(UroToday.com) The 2022 GU ASCO Annual meeting included a renal cell carcinoma (RCC) session highlighting work from Dr. Vishal Navani and colleagues presenting results from the International Metastatic RCC Database Consortium (IMDC) assessing predictors of objective response to first-line immuno-oncology combination therapies in metastatic RCC. Predictors of objective response to first-line immuno-oncology (IO) combination therapies remain elusive. Dr. Navani and investigators sought to characterize clinical variables and their association with investigator assessed the best overall response.
Using the IMDC, this study retrospectively identified patients treated with first-line ipilimumab nivolumab or approved IO/vascular endothelial growth factor (VEGF) inhibitor combinations. Patients were classified, per RECIST v1.1, as responders (complete or partial response (CR or PR)) or non-responders (stable or progressive disease (SD or PD)). The primary outcome was identification of baseline characteristics associated with real-world physician-assessed imaging response using logistic regression. Secondary outcomes were overall survival and time to next treatment.
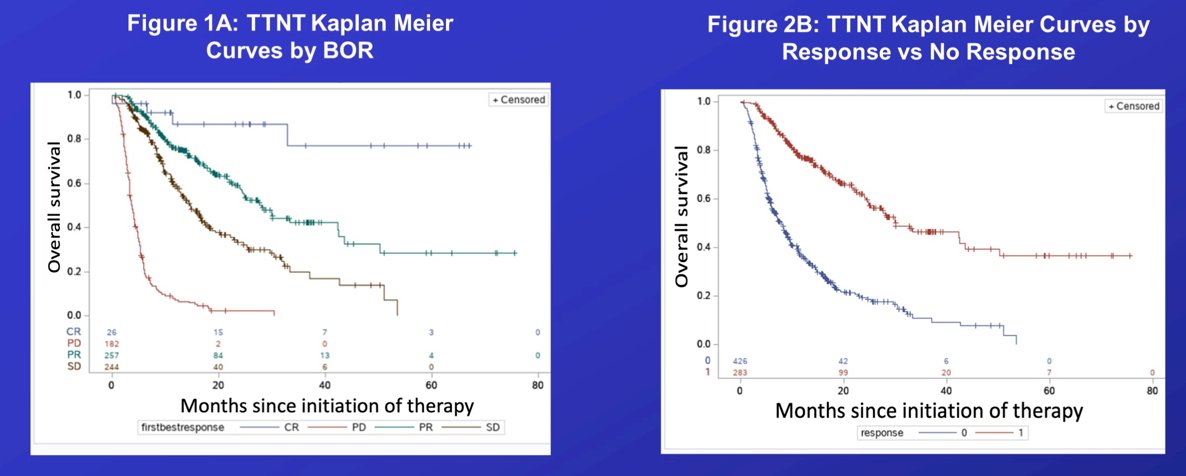
Out of 1,084 patients, 794 (73%) received ipilimumab nivolumab and 290 (27%) received IO/VEGF (axitinib + pembrolizumab, cabozantinib + nivolumab, axitinib + avelumab, lenvatinib + pembrolizumab) therapy. Favorable, intermediate and poor IMDC risk patients comprised 147 (16%), 517 (55%) and 272 (29%), respectively. Of the 898 patients with evaluable responses, 37 (4%) achieved a best response of CR, 343 (38%) PR, 315 (35%) SD and 203 (23%) PD. Corresponding median overall survival from time of first-line initiation was: not reached (CR), 55.9 (PR), 48.1 (SD), and 13 months (PD), respectively (log-rank p < 0.0001). As follows are the Kaplan-Meier curves for overall survival stratified by best overall response and response vs no response:

The following Kaplan-Meier curves highlight time to next treatment stratified by best overall response and response vs no response:
In a multivariable model, lung metastases (OR 1.71) and cytoreductive nephrectomy (OR 1.47; performed after diagnosis of metastatic disease and before first-line therapy) retained independent association with response, after adjustment for IMDC criteria. Factors not associated with response included (with univariable p values): gender (p = 0.58), age (p = 0.06), sarcomatoid histology (p = 0.99), smoking status (p = 0.39), liver (p = 0.63) and brain (p = 0.12) metastases. As in the VEGF monotherapy era, improved IMDC prognostic risk was associated with response. Results were similar when restricted to the ipilimumab nivolumab cohort.
Dr. Navani concluded his presentation assessing predictors of objective response to first-line immuno-oncology combination therapies in metastatic RCC in the IMDC with the following take-home messages:
- The presence of lung metastases, cytoreductive nephrectomy, and better IMDC risk group is associated with a higher probability of response to first-line immunotherapy combination regimens
- Further work to identify reliable predictors of response to guide treatment selection and patient counseling is warranted
Presented by: Vishal Navani, MD, Tom Baker Cancer Center, University of Calgary, Calgary, AB, Canada
Co-Authors: Matthew Scott Ernst, Connor Wells, Takeshi Yuasa, Kosuke Takemura, Frede Donskov, Naveen S. Basappa, Andrew Lachlan Schmidt, Sumanta K. Pal, Luis A Meza, Lori Wood, D. Scott Ernst, Bernadett Szabados, Rana R. McKay, Andrew James Weickhardt, Cristina Suárez, Anil Kapoor, Jae-Lyun Lee, Toni Choueiri, Daniel Yick Chin Heng
Written by: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, @zklaassen_md on Twitter during the 2022 American Society of Clinical Oncology Genitourinary (ASCO GU) Cancers Symposium, Thursday Feb 17 – Saturday Feb 19, 2022

