San Francisco, CA (UroToday.com) During Oral Abstract Session B: Urothelial Carcinoma; Penile, Urethral, Testicular, and Adrenal Cancers at ASCO GU 2020, Silke Gillessen, MD, presented the analysis from International Germ Cell Cancer Collaborative Group (IGCCCG). Extrapulmonary visceral metastases were the only adverse prognostic factor among 660 advanced seminomas in the original classification of the IGCCCG treated between 1975 and 1990 and published in 1997. There were multiple rationales for this update- not all patients had received cisplatin-based treatments, outcomes may have improved with current era management, and additional prognostic factors may exist.
To update the original IGCCCG classification, an international consortium (30 centers/groups) provided data on 2451 advanced seminoma patients treated with cisplatin- and etoposide-based first-line chemotherapy between 1990 and 2013 in prospective cohorts or clinical trials. There were two goals of this update: 1) To validate original IGCCCG criteria and update survival rates in a modern cohort, and, 2) To identify new prognostic factors that may explain the heterogeneity of outcomes in the original IGCCCG risk groups. The primary endpoint was progression-free survival (PFS), and the secondary endpoint was overall survival (OS).
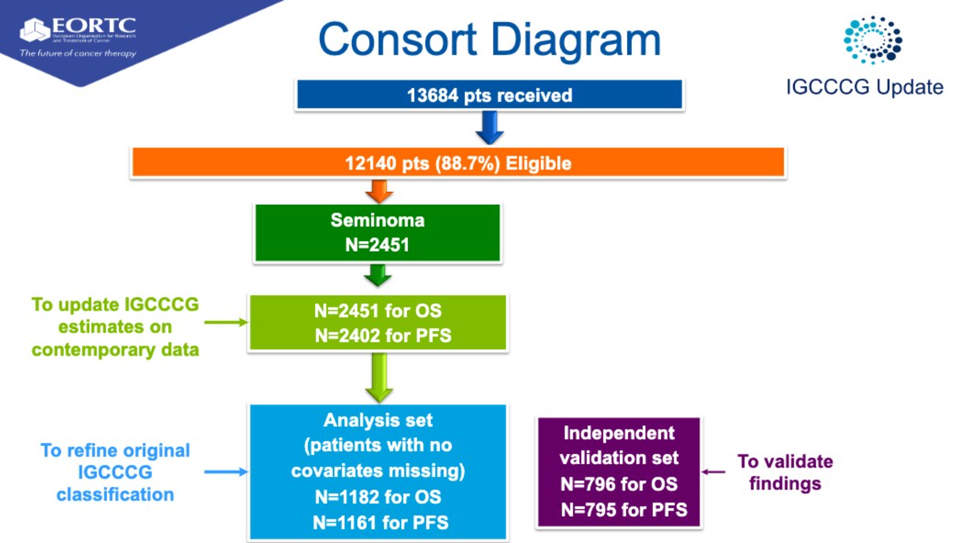
Dr. Gillessen then summarized the results of this updated analysis. Compared with the 1997 IGCCCG benchmarks, the 5-year PFS rates increased to 89 % and 79% in good and intermediate IGCCCG patients. The corresponding 5-year OS rates were 95% and 88%. Conditional forest methods analysis was used to identify prognostic factors within the original 1997 IGCCCG good risk group to refine the classification further. 1182 patients were used in the analysis set, and an independent set of 796 patients was set aside for validation. Conditional forest analysis identified LDH as the single most significant prognostic factor in good prognosis patients. 2 x ULN and 2.5 x ULN were the thresholds most often selected by the conditional tree method for LDH. 2.5 x ULN was chosen over 2 because of its higher specificity. Good risk patients with LDH above 2.5 x ULN had a worse prognosis than good-risk patients with lower LDH. PFS of good-risk patients with elevated LDH was similar to Intermediate risk patients. The difference in prognosis between the two good prognostic patient subgroups defined by LDH was confirmed in the validation set for PFS.


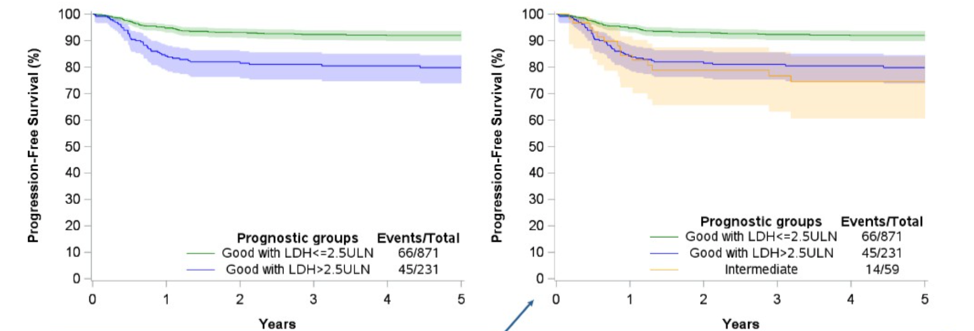
Dr. Gillessen concluded this update with a summary that noted that even in this modern era series, the original IGCCCG still correctly identified two risk groups with significantly improved PFS and OS in both risk groups. She highlighted that LDH was the single most significant prognostic factor in good prognosis patients. LDH, at a cut-off point of 2.5 x ULN further refined this classification and identified men with intermediate-risk seminoma in the absence of extrapulmonary visceral metastases. This refinement will be relevant to improve future seminoma care.
Presented by: Silke Gillessen, MD, Senior Consultant, Medical Oncology-Hematology Department, Kantonsspital St. Gallen, St. Gallen, Switzerland and Co-founder of the Advanced Prostate Cancer Consensus Conference (APCCC), previously of the University of Manchester and the NHS Christie Trust, Manchester, United Kingdom
Written by: Abhishek Srivastava, MD, Society of Urologic Oncology Fellow, Fox Chase Cancer Center, Philadelphia, PA, Twitter: @shekabhishek, at the 2020 Genitourinary Cancers Symposium, ASCO GU #GU20, February 13-15, 2020, San Francisco, California.

