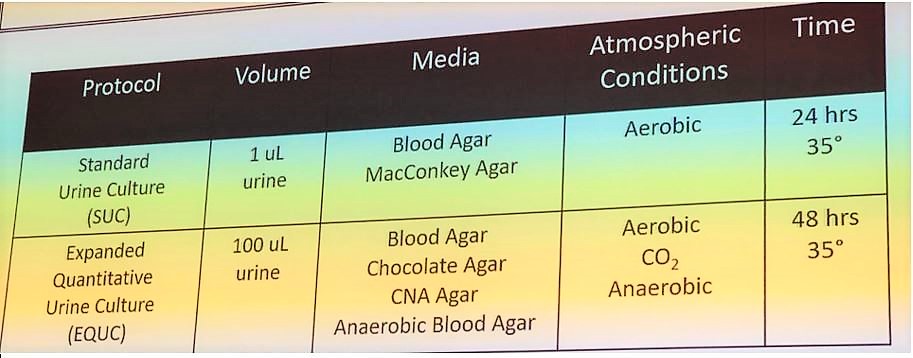
Dr. Wolfe and colleagues hypothesized that bladder wasn’t, in fact, sterile due to following reasons: the human body is a host to the millions of bacteria, other organs considered sterile were not, and most bacteria did not grow under the standard urine protocol. First, the study team analyzed urine collection techniques. They compared vaginal swabs to urine collected by catheterization, suprapubic aspirate, and mid-stream clean catch. All voided urine samples came back negative. Aspirated samples resembled catheter samples while voided urine was similar to the vaginal swab results. Aspirate bypasses vulvo-vaginal contamination and detected bacterial DNA from the bladder. Second, bacteria detection methods were studied. Many bacteria found in the bladder could be grown, but not under the standard urine protocol. Researchers developed Expanded Quantitative Urine Culture (EQUC) protocol, which differs in urine volume, media, atmospheric conditions, and time compared to the standard (Table 1).
Table 1
Novel tests confirmed that bladder microbiome exists, but there were more questions to address. Researchers were interested in what bacteria were part of normal flora. Multiple genera were identified with one type often dominating. Most common dominant bacteria of the female bladder include Lactobacillus, Gardnerella, and Streptococcus, but species span spectrum of bacterial phylogeny. Candida, Streptococcus, Staphylococcus, Gardnerella often dominate male microbiome. The bacterial composition also differs between women with and without urge urinary incontinence (UUI). For example, the presence of Lactobacillus crispatus was associated with lack of UUI (Figure 1). Other studies suggest that microbiota vary daily and can be affected by menstruation and vaginal sex.
Figure 1

The presenter noted that there is a similar association with symptoms in men. Studies demonstrate that compared to healthy men, patients with BPH/LUTS are more like to have detectable bacteria (OR: 8,03; 95% CI: 1.92-33.62). Increase in the International Prostate Index Score was associated with higher odds of bacteria detection (OR: 2.81; 95% CI: 1.34-5.92).
Presented by: Alan Wolfe, PhD, Loyola University Chicago, Chicago, Illinois
Written by: Hanna Stambakio, BS, Clinical Research Coordinator, Division of Urology, University of Pennsylvania @AStambakio at American Urological Association's 2019 Annual Meeting (AUA 2019), May 3 – 6, 2019 in Chicago, Illinois

