The authors recruited 179 men with a suspicious lesion on mpMRI (defined as Pi-RADs v2 ≥3). Each patient underwent micro-US targeted biopsy (with blinding of the operator to mpMRI results), mpMRI targeted biopsy and systematic biopsy. The PRI-MUS risk score was used to characterize the likelihood of cancer based on micro-US. The authors assessed diagnostic rates of prostate cancer overall and clinically significant (Gleason score ≥7, Gleason Grade Group ≥2) prostate cancer.

Among the 179 men included in this prospective cohort study, the mean age was 64.7 years and the mean PSA was 8.2 ng/mL. 92 of 179 patients (51.4%) had undergone prior prostate biopsy while the remainder were biopsy naïve. The proportion of patients diagnosed with clinically significant prostate cancer increased with a growing PRI-MUS score: 17% in PRI-MUS score 3, 41% in score 4, 61% in score 5 (p<0.001). Similarly, the likelihood of clinically significant cancer increased with a growing Pi-RADs score: 18% in Pi-RADs 3, 39% in Pi-RADs 4, and 55% in Pi-RADs 5 (p=0.002).
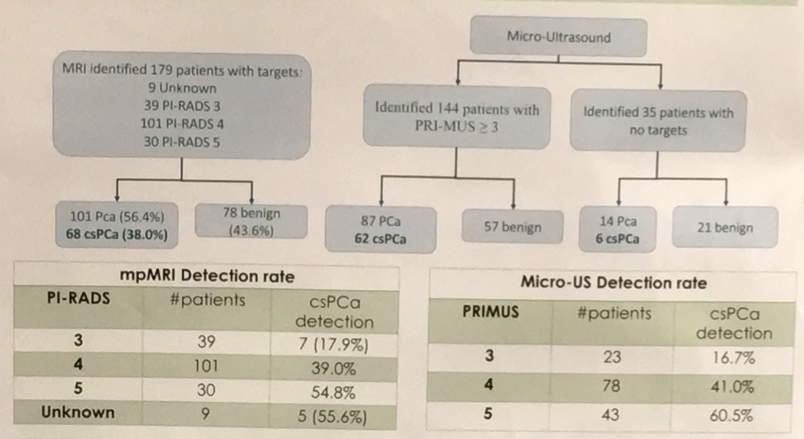
Micro-US exhibited favorable test parameters with a sensitivity of 91.2%, specificity of 25.2%, negative predictive value of 82.4%, and positive predictive value of 42.8%. Thus, micro-US was found to be quite accurate in excluding clinically significant prostate cancer, however, many abnormalities detected on micro-US were not clinically significant cancer. Whether this modality is able to supplant mpMRI or serve as an adjunct to guide fusion biopsies remains to be ascertained in future studies.
Presented by: Davide Maffei, MD, Department of Urology, Humanitas University, Milan, Italy
Co-authored by: Marco Paciotti, Massimo Lazzeri, Piergiuseppe Colombo, Vittorio Fasulo, Luigi Domanico, Paolo Casale, Alberto Saita, Rodolfo Hurle, Nicolo Maria Buffi, Giorgio Ferruccio Guazzoni, Giovanni Lughezzani
Written by: Christopher J.D. Wallis, Urology Resident, University of Toronto, Twitter: @WallisCJD at the American Urological Association's 2019 Annual Meeting (AUA 2019), May 3 – 6, 2019 in Chicago, Illinois

