(UroToday.com) On the first day of the American Society for Clinical Oncology (ASCO) Genitourinary Cancer Symposium 2023 focussing on prostate cancer, Dr. Alicia Morgans presented in Poster Session A on the association between intermittent as compared to continuous androgen deprivation therapy (ADT) and cardiovascular disease and endocrine/metabolic disorders in patients with metastatic prostate cancer.
While an association between ADT and cardiovascular disease and endocrine/metabolic disorders has been relatively well characterized, there is mixed evidence on the risks of cardiovascular disease (CVD) and endocrine/metabolic disorders associated with long-term intermittent and continuous androgen deprivation therapy (iADT and cADT, respectively) for metastatic prostate cancer (mPC). Thus, these authors examined these risks in patients with mPC receiving iADT vs cADT in the US.
To do so, they performed a retrospective cohort study of SEER-Medicare patients with mPC initiating ADT (2010–2017), with ≥36 months of continuous insurance coverage, unless death occurred, who did not receive chemotherapy or a second-generation anti-androgen during follow-up. iADT and cADT cohorts were defined by treatment patterns and gaps in therapy. The authors identified comorbidities and clinical events using ICD-9/10-CM codes. Their outcomes of interest included major adverse cardiovascular events (MACE [myocardial infarction (MI), stroke, cardiomyopathy/heart failure (HF), pulmonary embolism (PE), ischemic heart disease (IHD), or all-cause mortality]) and endocrine/metabolic events (diabetes, hypercholesterolemia, bone fractures, or osteoporosis). Inverse probability of treatment weighting (IPTW) was used to adjust for differences between cohorts with weighted Cox models used to estimate the hazard ratio (HR) of the outcomes. They further performed a number of subgroup and sensitivity analyses including by restricting to those with CVD history and restricting the definition of MACE to include CVD-related mortality as a component, i.e., MACESA (MI, stroke, cardiomyopathy/HF, PE, IHD, or CVD-related mortality).
The authors included 2234 men with mPC of whom 478 (21%) received iADT and 1756 (79%) cADT. The median follow-up time was 27 and 13 months, and time on ADT (excluding gaps for iADT patients) was 24 and 19 months for the iADT and cADT cohorts, respectively.
Deaths occurred in 39% of iADT patients vs 55% of cADT patients with prostate cancer the most common cause of death in both cohorts. In adjusted analyses, patients receiving cADT had a higher risk of MACE vs iADT.
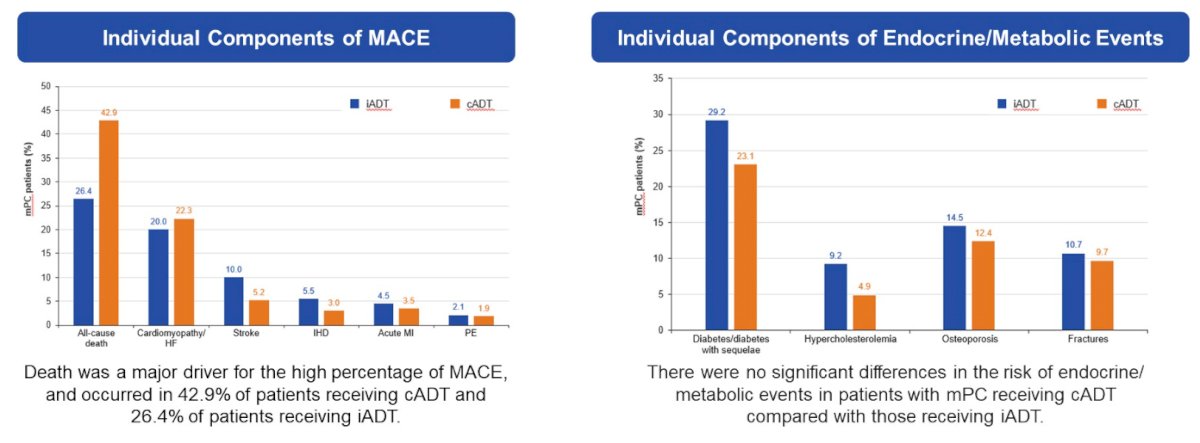
No differences in risk of endocrine/metabolic events were observed. Subgroup analysis showed that baseline history of CVD did not alter the results for MACE. Sensitivity analysis results showed no difference in risk of MACESA between patients receiving cADT vs iADT.
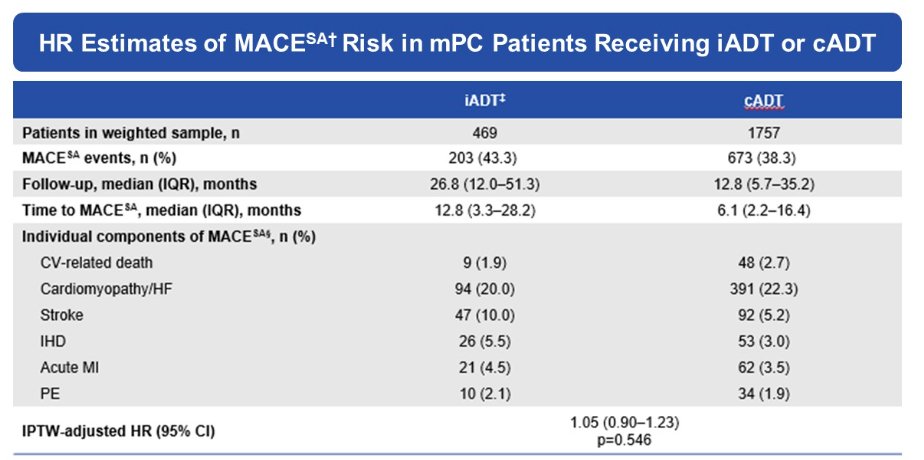
Thus, the authors concluded that, compared to those receiving iADT, patients with mPC receiving cADT had a higher risk of MACE (including all-cause mortality) but no difference in risk of endocrine/metabolic events. When MACE was restricted to include CVD-related mortality, there was no difference in risk between cohorts.
Presented by: Alicia K. Morgans, MD, MPH, Genitourinary Medical Oncologist, Medical Director of Survivorship Program at Dana-Farber Cancer Institute, Boston, Massachusetts
