To further explore this, Dr. Esdaille and collaborators conducted a study to define the perioperative outcomes in a contemporary multicenter series of cytoreductive nephrectomies. They gathered information from 937 patients who underwent cytoreductive nephrectomy between 2006 and 2019 across 5 centers in the United States. They measured several variables including complications (Clavien-Dindo system), length of hospitalization, re-admission rate, blood transfusion rate, and peri-operative mortality. Patients included for analysis were mostly men (71%), with a median age of 61. 95% of patients had an ECOG performance status of 0 or 1. The median tumor size was 9.8cm, and 56.2% of patients had a tumor thrombus. With regards to IMDC risk group, 5% of patients were favorable risk, 64% were intermediate, and 31% were poor risk. This last point was commented on as suggesting that surgeons are using other criteria to select patients for nephrectomy that do not align perfectly with IMDC risk stratification.
The treatments received by patients prior to nephrectomy as shown below, with 26% of patients in the cohort receiving some sort of medical therapy prior to surgery. The majority of patients received single-agent targeted therapy (80%).
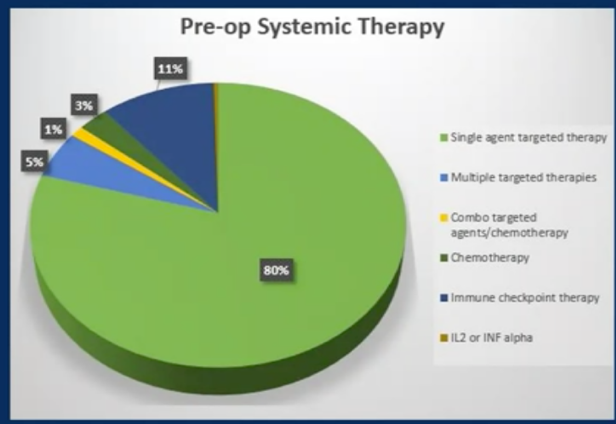
Most patients underwent open surgery, with a median operative time of 180 minutes. A third of patients received a blood transfusion, perhaps related to the baseline anemia associated with poorer risk IMDC tumors. The median length of hospitalization was 5 days, the 30-day readmission rate was 9.2%, and 30-day perioperative mortality was 1.3%. The major complication rate at 90 days was 10.1%, with only IVC thrombectomy emerging as an independent risk factor (OR 1.94, 95% CI 1.2-3.1, p < 0.006) for risk of major complications. No association was identified between major complication risk and pre-surgical systemic therapy, performance status of 2 or greater, age, open surgery, and IMDC risk group. There was no difference in surgical complication rate if patients received pre-operative immunotherapy (37% vs 34% for all complications, 9% vs 10% for major complications).
The investigators assessed the impact of nephrectomy on subsequent receipt of systemic treatment. In total, 78.7% of patients received systemic treatment within the first year of surgery, and 15.7% of patients were observed for at least 1 year without treatment. Twenty-seven patients were lost to follow-up, and 5.6% of patients died in the first year without receiving systemic therapy. This included patients with peri-operative mortality as well as those progressing rapidly such that they were not able to be treated. The median time to initiation of systemic treatment was 64 days, with a similar median time to therapy initiation regardless of surgical complication status or IMDC risk group.
Dr. Esdaille ended her presentation by summarizing that this study looked at post-surgical outcomes in patients who underwent cytoreductive surgery at 5 tertiary care centers in the US between 2006 and 2019. There was considerable patient heterogeneity in terms of systemic therapy given either before or after surgery. Overall, there was a 10% risk of major complications and a 1% risk of 30-day mortality. Pre-surgical systemic therapy was not associated with an increased risk of complication or mortality, and approximately 95% of patients were either observed or received systemic therapy in the first year after surgery.
Presented by: Ashanda R. Esdaille, MD, University of Wisconsin, Madison
Written by: Alok Tewari, MD, PhD, Medical Oncologist at the Dana-Farber Cancer Institute, during the 2021 American Society of Clinical Oncology Genitourinary Cancers Symposium (#GU21), February 11th-February 13th, 2021

