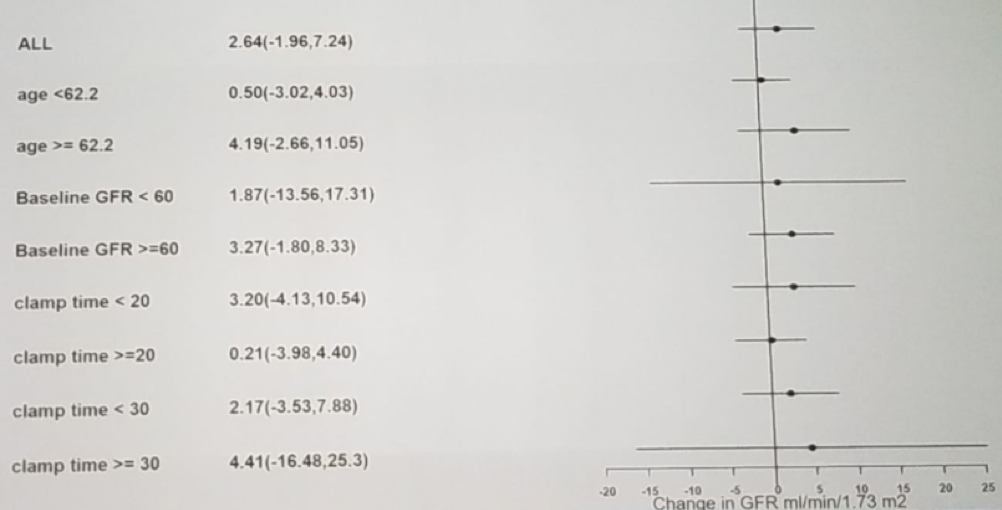
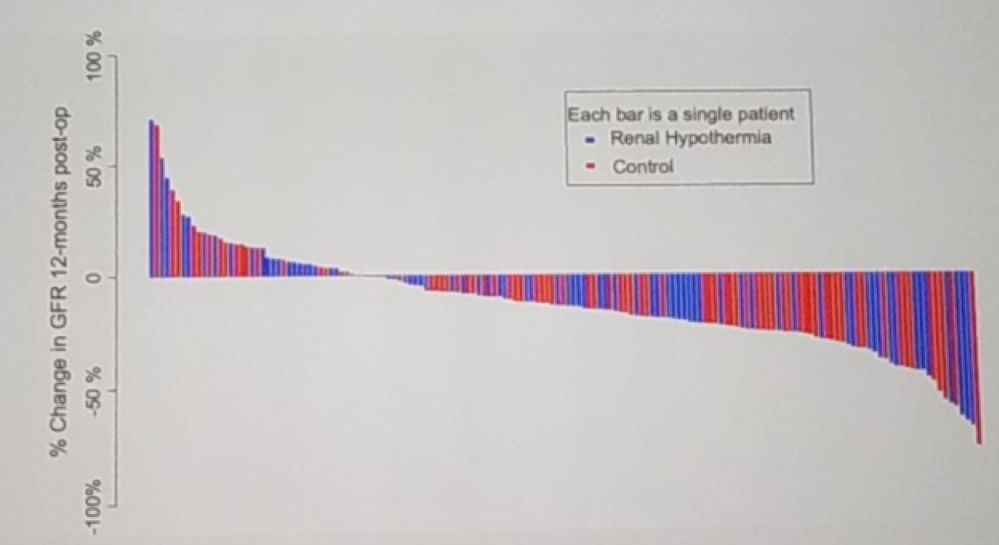
Patient demographic, clinical and baseline renal function was balanced quite well. When assessing the operative and pathology information, the clamp time was higher in the hypothermia arm (Table 1). When assessing the GFR at 12 months, no significant difference could be seen between the two groups (Figure 2). The GFR change in the operated kidney was also not significantly different between the treatment and control arm (figure 3).
Concluding his talk on this interesting level one evidence trial, Dr. Cagiannos stated that no difference in 12 months-postoperative renal function between the groups could be discerned. The effect of hypothermia was not modified by the clamp time or the baseline renal function.
Figure 1 – Flow diagram:
Presented by: Ilias Cagiannos, MD, Assistant Professor of Surgery, Department of Urology, The University of Ottawa
Written By: Hanan Goldberg, MD, Urologic Oncology Fellow (SUO), University of Toronto, Princess Margaret Cancer Centre @GoldbergHanan at the American Urological Association's 2019 Annual Meeting (AUA 2019), May 3 – 6, 2019 in Chicago, Illinois
References:
- Breau et al. BMJ OPEN 2018

